
GUIDELINES
For the
Management of Moderate Acute
Malnutrition, in Ethiopia
Final version
September, 2012
ENCU/EWRD/MOARD
Addis Ababa, Ethiopia
Tel: 0115 52 35 56
e-mail: isaackm@dppc.gov.et
http://www.dppc.gov.et

Acknowledgments
The DRMFSS and Federal Ministry of Health (FMoH) would like to express its appreciation to the Emergency
Nutrition Coordination Unit (ENCU) for leading the process to develop these guidelines. We are also
grateful to the Humanitarian Response Fund (HRF) for providing the financial support required to produce
this document. These guidelines were developed by Ms. Emily Mates, an independent consultant engaged
by UNICEF with funding from the HRF.
We would like to express our appreciation to the very many people who contributed to these guidelines.
Many thanks are due to members of both the MAM Technical Working Group (TWG) and the Multi Agency
Nutrition Task Force (MANTF) in Ethiopia, who provided valuable input, comments and feedback to
improve the document.
Early Warning and Response Directorate (EWRD) of the Disaster Risk Management and Food Security
Sector, of the Ministry of Agriculture and Rural Development, Addis Ababa, Ethiopia. 2012.
ii

Table of Contents
Acknowledgments ..................................................................................................................................................... ii
Table of Contents ...................................................................................................................................................... iii
List of Boxes, Figures and Tables ........................................................................................................................... iv
List of Annexes .......................................................................................................................................................... v
Glossary of Acronyms ............................................................................................................................................... v
Definition of Terms................................................................................................................................................... vii
Introduction ................................................................................................................................................................ 1
Current health and nutrition situation in Ethiopia ...................................................................................................... 1
Current MAM situation in Ethiopia ............................................................................................................................ 2
The aim of these guidelines...................................................................................................................................... 3
Chapter 1. Overview and classification of malnutrition.......................................................................................... 4
1.1 Types of malnutrition...................................................................................................................................... 4
1.2 Causes of malnutrition ................................................................................................................................... 5
1.3 Identification of acute malnutrition using WHO growth standards (2006)....................................................... 7
1.3.1 Identification of Weight for Height Measurement (WFH) ratio using the reference tables ............................. 8
1.3.2 Identification of malnutrition using MUAC...................................................................................................... 9
1.4 Information sources that can provide information on the need to establish MAM treatment emergency
interventions ............................................................................................................................................................. 9
Chapter 2. Supplementary Feeding Interventions................................................................................................. 10
2.1 Description of supplementary feeding.......................................................................................................... 10
2.1.1 Objectives of setting up an SFP .................................................................................................................. 10
2.2 Planning the intervention ............................................................................................................................. 11
2.2.1 Staff ............................................................................................................................................................. 11
2.2.2 Supplies, equipment and transport .............................................................................................................. 11
2.2.3 Storage and Warehousing........................................................................................................................... 12
2.3 Types of Supplementary Feeding Programmes (SFPs)............................................................................... 12
2.3.1 Blanket Supplementary Feeding Programme (BSFP) ................................................................................. 13
2.3.1.1 Objectives of the BSFP ............................................................................................................................... 13
2.3.1.2 General criteria for establishing emergency BSFPs...................................................................................... 13
2.3.1.3 Case load estimation and beneficiary identification for BSFPs...................................................................... 13
2.3.1.4 Admission and discharge criteria for BSFP ................................................................................................. 14
2.3.1.5 When to Close emergency BSFPs ................................................................................................................ 14
2.3.2 Targeted Supplementary Feeding Programme (TSFP) ............................................................................... 14
2.3.2.1 Objective of the TSFP................................................................................................................................. 14
2.3.2.2 When to establish TSFPs............................................................................................................................ 15
2.3.2.3 Determining the case load for a TSFP ......................................................................................................... 15
2.3.2.4 TSFP triage, diagnosis and beneficiary selection ......................................................................................... 16
2.3.2.5 Admission criteria for TSFP ....................................................................................................................... 18
2.3.2.5.1 MAM children 6-59 months.................................................................................................................... 18
2.3.2.5.2 MAM Pregnant and Lactating Women (PLW).......................................................................................... 19
2.3.2.5.3 MAM in other vulnerable groups (admission and discharge criteria)....................................................... 20
2.3.2.6 TSFP distribution procedures at the site for new and registered beneficiaries ............................................... 20
2.3.2.6.1 Beneficiary registration ................................................................................................................... 21
2.3.2.6.2 Routine treatment ........................................................................................................................... 21
2.3.2.6.3 Follow up procedures for those already registered in TSFP .............................................................. 21
2.3.2.6.4 Transfer to OTP or inpatient unit (TFU or SC) .................................................................................. 22
2.3.2.7 Nutrition counselling and education .......................................................................................................... 22
2.3.2.8 Supplementary food ration ........................................................................................................................ 22
2.3.2.8.1 Provision of the dry ration ............................................................................................................... 22
2.3.2.8.2 Premixing the ration........................................................................................................................ 23
2.3.2.8.3 Cooking demonstrations.................................................................................................................. 23
2.3.2.8.4 Newer products for the treatment of MAM ....................................................................................... 24
2.3.2.9 Discharge criteria ..................................................................................................................................... 24
2.3.2.9.1 Discharge recovered cured .............................................................................................................. 24
2.3.2.9.2 Discharges from TSFP other than recovered cured - children 6-59 months ....................................... 25
2.3.2.9.3 Discharges from TSFP other than recovered cured - PLW ................................................................. 26
2.3.2.10 When to close the emergency TSFP ........................................................................................................ 26
iii

Chapter 3. Monitoring, reporting and coverage .................................................................................................... 27
3.1 Monitoring .................................................................................................................................................... 27
3.2 Reporting ..................................................................................................................................................... 28
3.2.1 Completing the monthly report .................................................................................................................... 28
3.2.2 Using the monthly reports to determine programme performance .............................................................. 28
3.3 Coverage ..................................................................................................................................................... 29
Chapter 4. Community mobilisation, nutrition counselling and education ....................................................... 32
4.1 Community mobilisation ............................................................................................................................... 32
4.1.1 Objectives of community mobilisation ......................................................................................................... 32
4.1.2 Information required prior to programming .................................................................................................. 33
4.1.3 Who should be involved in community mobilisation .................................................................................... 33
4.1.4 Supplies and training ................................................................................................................................... 33
4.1.5 Case finding and referral ............................................................................................................................. 34
4.1.6 Follow-up and home visits ........................................................................................................................... 34
4.2 Nutrition counselling and education ............................................................................................................. 35
4.2.1 Promotion of good hygiene at health facilities and distribution sites............................................................ 36
Chapter 5. Management of acute malnutrition in infants under-6 months (MAMI), maternal health, urban and
pastoralist issues ..................................................................................................................................................... 37
5.1 Management of acute malnutrition in infants < 6 months (MAMI) ................................................................ 37
5.1.1 Implications for Ethiopia from the MAMI project findings ............................................................................. 38
5.1.2 Identification and response.......................................................................................................................... 39
5.2 Maternal nutrition health .............................................................................................................................. 40
5.3 Urban and pastoralist issues........................................................................................................................ 41
5.3.1 Urban issues ............................................................................................................................................... 41
5.3.2 Pastoralist issues ........................................................................................................................................ 42
References................................................................................................................................................................ 43
List of Boxes, Figures and Tables
Box 1: The Productive Safety Net Programme (PSNP)....................................................................................................... 2
Box 2: Technical review of the Management of Acute Malnutrition in Infants (MAMI) Project: Current evidence, policies,
practices & programme outcomes ...................................................................................................................................... 38
Box 3: Urban issues .......................................................................................................................................................... 41
Figure 1: Types of Malnutrition............................................................................................................................................ 4
Figure 2: UNICEF conceptual framework for the determinants of nutritional status ............................................................ 6
Figure 3: The important features of warehousing and storing food commodities .............................................................. 12
Figure 4: Triage process for children 6 – 59 months screened or referred to distribution site or health facility for
Management of Acute Malnutrition (for infants 0 - 6 months, refer to SAM guidelines) .................................................. 16
Figure 5: Formulas for calculating period and point coverage........................................................................................... 30
Table 1: Target group and type of measurement .............................................................................................................. 18
Table 2: Summary of Admission Criteria for TSFP............................................................................................................ 19
Table 3: Recommendations for admission and discharge criteria for other vulnerable groups suffering from MAM ......... 20
Table 4: Summary of routine medicines for children ......................................................................................................... 21
Table 5: Summary of routine medicines for pregnant and lactating women ...................................................................... 21
Table 6: Criteria for MAM beneficiaries, discharge ‘recovered/cured’ ............................................................................... 24
Table 7: Calculation of indicators for the monthly report (example given is for Under-5 children)..................................... 29
iv

List of Annexes
Annex 1
Annex 2
Annex 3
Annex 4
Annex 5
Annex 6
Annex 7
Annex 8
Annex 9
Annex 10
Annex 11
Annex 12
Annex 13
Annex 14
Annex 15
Annex 16
Annex 17
Annex 18
Annex 19
Annex 20
Annex 21
Annex 22
Annex 23
WFH Reference Table (WHO GS 2006)
TSFP Ration Card: Children 6-59 months and PLW
Referral Slip from Community to Distribution Site
Registration Book: Children 6-59 months and PLW
TSFP Tally and Compilation Sheets
TSFP Monthly Statistics Report & How To Calculate Average Weight Gain, Length Of Stay
TSFP Supervision Checklist
Suggested Equipment and Supplies for TSFP
Stock Card
Taking Anthropometric Measurements: Oedema, MUAC, height/length and weight
WFH % of Median Reference Table (NCHS 1977) & Admission and Discharge Criteria Table
WFH z-score Reference Table for Adults and Adolescents
Referral Form Between TSFP and OTP
How to Prepare CSB
Decision Tree for Nutritional Products
Discharge Table (13%) Target Weight Gain
Discussion of 13% Weight Gain as MUAC Discharge Criteria
Home Visit Form
Post Distribution Monitoring (PDM) Questionnaire
Planning and Analysing Focus Group Discussions (FGD)
CSAS Picture Guide
Guiding Principles on IYCF in Emergencies
Warehouse Management
Glossary of Acronyms
AIDS
ANC
ASRI
BMI
BSFP
CBN
CDC
CHD
CMAM
CSAS
CSB
CTC
CVHW
DHS
DRMFSS
EHNRI
ENCU
ENA
ENI
ENN
EOS
EPI
FBF
FDA
FFI
FGD
FMHACA
FMoH
Acquired Immune Deficiency Syndrome
Ante Natal Care
Accelerated Stunting Reduction Initiative
Body Mass Index
Blanket Supplementary Feeding Programme
Community Based Nutrition
Centre for Disease Control and Prevention
Child Health Day
Community Management of Acute Malnutrition
Centric Systematic Area Sampling
Corn-Soy Blend
Community-based Therapeutic Care
Community Volunteer Health Worker
Demographic and Health Survey
Disaster Risk Management and Food Security Sector
Ethiopian Health and Nutrition Research Institute
Emergency Nutrition Coordination Unit
Essential Nutrition Actions
Emergency Nutrition Intervention
Emergency Nutrition Network
Enhanced Outreach Strategy
Expanded Programme of Immunisation
Fortified Blended Food
Food Distribution Agent
Food Fortification Initiative
Focus Group Discussion
Food, Medicine and Health Care Administration and Control Authority
Federal Ministry of Health
v

GAM
GFD
GMP
GoE
GS
HABP
HEP
HEW
HFA
HIV
HTP
IASC
IDP
IEC
IFE
IRT
ITN
IU
IUGR
IYCF
KCAL
LBW
MAM
MAMI
MDG
MoH
MUAC
NCHS
NFI
NGO
NNP
NNS
OTP
PLWHA
PLW
PSNP
RDA
RUF
RUSF
RUTF
S3M
SAM
SC
SD
SFP
SQUEAC
TB
TFP
TFU
TSFP
UNHCR
UNICEF
VAS
WASH
WFA
WFH
WFP
WHO
Global Acute Malnutrition
General Food Distribution
Growth Monitoring and Promotion
Government of Ethiopia
Growth Standards
Household Asset Building Programme
Health Extension Programme
Health Extension Worker
Height-for-Age
Human Immunodeficiency Virus
Harmonised Training Package
Inter-Agency Standing Committee
Internally Displaced Population
Information, Education and Communication
Infant Feeding in Emergencies
Integrated Refresher Training
Insecticide Treated Net
International Units
Intra Uterine Growth Retardation
Infant and Young Child Feeding
Kilocalories
Low Birth Weight
Moderate Acute Malnutrition
Management of Acute Malnutrition in Infants
Millennium Development Goal
Ministry of Health
Mid Upper Arm Circumference
National Centre for Health Statistics
Non Food Item
Non-Governmental Organisation
National Nutrition Programme
National Nutrition Strategy
Outpatient Therapeutic Programme
People Living With HIV/AIDS
Pregnant and Lactating Women
Productive Safety Net Programme
Recommended Daily Allowance
Ready-to-Use Food
Ready-to-Use Supplementary Food
Ready-to Use Therapeutic Food
Simple Spatial Survey Method
Severe Acute Malnutrition
Stabilisation Centre
Standard Deviation
Supplementary Feeding Programme
Semi-Quantitative Evaluation and Assessment of Coverage
Tuberculosis
Therapeutic Feeding Programme
Therapeutic Feeding Unit
Targeted Supplementary Feeding Programme
United Nations High Commission for Refugees
United Nations Children’s Fund
Vitamin A Supplementation
Water Sanitation and Hygiene
Weight-For-Age
Weight-For-Height
World Food Programme
World Health Organisation
vi

Definition of Terms
Acute malnutrition/ wasting - measure of “thinness” due to rapid recent weight loss.
Anthropometry - the study and technique of human body measurement. It is used to measure and monitor
nutritional status in an individual or population group. Body measurements include: age, sex, weight,
height, oedema (fluid retention) and mid upper arm circumference (MUAC).
Blanket Supplementary Feeding (BSF) - feeding of all nutritionally vulnerable population irrespective of
nutritional status.
Body Mass Index (BMI) - a number that indicates a person’s weight in proportion to height/length,
calculated as kg/m².
Caregiver – parent or guardian of the malnourished child.
Community Involvement (sometimes referred to as social or community mobilisation) - term used to
cover a range of activities that, help nutrition programme implementers (i.e. nutritionists, managers and
health workers) build a relationship with the community and encourage programme uptake by community
members.
Community-based Management of Acute Malnutrition (CMAM) - international term for timely detection
of severe acute malnutrition in the community (social mobilisation); provision of treatment for those
without medical complications with ready-to-use therapeutic foods or other nutrient-dense foods at home
(OTP) combined with a facility-based approach for those malnourished children with medical complications
(TFU or SC). In some instances/programmes the CMAM also includes TSFP activities.
Community Sensitization - a way to reach out to people in the community and teach the causes, signs and
symptoms of malnutrition, and how to seek treatment opportunities and prevent healthy children from
becoming malnourished.
Community-based Therapeutic Care (CTC) - international term used prior to the CMAM term.
Complementary Feeding - the process starting when breastmilk alone is no longer sufficient to meet the
nutritional requirements of infants and therefore other food and liquids are needed along with breastmilk.
The target age range for complementary feeding is generally 6-24 months even though breastfeeding can
continue beyond 2 years.
Crude Mortality Rate (CMR) - the rate of death in the entire population, including both sexes and all ages.
The CMR can be expressed with difference standard population denominators and for different time
periods, often commonly described as deaths per 10,000 population per month/year.
Emergency Nutrition Intervention (ENI) - programmes set-up to manage malnutrition and to provide food
to a population that does not have sufficient access to or quality of food. Emergency Nutrition
Interventions can also be started in response to other factors such as disease outbreaks in populations with
sufficient access to food.
Evaluation - a process that objectively determines appropriateness, relevance, effectiveness, efficiency and
impact of activities in light of specified objectives.
vii

Exclusive breastfeeding (EBF) - breastfeeding while giving no other food or liquid, not even water.
Recommended for infants up to the age of 6 months.
Fortified Blended Food (FBF) - a precooked mixture of cereals and other ingredients such as pulses, dried
skim milk and vegetable oil, which is fortified with micronutrients. Commonly marketed as CSB (+ and ++),
Famix or Unimix.
F-75 - Formula 75 (75kcal/100 ml) is the milk based diet recommended by WHO for the stabilisation of
children with SAM with in inpatient care (those with medical complications and/or no appetite).
F-100 - Formula 100 (100kcal/100 ml) is the milk based diet recommended by WHO for the nutrition
rehabilitation of children with SAM after stabilisation in inpatient care, now is generally replaced by RUTF.
Global Acute Malnutrition (GAM) - a population indicator that provides an aggregate of moderate and
severe malnutrition, i.e. ≤-2 Z-scores and oedema. GAM is divided into moderate and severe acute
malnutrition (GAM = MAM+SAM).
Inpatient Therapeutic Care - severely malnourished patients admitted to inpatient facility for treatment
(TFU or SC).
IYCF - describes the feeding of infants and young children (usually 0-24 months).
Kwashiorkor - bilateral pitting oedema (nutritional oedema) that is a clinical indicator for SAM. Oedema is
the excessive accumulation and abnormal infiltration of serous fluid in connective tissue or in a serous
cavity. Classified into 3 grades; + mild (both feet, can include ankles), ++ moderate (both feet, lower legs,
hands or lower arms); +++ severe (generalized oedema over whole body including arms and face).
Malnutrition - a state in which the physical function of an individual is impaired to the point where s/he
can no longer maintain adequate bodily performance processes.
Marasmic-Kwashiorkor – a combination of both maramus and kwashiorkor.
Marasmus - severe weight loss and muscle mass leaving ‘skin and bones’. Appearance can manifest as ‘old
man face’ and ‘baggy pants’.
Moderate Acute Malnutrition - description of malnutrition level; persons with MAM have higher morbidity
and mortality risks. In Ethiopia the definition encompasses children 6-59 months with < -2 to ≥-3 z-scores
and/or MUAC ≥ 11.0 to < 12.0 cm; and PLW with MUAC < 23.0 cm. For MAM classifications for infants,
older children and adults in Ethiopia, please refer to Table 3 on page 19.
Monitoring - periodic oversight of the implementation of an activity which seeks to establish the extent to
which input deliveries, work schedules and targeted outputs are proceeding according to plan.
MUAC – Low MUAC is an indicator for wasting. For a child 6-59 months, MUAC < 11.0 cm indicates severe
wasting or SAM, MUAC ≥ 11.0 to < 12.0 cm indicates moderate wasting or MAM. For PLW, MUAC < 23.0 cm
indicates MAM. For adults with HIV/AIDS (or other chronic diseases), MUAC ≥ 18.0 to < 23.0 cm indicates
MAM. MUAC is a better indicator of mortality risk associated with acute malnutrition than WFH.
NCHS/WHO Reference - the 1977 NCHS/WHO growth reference, which is based on the weights and heights
of a statistically valid population of healthy infants and children in the United States, was previously widely
used to assess, monitor and evaluate the nutritional status of individual children or groups of children.
Many countries have now moved to the use of the new WHO Growth Standards (2006), see below.
viii

Nutrition - study of food and its nutrients; its functions, actions, interactions and balance in relation to
health and disease.
Nutrition Education – process of imparting knowledge, designed to improve people’s attitude, habits,
behaviour, customs and beliefs that are related to food consumption
Outpatient Therapeutic Programme (OTP) - programme run from a health centre or health post offering
outpatient care to severely malnourished cases who have appetite and who do not have any medical
complications (this group usually represents > 90% of all the SAM cases). At admission, children receive a
medical check to determine if they warrant direct referral to the nearest inpatient TFU. If they are well
enough to be treated as an outpatient they receive systematic treatment and a ration of RUTF. Patients are
seen on a weekly or fortnightly basis, but carers are encouraged to return to the OTP if the child’s condition
deteriorates during that time. The average length of stay in OTP is 4-8 weeks.
Prevalence Rate - the proportion of the population that has the health problem under study (e.g. the
prevalence of GAM).
Ready-to Use Foods (RUFs); Ready-to use Supplementary Food (RUSF) and Ready-to Use Therapeutic
Food (RUTF) - energy dense, mineral and vitamin enriched food that does not require cooking or
preparation or dilution with water and can be eaten directly from the packet. RUTF has been specifically
developed for the recovery of severe acute malnutrition at home, while RUSF is for the recovery of
moderate acute malnutrition.
Recommended nutrient intake (RNI) - the daily intake which meets the nutrient requirements of almost all
(97.5%) apparently healthy individuals in an age- and sex-specific population.
Selective Feeding Programmes – therapeutic (for severely malnourished) and supplementary (for
moderately malnourished).
Severe Acute Malnutrition (SAM) - description of malnutrition level encompassing children 6-59 months
with < -3 z-scores, and/or MUAC < 11.0 cm, and/or bilateral pitting nutritional oedema. Persons with SAM
have higher morbidity and mortality risks.
Sphere Project - was launched in 1997 by a group of humanitarian NGOs, the Red Cross and Red Crescent
movement. The Sphere humanitarian charter and minimum standards in disaster response, 3rd edition
(2011) has just been released; providing a set of recommendations that humanitarian projects should aim
to meet.
Standard Deviation (SD) or z-score - the deviation of the anthropometric value (weight, height etc.) for an
individual from the median value of the reference population.
Stunting - or chronic undernutrition, is a form of undernutrition that is defined by a height-for-age (HFA) z-
score below two SDs of the median WHO standards. Stunting is a result of prolonged or repeated episodes
of undernutrition often starting before birth. This type of undernutrition is best addressed through
preventative maternal health programmes aimed at pregnant women, infants, and children under age 2.
Programme responses to stunting require longer-term planning and policy development.
Supplementary Feeding Programme (SFP) - provision of an additional food ration for moderately
malnourished individuals through a ‘targeted SF’; or to the most nutritionally vulnerable groups (regardless
of nutritional status) through ‘blanket SF’.
Targeting - a method of delivering goods (such as food assistance) and/or services to a selected group of
individuals or households, rather than to every individual or household in the population.
ix

Therapeutic Feeding Programme (TFP) - combination of inpatient (TFU) and outpatient (OTP) therapeutic
feeding for the treatment of severe acute malnutrition.
Therapeutic Feeding Unit (TFU) - units in hospitals and health centres offering inpatient care to the
severely malnourished cases with complications and/or lack of appetite. If OTP is not available in the
catchment area, TFU offers full inpatient care with Phase 1, Transition Phase and Phase 2 with an average
length of stay of 2-3 weeks. When OTP is available in the catchments area, only the complicated severe
cases as defined by a lack of appetite and the presence of medical complications are admitted in TFU.
Usually, patients would only stay as long as they required Phase 1 treatment (2-7 days) and then would
progress to outpatient care.
Triage of Acute Malnutrition - Refers to the selection/ sorting/classification of cases of acute malnutrition
presented to fast track treatment and increase survival rates.
Undernutrition - Is a consequence of a deficiency in nutrient intake and/or absorption in the body. The
different forms of undernutrition that can appear isolated or in combination are acute malnutrition
(bilateral pitting oedema and/or wasting), stunting, underweight (combined form of wasting and stunting),
and micronutrient deficiencies.
Underweight - Underweight is a composite form of undernutrition including elements of both stunting and
wasting and is defined by a weight-for-age (WFA) z-score below 2 SDs of the median (WHO standards). This
indicator is commonly used in growth monitoring and promotion (GMP) and child health and nutrition
programmes aimed at the prevention and treatment of undernutrition.
Vulnerable Groups – Groups of people who are ‘at risk’ of malnutrition, which vary in characteristic but are
often defined by age, sex, ethnicity and location; can also include those with disabilities and stigmatised
illnesses, such as mental ill-health and displaced persons such as refugees or migrant workers
WHO Growth Standards (WHO GS 2006) - Developed using data collected in the WHO Multicentre Growth
Reference Study in Brazil, Ghana, India, Norway, Oman, and the United States between 1997 and 2003 to
generate new curves for assessing the growth and development of children from birth to five years of age
under optimal environmental conditions. They are intended to be used to assess children everywhere,
regardless of ethnicity, socioeconomic status and type of feeding.
Z-score - Indicates how far a measurement is from the median – also known as the standard deviation (SD)
score. The reference lines on the growth charts (labelled 1, 2, 3, -1, -2, -3) are called z-score lines; they
indicate how far the measurement is above or below the median (= z-score of 0).
x

Introduction
Current health and nutrition situation in Ethiopia
Ethiopia is the third most populous country in Africa with an estimated population of 79.5 million, of which
approximately 11 million are children under-5.1 The health situation in Ethiopia is generally poor; a
reflection of widespread poverty, limited employment opportunities, low income levels, high population
pressure, low education levels (especially among women), inadequate access to clean water and sanitation,
high rates of migration and poor access to health services. The recent National Nutrition Survey (2010)
confirmed that maternal and child feeding practices and knowledge of ‘healthy behaviours’ remain at sub-
optimal levels.2
Ethiopia’s long and continuing history of food insecurity is attributed to erratic rainfall and/or the complete
failure of rains, degraded land, archaic and inefficient farming practices and regular pest infestations,
among other factors. As a result, every year millions of people in rural Ethiopia are in need of support in the
form of food aid, nutrition support, health, water supply and sanitation, shelter and other emergency
inputs. With more than 80% of the population relying on subsistence agriculture as their primary livelihood,
they are dependent on the success of two annual rainy seasons to secure nearly all their food needs for the
year. As such, they are particularly vulnerable to climatic shocks and their ability to recover from those
shocks is limited. Over the past few years some communities have faced considerable hardships, as one or
other, or both of the two annual rains have failed and pest infestation has been high, causing crop failures
across many areas of the country and intensifying the cumulative vulnerability of communities
The consequence of Ethiopia’s poor health situation, sub optimal caring practices and continuing food
insecurity (which can regularly develop into more severe food crises), is that malnutrition rates among
children remain at unacceptably high levels; the prevalence of Global Acute Malnutrition (GAM) at the
national level is estimated to be 11% (moderate and severe), with 47% of children suffering from chronic
malnutrition. By now it is very well understood that much of childhood morbidity and mortality is rooted in
malnutrition. While it is encouraging that Ethiopia’s under-5 mortality rate has decreased in recent years
from 169/1,000 to 123/1,000 live births, this figure still represents 389,000 under-5 deaths annually.3
The importance of achieving good nutritional status for vulnerable groups is fundamental, not only to avoid
the short-term consequences of increased morbidity and mortality, but also to avoid potential longer-term
economic consequences that have been identified. Undernourished infants and children, who manage to
survive may be subject to longer-term impairment. Furthermore, they are more likely to grow into shorter
adults, to have lower educational achievements and, for women, more likely to subsequently give birth to
smaller infants themselves, thus perpetuating an intergenerational cycle of undernutrition. Prevention of
maternal and child undernutrition is therefore of critical importance that will benefit not only the present
generation, but also their children.4
1 Population Projection (2010) according to the Ethiopia Census 2007. Central Statistics Agency.
2 The National Nutrition Survey, 2010. Ethiopian Health and Nutrition Research Institute.
3 Ethiopia Demographic and Health Survey, 2005. Central Statistics Agency. Preliminary results from the EDHS 2011 suggest that
the U5 mortality rate has reduced to 88/1,000 live births
4 Black, R., Allen, L. H., Bhutta, Z. A., Caulfield, L. E., De Onis, M., Ezzati, M., Mathers, C., and Rivera, J. For the Maternal and
Child Undernutrition Study Group. Maternal and child undernutrition: global and regional exposures and health consequences. The
Lancet. Published online Jan 17 2008. DOI:10.1016/S0140-6736(07)61690-0
1

In response to the continuing high levels of malnutrition, the Government of Ethiopia (GoE) developed the
National Nutrition Strategy during 2008, to be implemented through the National Nutrition Programme
(NNP). The objective is better harmonization and coordination of the various approaches to manage and
prevent malnutrition. The NNP is currently a 10 year initiative, aiming to reduce the levels of stunting,
wasting, underweight and Low Birth Weight (LBW) infants, thus contributing to Ethiopia’s efforts to reach
the relevant Millennium Development Goals (MDGs) by 2015. Its first phase spans five years (2008-2013)
and consists of two main components: a) ‘Supporting Service Delivery’ which includes ‘increased access for
the management of Severe Acute Malnutrition (SAM)’, and b) ‘Institutional Strengthening and Capacity
Building’.
In efforts to further expedite improvements in nutrition indicators, the GoE has recently developed a
number of initiatives to combat malnutrition and work toward reaching the MDGs, which include the
Accelerated Stunting Reduction Initiative (ASRI), Food Fortification Initiative (FFI) and enhancing linkages
between the NNP and the Productive Safety Net Programme (PSNP).
Box 1: The Productive Safety Net Programme (PSNP)
The PSNP focuses support continuously on selected households over several years and has an
explicit objective of beneficiaries eventually graduating. The PSNP is the largest social safety
net programme in Sub-Saharan Africa with plans for it to be complemented by the Household
Asset Building Programme (HABP)
The PSNP is currently reaching 7.57 million chronically food insecure people through two
components: public works (80%) and direct support (20%). This remuneration enables
households to meet their food gaps (through provision of food or cash), in order that they are
not forced to sell productive assets, when faced with periodic food shortages or other shocks.
Current MAM situation in Ethiopia
The 2005 Demographic and Health Survey (DHS) identified that 11% of children 6-59 months in Ethiopia
were wasted; a situation that has remained unchanged since the first DHS conducted in 2000. A number of
approaches have been employed over recent years to address MAM, summarised below.
MAM in Ethiopia is currently detected and treated via three food-based programmes:
1. The Ethiopian government has been implementing the Enhanced Outreach Strategy Targeted
Supplementary Feeding (EOS/TSF) programme or Child Health Days (CHD), which conducts
screening exercises (6-monthly and 3-monthly, respectively) in 168 chronically food insecure
woredas and includes provision of TSF rations for identified MAM individuals. Selected beneficiaries
[drawn from under-5 children and Pregnant and Lactating Women (PLW)] are issued with a ration
card that is presented to receive 3-monthly TSFP rations. In addition to screening, additional
promotive/preventative services are provided every 6 months, of vitamin A supplementation (VAS)
and de-worming. The EOS is in the process of transitioning into the activities of the routine CHDs
that are managed by the Health Extension Workers (HEWs) every 3 months; as such MAM
treatment will be provided as part of routine health services in food insecure areas of the country.
2. During times of deteriorating and/or acute nutritional situations (as defined and guided by the
DRMFSS 'hot-spot' classification of woredas as food insecure, with raised malnutrition rates), a
smaller MAM caseload is detected and treated, usually through Non-Governmental Organisations
(NGOs) Targeted Supplementary Feeding Programmes (TSFPs), set up in selected woredas. These
programmes act as a complement to on-going Therapeutic Feeding Programmes (TFPs). The TSFPs
2

are characterised by rigorous nutritional monitoring, active case finding and usually bi-weekly
distributions. However, it is important to note that these NGO TSFPs are generally short-term
operations and have limited coverage across this vast country.
3. While not identified by their nutritional status, young children and pregnant women are included in
beneficiary lists of communities receiving relief food to benefit from an extra ration of highly
fortified Corn Soya Blend (CSB)5. This intervention is embedded in the DRMFSS sector of the
Ministry of Agriculture and is also addressing MAM to some extent.6
While we know that MAM treatment programmes work, there is considerable interest to move away from
the ‘food bias’ when treating MAM and the international community has been raising questions about the
effectiveness of traditional SFPs.7 However, as yet there is limited evidence available for what type of non-
food interventions might be most appropriate to both prevent and treat MAM in the Ethiopian context. In
some countries, cash transfers are being targeted to malnourished populations, although it is recognised
that this alternative might need to be piloted in the Ethiopian context alongside the ongoing
implementation of the PSNP, which already provides cash transfers to large sections of the population.
Additionally, cash transfers intended to treat MAM could face some challenges in areas of Ethiopia, where
there might be limited purchasing availability in the markets for sufficiently nutritious food.
Due to the interest in other (and potentially more effective) approaches, some organisations are currently
reviewing traditional SFP programming e.g. the Centre for Disease Control (CDC) ‘grey literature’ review
and the University of Westminster and Emergency Nutrition Network (ENN) review of evidence for the
effectiveness of interventions during emergencies. It is possible that ‘new and improved’ thinking or
alternative methods of programming might be proposed in the near future. It is therefore recommended
that these guidelines are viewed as ‘living document’, subject to revision as new evidence and best
practices emerge.
The aim of these guidelines
These guidelines are intended for use by all health and nutrition staff from government, agencies and
organisations involved in nutrition related activities in Ethiopia. The purpose of the guideline is to define
basic concepts and criteria related to the planning, implementation, monitoring and evaluation of
nutritional interventions aimed at treating and/or preventing Moderate Acute Malnutrition (MAM) and to
describe locally appropriate and internationally acceptable standards for MAM treatment programmes, as
well as overall intervention management.
These guidelines focus on the implementation of Supplementary Feeding Programmes (SFPs) in emergency
contexts, to complement the programme implementation manual of the EOS/TSF that guides the ongoing
programmes to identify and treat MAM. They also highlight the importance of increased awareness of
infant and Young Child Feeding (IYCF) and maternal nutrition; in order to reduce the incidence of MAM in
Ethiopia through comprehensive programming, as outlined in Ethiopia’s National Nutrition Programme
(NNP). In response to requests from the MAM TWG to provide the latest international information, at times
these guidelines veer from technical guidance on known interventions, to discussion of some of the
outstanding questions that are arising during the implementation of programmes to address MAM.
These guidelines should be used in conjunction with the Emergency Nutrition Intervention (ENI) Guideline,
2011, and the Guidelines for the Treatment of Severe Acute Malnutrition (SAM) in Ethiopia, 2007, endorsed
by the Ministry of Health.8
5 The more enriched product of CSB+ is known as ‘super cereal’. CSB++ is now known as ‘super cereal plus’
6 Concept note for the Management of MAM. Ethiopian Federal Ministry of Health, 2010.
7 Navarro-Colorado, C., Shoham, J., Mason, F. Measuring the effectiveness of Supplementary Feeding Programmes in Emergencies.
Working Paper HPN Network Papers 63, August 2008.
8 Protocol for the Management of Severe Acute Malnutrition, Ethiopia, Federal Ministry of Health (FMoH), March 2007.
3
Chapter 1. Overview and classification of malnutrition
1.1 Types of malnutrition
The nutritional requirements of individuals vary at different stages of life and depend on a number of
factors including age, sex and current health status of the individual. Nutritional requirements will also
depend on:
differing physiological conditions, such as pregnancy and breastfeeding
environmental conditions, such as temperature
varying levels of physical activity
There are two categories of nutrients needed by the body:
1. Macronutrients - that provide the energy required for growth and replacement of cells, which are
required in large amounts and include protein, carbohydrate and fat
2. Micronutrients - which ensure the healthy functioning of organs and body processes. These are
required in much smaller amounts and include vitamins and minerals
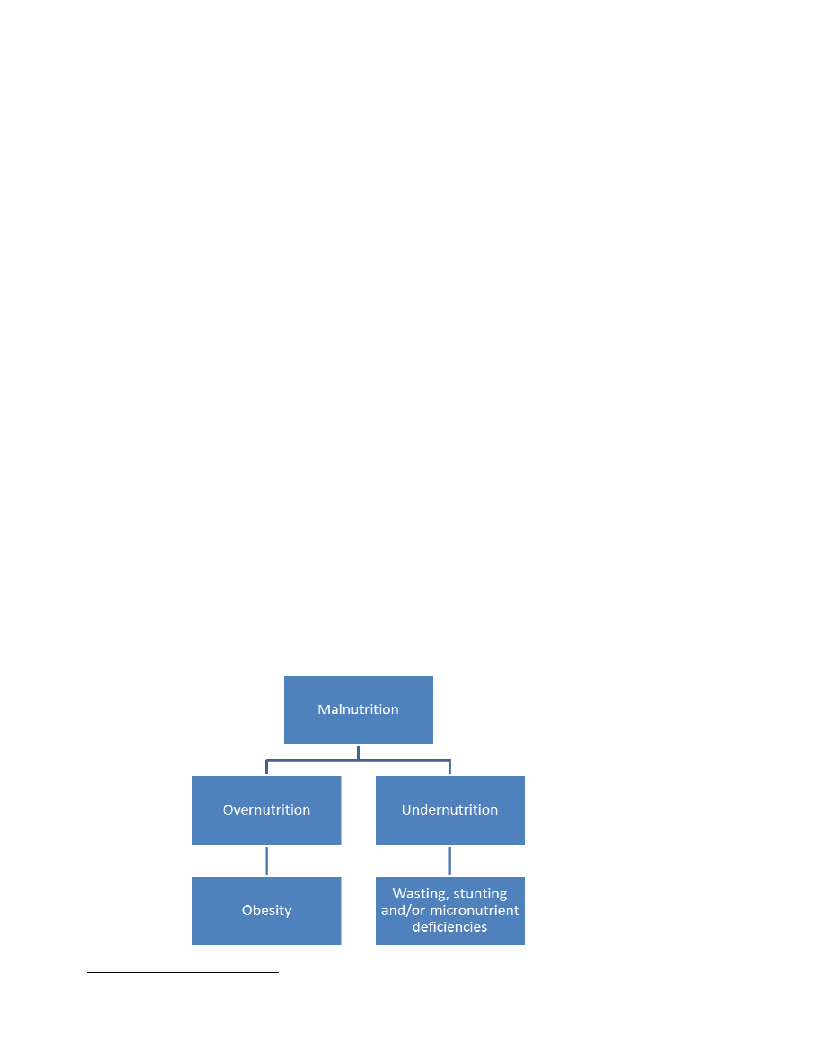
Malnutrition can exist in two forms as outlined in Figure 1 below; overnutrition and undernutrition.9 In
Ethiopia the most common form of malnutrition is undernutrition, which can manifest as wasting, stunting
and/or deficiencies of essential vitamins and minerals (collectively referred to as micronutrients).
Undernutrition generally results from a complex web of interactions, from the molecular and
microbiological level of the individual, to the cultural and socioeconomic features of societies.10
Figure 1: Types of Malnutrition
9 In this guideline unless otherwise indicated, the term ‘malnutrition’ refers to undernutrition in the form of wasting.
10 Heikens, G. T., Amadi, B. C., Manary, M., Tollins, N., and Tomkins, A. Nutrition interventions need improved operational
capacity. The Lancet. Published online Jan 17 2008. DOI:10.1016/S0140-6736(07)61690-0
4

The three main types of undernutrition are known as acute malnutrition (wasting), chronic malnutrition
(stunting) and micronutrient deficiency.
1. Chronic malnutrition or ‘stunting’ (individuals whose height is below the average expected height
for their age) - is generally a result of prolonged or repeated episodes of undernutrition that often
starts before birth. Stunting is strongly associated with poverty, poor health and impaired physical
and mental development. Stunting can be reversed through ‘catch up growth’ until 2 years of age;
after which it is irreversible.
2. Acute malnutrition or ‘wasting’ [a measure of thinness defined by Weight-For-Height (WFH) or Mid
Upper Arm Circumference (MUAC) measurements] - is characterized by rapid weight loss usually
due to illness and/or reduced food intake. Wasting can be reversed, however it is of particular
concern during emergency situations because it can quickly lead to excess morbidity and mortality.
Acute malnutrition leads to changes in the body related to cellular composition, tissue and organ
functions. Acute malnutrition can either present itself as severe or moderate and can result from
type II nutrient deficiencies (see below)
3. Micronutrient deficiencies - individuals can have a deficiency of either Type I or type II nutrients.
a. Type I nutrients are those required for adequate functioning of the body, such as iron,
vitamin A, iodine, etc. These nutrients regulate hormonal, immunological, biochemical and
other bodily processes. While these deficiencies can cause major illness and increased risk
of mortality, anthropometric measurements (e.g. height and weight) can be normal,
although it is common for stunted or wasted individuals to also have some degree of
micronutrient deficiency.
b. Type II nutrients are the growth nutrients required to build new tissue e.g. nitrogen,
essential amino-acids, potassium, magnesium, sulphur, phosphorus, zinc, sodium, etc.
Deficiencies will result in the failure to grow, to repair tissue that is damaged, to replace
cells that rapidly turn-over (e.g. intestine and immune cells) or to gain weight after an
illness, which can lead to an increase in the risk of stunting and/or wasting.
1.2 Causes of malnutrition
Figure 2 below describes the three layers of the determinants of nutritional status;
1. Immediate - which act on the individual
2. Underlying - which influence households and communities
3. Basic - which act on entire societies
5
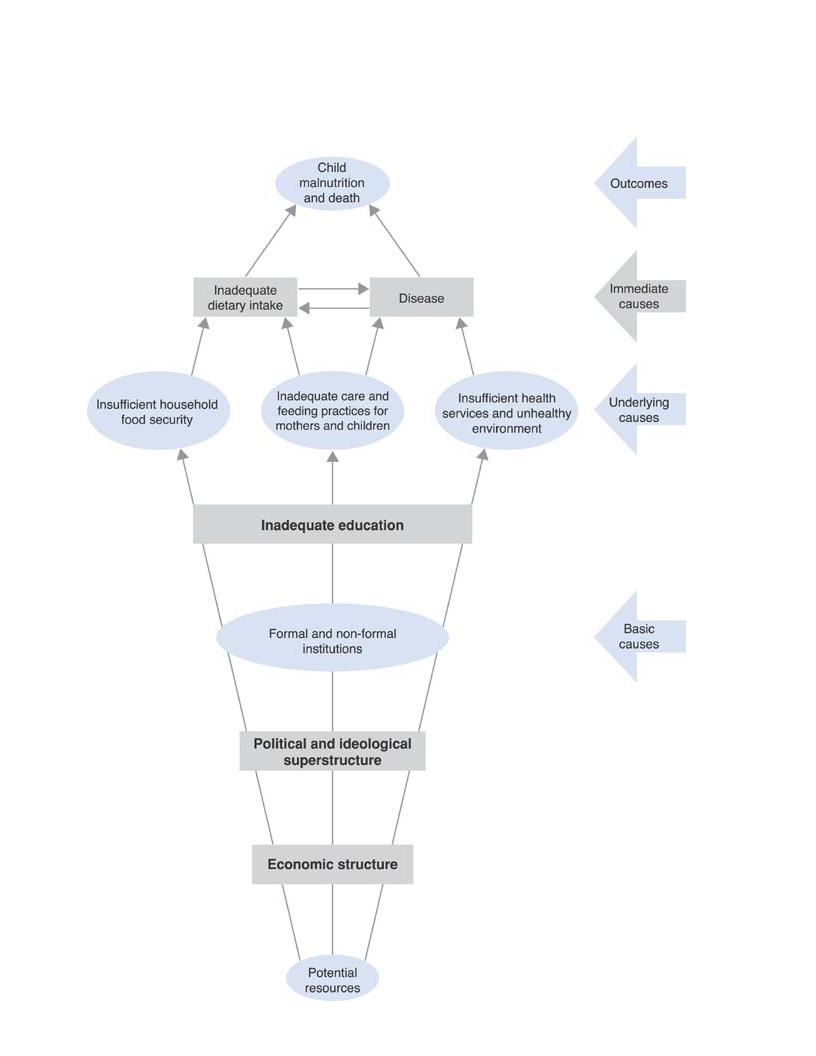
Figure 2: UNICEF conceptual framework for the determinants of nutritional status
6

1. Immediate Causes
These include inadequate dietary intake and infection or disease. Malnutrition is often exacerbated by
a vicious cycle between these two factors. Inadequate food intake can lead to a higher risk of infection
or disease, and conversely disease can lead to inadequate food intake. In the Lancet series (2008) Black
et al, summarised the effects of the deadly relationship between infection and undernutrition by
stating that:
“substantially more children die as a result of the synergy between infectious diseases and
undernutrition than from the direct sequelae of the nutritional conditions themselves.” 11
Nine out of ten child deaths in Ethiopia are due to only five conditions: pneumonia, malaria, diarrhoea,
neonatal problems and measles. Approximately 57% of these deaths are related to a weak physical
state due to malnutrition (three-quarters of these deaths result from mild to moderate malnutrition).12
2. Underlying Causes
The main underlying causes of malnutrition include shocks, such as drought, flooding, etc.; household
food insecurity, inadequate social and care environment, inadequate access to health services and
environmental factors, such as poor water and sanitation facilities.
3. Basic Causes
The basic causes of malnutrition include the country’s social, economic and political situation, for
example, the formulation and implementation of policies to address issues such as lack of capital
(financial, human, physical, social, agro-ecological, technical).
1.3 Identification of acute malnutrition using WHO growth
standards (2006)
The World Health Organisation (WHO) undertook a comprehensive survey in the early 1990’s to review the
existing National Centre for Health Statistics (NCHS) 1977 reference values and develop more appropriate
standards for use with a wider range of children from a variety of ethnic backgrounds, in developing and
developed countries. The outcome of this survey was the development of new growth standards that
describe how children should grow when their nutritional needs are fully met. These child growth standards
support the notion that given the same environmental conditions, growth potential is independent of
ethnic origin; therefore these standards can apply in any country.
The new growth standards use the same cut-off points for weight-for-height, weight-for-age, and height-
for-age z-scores, although the international recommendations for cut-off points for mid-upper arm
circumference (MUAC) measurement was increased from a MUAC <11cm to <11.5cm for SAM diagnosis.
The MUAC cut-off for MAM diagnosis remained the same at <12.5 cm.13
11 Black, R., Allen, L. H., Bhutta, Z. A., Caulfield, L. E., De Onis, M., Ezzati, M., Mathers, C., and Rivera, J. For the Maternal and
Child Undernutrition Study Group. Maternal and child undernutrition: global and regional exposures and health consequences. The
Lancet. Published online Jan 17 2008. DOI:10.1016/S0140-6736(07)61690-0
12 UNICEF and IFPRI coordinated effort, 2005. An Assessment of the causes of Malnutrition in Ethiopia: A contribution to the
formulation of a National Nutrition Strategy for Ethiopia (Background Papers)
13The FMoH has endorsed the MUAC cut-offs for children 6-59 months in Ethiopia as follows: SAM < 11.0 cm;
MAM ≥11.0 to < 12.0 cm. See section 2.3.2.5 for further details of admission criteria
7

Studies have shown that the changes in growth standards and cut-off points have potential implications on
the numbers of children eligible for admission to selective feeding programmes (especially for SAM, to a
lesser degree for MAM).14 15 16 It is therefore advisable to introduce them systematically so as not to
overload the system. With the introduction of the new growth standards, intense nation-wide training
should be conducted for all staff involved in the treatment of acute malnutrition.
When adopting the new growth standards, selective feeding programmes must be prepared for an increase
in case load by ensuring:
• Staff numbers in health facilities are adequate
• Facility staff are trained on MAM procedures, reporting, stock management, etc.
• Stock capacity at federal, regional, zonal and woreda levels are secured to prevent pipeline
ruptures
1.3.1 Identification of Weight for Height Measurement (WFH) ratio using
the reference tables
When a child's WFH is assessed, the child's weight is being compared to a reference weight for a child of
the same height. The reference weights for each height are known as the WHO reference values. The
reference values are used to assess or compare individual or population nutritional status.
The method by which a child or group of children is compared to the reference is known as "standard
deviation (SD)" or more commonly, "z-score". The z-score or SD describes how far a child's weight is from
the median weight of a child at the same height in the reference population.
The z-score is a more sensitive descriptor than either "percentiles" or "percentage of the median" so its use
implies that more children who are actually malnourished are identified. In addition to MUAC
measurements, to assess malnutrition, z-score or SD is used.17
For assessment of malnutrition in adolescents or adults, see section 2.3.2.5.3.
Health workers should use the WFH Reference Tables
for Girls and Boys in annex 1 to quickly identify if a child
is acutely malnourished or not.
14 Myatt, M., and Duffield, A. (2007) Assessing the impact of the introduction of the World Health Organisation (WHO) growth
standards on the measured prevalence of acute malnutrition and the number of children eligible for admission to emergency feeding
programmes. Background paper
15 de Onis, M., Onyango, A. W., Borghi, E., Garza, C., Yang, H. (2006) Comparison of the World Health Organisation (WHO) child
growth standards and the National Centre for Health Statistics/WHO international growth reference: implications for child health
programmes. Public Health Nutrition 9: 942-947
16 Seal, A., and Kerac, M. (2007) Operational implications of using the 2006 World Health Organisation growth standards in
nutrition programmes: secondary data analysis. British Medical Journal. DOI:10.1136
17 For programmes that are not yet implementing the WHO GS (2006), instead are using NCHS (1977) ‘percentage of the median’
reference values, the WFH reference tables are provided in annex 11.
8

1.3.2 Identification of malnutrition using MUAC
MAM in children 6-59 months (girls and boys) is
classified as a MUAC measurement of
≥ 11.0 to < 12.0 cm
MUAC tapes are portable, simple to use with minimal training and the colour coding ensures that
beneficiaries (or their caregivers) can easily understand why they have been included in a programme, or
not. MUAC is also the best predictor of mortality, an important fact for any child survival programme.18
However, the accuracy of MUAC measurements [especially those taken during the Enhanced Outreach
Strategy (EOS) nutrition screening] has frequently been questioned. Poor measurements can result in poor
targeting of the nutrition intervention, that is, inclusion of children in the TSFP who may not need nutrition
support and/or exclusion of children who do need nutrition support.
Problems generally arise with insufficient monitoring of programmes; food is a valuable commodity, and it
is all too easy to pull the MUAC tape a ‘bit tight’ to ensure the individual is included in the programme,
particularly if the measurer is under some pressure to include them (e.g. they are known personally to the
worker conducting the screening). It is therefore extremely important to ensure that the measurements are
taken accurately at health facilities or distribution sites, to ensure that only those individuals who fit the
admission criteria and can be admitted to the programme.
1.4 Information sources that can provide information on the need
to establish MAM treatment emergency interventions
MAM is treated in food insecure areas of Ethiopia through routine ongoing activities, such as the TSF/EOS
(as part of the quarterly CHD activities, refer to EOS/TSF implementation manual). However, in times of
heightened food insecurity emergency nutrition interventions might be required. For further information
on sources that can provide evidence on the need to establish emergency nutrition interventions, please
refer to the Ethiopia Emergency Nutrition Intervention (ENI) guideline, 2011.
18 Myatt, M., Khara, T., and Collins, S. A review of methods to detect cases of severely malnourished children in the community for
admission into community-based therapeutic programmes. Food and Nutrition Bulletin. Vol 27. No 3 (Suppl). 2006:S7-23.
9

Chapter 2. Supplementary Feeding Interventions
2.1 Description of supplementary feeding
At present the most common interventions for the management of MAM are Supplementary Feeding
Programmes (SFP). Supplementary feeding is the provision of nutritious rations to vulnerable children
(usually classified at < 5 years) or those with special dietary needs (e.g. pregnant and lactating women,
individuals with HIV/AIDS, etc.). SFPs also provide vital links to ongoing SAM treatment programmes. In
most situations, SFPs are implemented in order to prevent excess mortality among vulnerable groups. SFPs
can either be blanket or targeted and aim to supplement the energy and nutrients missing from the diet
due to various reasons.
During emergency situations, SFPs should be a short-term measure and not necessarily be seen as a means
of compensating for inadequate household food security.19 A significant and continued reduction in the
prevalence of malnutrition is likely only if an SFP is implemented alongside adequate General Food
Distributions (GFD), and/or is well aligned with the PSNP. The recently endorsed National Guidelines on
Targeting Relief Food Assistance (2011) states:
“In areas where nutritionally-targeted interventions such as TSF or CMAM are in operation, the
households of individuals who are registered for such nutritional support should automatically be
included in the registration for GFD. That is, current acute malnutrition should be an inclusion criterion
for general rations. All international experience shows that supplementary feeding is only effective
when the household has adequate access to basic foods.
In PSNP woredas, similarly, no household should be excluded from nutritional programmes (e.g. TSF,
CMAM or BSFP) on the grounds that they are already receiving support from the PSNP. Overlaps
between these programmes at the household level are desirable and represent effective targeting of
complementary assistance types.”20
2.1.1 Objectives of setting up an SFP
It is vital that the objectives of commencing and setting up the programme are well defined at the start of
the programme and are understood by all partners.
1. To reduce the risk of mortality and morbidity associated with MAM
2. To rehabilitate at-risk individuals to prevent deterioration into MAM (blanket SFP) and moderately
malnourished individuals to prevent deterioration into SAM (targeted SFP)
3. To provide a ‘protection ration’ for individuals discharged from therapeutic feeding programmes
and thus prevent relapse into SAM
4. To rehabilitate PLW who are at-risk or moderately malnourished to improve maternal nutritional
status and minimise the risk of infants born with low birth weight
5. To provide nutritional/health education messages for beneficiaries or caregivers and hence
increase awareness on optimal child feeding practices and appropriate health seeking behaviours
19 A toolkit for addressing nutrition in emergency situations. IASC Global Nutrition Cluster, UNICEF, New York, NY, 2008
20 National Guidelines on Targeting Relief Food Assistance. Ministry of Agriculture (Disaster Risk Management and Food Security
Sector), Addis Ababa, Ethiopia, 2011
10

2.2 Planning the intervention
MAM is treated in food insecure areas of Ethiopia through routine ongoing activities, such as the TSF/EOS
(as part of the quarterly CHD activities). However, in times of heightened food insecurity emergency
nutrition interventions might be required.
Prior to any emergency intervention, discussion must be held with local authorities to discuss and
determine the methodology, size, location and other important features of the proposed programme.
Wherever possible, programmes must be run within existing health structures/facilities. SFPs are usually
implemented through a large number of decentralised sites, the number of which will depend on the area,
terrain, density of population, expected number of beneficiaries, etc. The exit strategy of any programme
must be clearly identified and communicated prior to implementation.
2.2.1 Staff
The routine treatment of MAM through the EOS/TSF is currently managed at community level during the
quarterly CHDs by the HEWs, with support from the Food Distribution Agents (FDAs).
During times of heightened food insecurity, emergency SFPs might be needed. When these programmes
are required, it is vital to discuss the aims and objectives of the programme with local officials from the
start, such as woreda Administrators. It is also essential to have local authority representatives, e.g. kebele
Chairpersons, attending distribution activities in order to ensure that the operation runs smoothly and to
facilitate liaison with the community. Local government personnel are essential for good communication
between programme implementers and the community, for example, clarity regarding which vulnerable
groups the programme is targeting, passing messages for which days distributions will be held, any changes
to the schedule, etc.
Emergency SFPs are encouraged to use whatever capacity is already present in the community e.g. existing
FDAs, who will have prior knowledge and experience with screening, health education, etc. Additional
numbers and types of programme staff will depend on the size of the planned programme and projected
case-loads.
For emergency SFPs, key positions may include;
1. Overall Programme Manager
2. Health workers available to conduct triage and provide medical checks for beneficiaries
3. Supervisor
4. Distribution staff; registrar, measurers, food mixers, health educators and demonstrators, guards
5. Store keeper
6. Outreach workers/community mobilisers for screening, mobilisation and follow-up activities (see
section 3.1)
2.2.2 Supplies, equipment and transport
The size of the area and number of beneficiaries expected for the SFP will determine the amount of
materials, equipment, food and other items that are required.
The minimum supply requirements for an emergency SFP may include:
1. Food commodities; Fortified Blended Food (FBF), oil, sugar and/or other products to treat MAM
(see section 2.3.2.8)
2. Routine and other common drugs and vitamin supplements (see section 2.3.2.6.2)
11

3. Monitoring materials; ration cards, bracelets, referral slips, registration books, reporting formats,
supervision formats (see annex 2, 3, 4, 5, 6, 7)
4. Anthropometric equipment; salter scale or electronic scales, height/length boards, MUAC tapes,
WFH reference tables in z-scores (see annex 1, 8)
5. Non-Food Items (NFIs); shelter, soap for washing hands and utensils, clean water, cups, spoons,
cooking demonstration equipment, tables, chairs/benches (see annex 8)
6. Documentation; Information, Education and Communication (IEC) materials, training materials,
National Guidelines, job aids, field guides (e.g. CSB+, RUSF usage), pictorial information for
beneficiaries outlining what they can expect at the site, such as ration entitlements, etc.
7. Sufficient transport must be available to effectively implement the programme; to ensure
uninterrupted product supply chains and to move staff around, as necessary
2.2.3 Storage and Warehousing
Figure 3: The important features of warehousing and storing food commodities
(Source - adapted from the Somalia MAM guidelines, 2009)
• Products should be stored 40 cm off the wall and 10 cm off
the floor. Food commodities like CSB should be stored on
pallets to prevent weevil infestation/ contamination. Food
commodities should be protected from rodent infestation
• Food products should be stored separately from other
commodities, e.g. medicines or stationary
• Bags must not lie directly on the floor. Stacks of bags should
be no more than 2 m high
• Separate damaged bags/boxes. Record and report any
damage that occurs
• Keep an inventory of all the items in the store; a record list
should indicate name of item, quantity, date received, date
dispatched, from whom, by whom, balance and expiring
dates. It is helpful to have a Stock Control System, using the
‘first in, first out’ storage strategy (but also considering the
expiry date; goods with earlier expiry dates should be used
first). See annex 9 for sample stock card and annex 23 for
tips on good warehouse management (supplied by WFP)
2.3 Types of Supplementary Feeding Programmes (SFPs)
There are two types of SFPs: Blanket or Targeted.
(Source – adapted from UNHCR/WFP Selective Feeding Guidelines, 2009)
The key difference between the two types of SFP is that:
• Targeted SFP target and treat moderately malnourished individuals;
while
• Blanket SFP has a more preventative role, targeting all those in ‘at risk
groups’ irrespective of nutritional status
12

2.3.1 Blanket Supplementary Feeding Programme (BSFP)
A BSFP is a temporary distribution of a supplementary ration to all members of a specified at-risk group
(e.g. all children <5 years, or all PLW, or people with chronic diseases), whether they are suffering from
MAM, or not. BSFPs are generally implemented in a specified geographical area e.g. a camp or woreda.
2.3.1.1 Objectives of the BSFP
BSFPs are implemented at population level, therefore their objectives are primarily preventative. BSFPs aim
to prevent deterioration in the nutritional status of a population, to reduce the potential prevalence of
acute malnutrition and micronutrient deficiency in order to reduce excess morbidity and mortality among
those at-risk, through the provision of a food/micronutrient supplement.
BSFPs can act as a very effective measure to stabilise rapidly deteriorating situations (e.g. very high GAM
levels, during outbreaks or epidemics of infectious diseases, etc.), or they may act as a short term measure
during a seasonal hunger gap. BSFPs are usually implemented alongside a GFD, or can be implemented as a
‘stop-gap’ measure until sufficient GFD can be established.
BSFPs provide a fortified food supplement for all members of the identified vulnerable group. The
availability of resources will dictate the scope of the target group, for example, under-24 months, under-36
months, under-60 months, PLW, etc. Where resources are limited, the priority is usually to ensure full
coverage of children 6-23 months in a defined geographical area.
While anthropometric status is not measured or monitored during BSFPs, staff are encouraged to conduct
anthropometric screening wherever possible, in order to facilitate the correct referrals of persons with
MAM and SAM. As targeted supplementary feeding programmes and BSFPs are not implemented
concurrently, emphasis must be placed on the referral of identified SAM children for further assessments of
complications and appropriate treatment.
All registered beneficiaries receive the same nutritional support over a fixed period of time (e.g. 2 months).
Individual measurements are not usually recorded; therefore it is not possible for BSFPs to quantify
individual outcomes.21
2.3.1.2 General criteria for establishing emergency BSFPs
Refer to the Ethiopia ENI guideline, 2011.
2.3.1.3 Case load estimation and beneficiary identification for BSFPs
Where no definitive population data exists, programme staff should discuss with relevant authorities
(woreda offices, health facilities and local leaders) to establish the population size for the area. Numbers of
potential beneficiaries within the defined groups (e.g. children < 2 years) can then be estimated. Where
population data cannot be obtained from local authorities, other information should be sourced that can
provide the ‘best guess’, for example, use of recent DHS or any other surveys/campaigns conducted in the
area.
21 Harmonised Training Package. Module 12: Management of MAM, technical notes, version 2: 2011.
http://www.ennonline.net/pool/files/ife/management-of-moderate-acute-malnutrition-technical-notes.pdf
13

At community level, beneficiaries that fall within the defined group must then be identified, for example,
children 6 - 23 months or 6 - 59 months (less than 87 cm or 110 cm in height, respectively). This can be
done through the passing of information via local sources, for example, calling the population to come to a
certain area on a certain day to be registered for the programme.
Depending on the seriousness of the situation and in discussion with local and regional authorities, it may
be decided to include other vulnerable groups in a BSFP,22 for example;
All PLW
All adults showing signs of malnutrition
Older persons
Those with a disability
Where possible, effort should be made to provide Vitamin A supplements and deworming tablets during
contact points with the children on distribution days. Where appropriate and resources allow, other
interventions could also complement the BSFP distribution mechanism, such as distribution of Insecticide
Treated Nets (ITNs), water purification tablets, etc. It is important to focus on nutrition, health and hygiene
sensitisation during any contact points with beneficiaries. Appropriate IEC material should be
disseminated/broadcasted.
2.3.1.4 Admission and discharge criteria for BSFP
Admission and discharge criteria for BSFPs do not rely on anthropometric indicators. Once the targeted
groups have been defined, those that meet the criteria are admitted (e.g. children aged 6 - 23 months).
After a specific time period or when the BSFP is closed, they are ‘discharged’.
2.3.1.5 When to Close emergency BSFPs
Refer to the Ethiopia ENI guideline, 2011.
2.3.2 Targeted Supplementary Feeding Programme (TSFP)
2.3.2.1 Objective of the TSFP
The Targeted Supplementary Feeding Programme (TSFP) aims to rehabilitate moderately malnourished
individuals (most commonly children 6 - 59 months and Pregnant and Lactating Women, PLW) through the
provision of nutritional support,
• To prevent deterioration into Severe Acute Malnutrition (SAM)
• To reduce the risk of morbidity and mortality associated with MAM
• To provide nutrition/health education and opportunities for counselling
Where required and resources allow, other nutritionally vulnerable groups can also be targeted, e.g.
adolescents, people living with HIV/AIDS (PLWHA) or other chronic disease, older people, etc.
22 Refer also to the 2011 National Guidelines on Targeting Relief Food Assistance. Ministry of Agriculture (Disaster Risk
Management and Food Security Sector), Addis Ababa, Ethiopia.
14
2.3.2.2 When to establish TSFPs
During times of heightened food insecurity, emergency nutrition interventions such as TSFPs may be
required to complement routine MAM treatment and prevention programmes. For further information
regarding criteria for starting emergency TSFPs, please refer to the Ethiopia ENI guideline, 2011.
2.3.2.3 Determining the case load for a TSFP
For new programmes, the number of beneficiaries can be estimated based on the findings of the most
recent nutritional assessment. Examples are given below for how to calculate the expected case-loads:
Total number of malnourished group =
Total population of vulnerable group X Prevalence rate of Moderate Acute Malnutrition23
For planning purposes, it is common to estimate that between 70-80% coverage of the population will be
reached by the TSFP.
Example 1:
A standard nutrition survey conducted in Borena Zone indicated a GAM level of 14.6% and a SAM of 1.6%.
The estimated total population of the survey area was 50,000. Based on the nutrition survey results, the
estimated number of children to be enrolled in the programme is calculated as follows:
• Total population of the area = 50,000
• Under 5 population (for example, 18% of total population) = 50,000 x 18/100 = 9,000
• Prevalence of MAM = GAM- SAM = MAM level (14.6% - 1.6%)= 13%
• Number of MAM children in the area = 9,000 x 13/100 = 1,170
• 75% of MAM children expected to be reached by TSFP = 1,170 x 75/100 = 878
It can be more difficult to estimate the expected case load of pregnant and lactating women for the TSFP
because the exact percentage of the women of childbearing age in the population that is pregnant or
lactating is generally unknown (if the figure is known, then it can be used for the calculation). However, a
rough measure can be used, estimating that approximately 5% of the total population will be women of
childbearing age, who are likely to be pregnant or lactating at any one time.
Example 2:
The same standard nutrition survey in Borena Zone also measured the MUAC of all PLW included in the
survey. This indicated that 10% of PLW were moderately malnourished.
• Total population in the area = 50,000
• Estimated population of PLW in the area (5% of total population) = 50,000 x 5/100 = 2,500
• Estimated number of PLW who are MAM (10%) = 2,500 x 10/100 = 250
• 75% of PLW with MAM expected to be reached by TSFP = 250 x 75/100 = 188
For ongoing programmes (and where it is not possible to conduct a nutrition assessment), trends of
admissions can be used, to forecast expected case-loads for the next phase of the programme.
23 The incidence rate should also be accounted for as new cases will arise during programme implementation. However, as yet there
is no international consensus about what number to use as the incidence multiplier, although at global level, WFP is currently using
prevalence multiplied by 2.
15
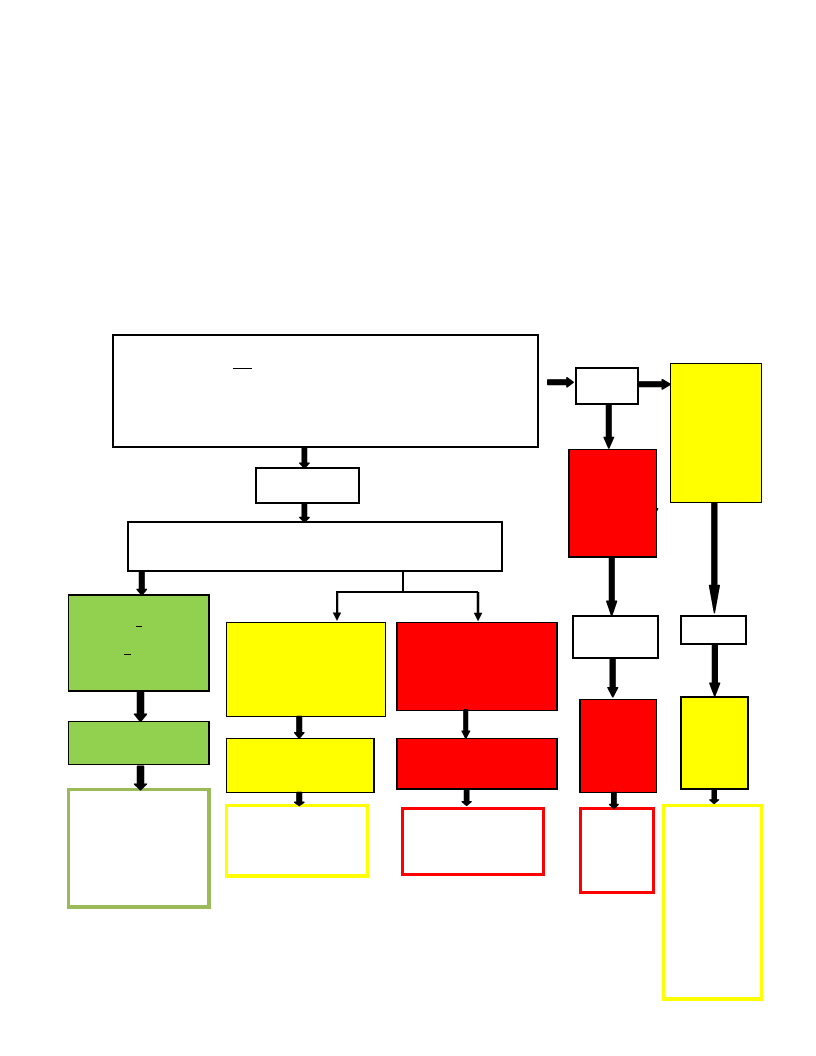
2.3.2.4 TSFP triage, diagnosis and beneficiary selection
Screening conducted at the community level is done through MUAC measurement (see community
mobilisation section 3.1). When individuals arrive at the distribution site (referred or otherwise),
programme staff (ideally in conjunction with an HEW or other suitably qualified health worker) should
assess each individual for malnutrition; this includes taking anthropometric measurements, recent history,
and a medical examination. Based on this information, the health worker can determine the appropriate
course of treatment depending on whether the individual is moderately or severely malnourished. Figure 4
below summarises the triage process for acute malnutrition:
Figure 4: Triage process for children 6 – 59 months screened or referred to distribution site or health
facility for Management of Acute Malnutrition (for infants 0 - 6 months, refer to SAM guidelines)
Step 1: Check for visible signs of malnutrition and medical complications
Does the child have any of the following? (Refer to IMCI treatment booklet
for advice and guidance on assessing the sick child)
hypoglycaemia, fever, hypothermia, vomiting, dehydration, severe
anaemia, very weak, lethargic, unconscious, convulsions, skin lesions,
difficult or fast breathing, bilateral pitting oedema +++
NO
Step 2: Check oedema and anthropometric measurements; record
on the child growth card
YES
And the child
has:
MUAC <11.0
cm
OR
WFH < -3 Z-
score
And the child
has:
MUAC ≥11.0
to < 12.0 cm
OR
WFH < -2 to
≥-3 Z-score
AND
No oedema
If the child has:
MUAC >12.0 cm
OR
WFH > -2 Z-score
AND
No oedema
CHILD IS HEALTHY
Step 3: Praise the
mother, provide
counselling on child
nutrition (including the
use of milk products,
where possible) and
send child home
If the child has:
MUAC ≥11.0 – < 12.0 cm
OR
WFH < -2 to ≥-3 Z-score
AND
No oedema
CHILD IS MAM
without complications
Step 3: Admit to
Targeted SFP following
procedures outlined
below
If the child has:
MUAC < 11.0cm OR WFH
< -3 Z-score
OR
+, ++ Bilateral oedema
CHILD IS SAM
without complications
Step 3: Refer to
Outpatient Therapeutic
Programme (OTP)
YES
YES
CHILD
IS SAM
with
compli-
cations
CHILD
IS MAM
with
compli-
cations
Fast
Track to
TFU (for
in-patient
care)
Follow IMCI
algorithm for
appropriate
treatment of
complications.
Refer to higher
level facility as
necessary.
Provide
treatment for
MAM
according to
the protocol.
16
The triage diagram in figure 4, outlines steps to identify individuals with acute malnutrition (see annex 10
for how to check for oedema and measure MUAC, weight and height/length):
Step 1:
Check for visible signs of malnutrition and any medical complications (e.g. signs of common infections). If
the individual is medically unwell or severely malnourished, they should be referred to the nearest health
facility for further assessment and appropriate treatment.
Step 2:
Check for oedema and measure anthropometry (see table 1 below); for those with acute malnutrition
(without additional medical complications) refer to the appropriate nutritional treatment centre and record
on the child growth card.
If bilateral pitting oedema is present, the individual is suffering from SAM and should be referred to the
nearest health facility (or mobile health clinic) providing OTP (+ or ++ oedema) or TFU (+++ oedema). See
annex 10 for a description of how to test for oedema.
Bilateral pitting oedema (kwashiorkor) is always considered as severe
malnutrition (SAM), due to its complex causes and high mortality risk if
left untreated (or poorly treated). Successful treatment requires the child
to receive additional medical care and therapeutic products; RUTF and
specialised milks.
Immediately refer any child identified with oedema to the nearest health
facility.
Step 3:
Take appropriate action. Use the WHO reference tables to determine z-scores and MUAC measurements.
• For healthy children (green) praise the caregiver, provide nutrition counselling including the use of
milk products, where possible and send the child home.
• For MAM children (yellow), admit to TSFP. For MAM children (yellow) with complications, follow
IMCI algorithm for appropriate treatment of complications. Refer to higher level facility as
necessary. Provide treatment for MAM according to the protocol.
• For SAM children (red) with appetite and without complications (see national protocol for SAM
management), refer to OTP. For SAM children with complications (red), refer to nearest TFU.
17
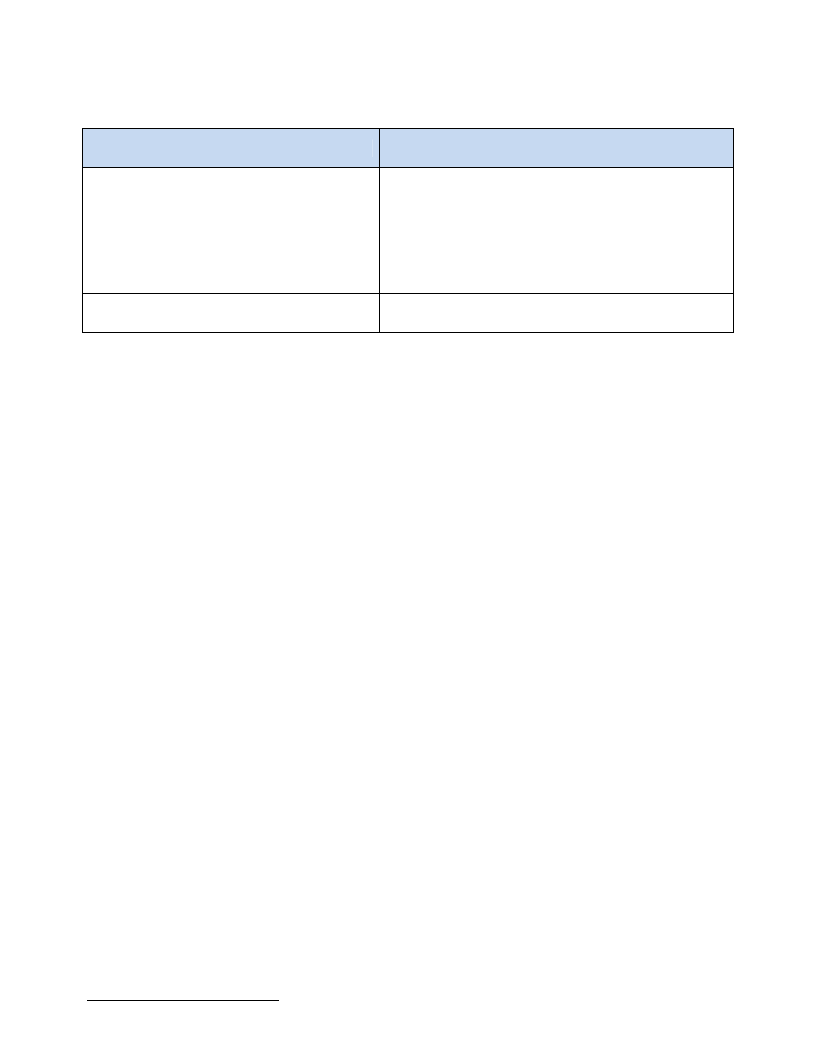

Table 1: Target group and type of measurement
Target group
Type of measurement
Children 6 to 59 months
•
(establish the age of the younger child from
discussion with the mother. 110 cm in height •
can be used as a proxy for children up to 5
years)
•
Take MUAC measurement for children 6 – 59
months using MUAC tape
Take Weight and length, if child is less than 24
months or less than 87 cm
Take height if child is 24 months and above or more
than 87 cm
Pregnant and lactating women (PLW)
Take and record MUAC measurement using MUAC tape
2.3.2.5 Admission criteria for TSFP
Admission to TSFPs for children 6-59 months rely on two types of anthropometric indicators of acute
malnutrition; MUAC and WFH z-score based on the 2006 WHO GS (as summarised in table 2 below). As the
transition to the use of WHO GS might take some time to implement, the NCHS 1977 reference tables and
table for admission/discharge criteria are provided in annex 11.
In Ethiopia, emergency TSFPs have traditionally used WFH percentage of the median, and MUAC for
admission and discharge, with the Enhanced Outreach Strategy (EOS) programme using MUAC ≥11.0 to <
12.0 cm as the sole admission criterion. Since 2009, global recommendations for admission to programmes
that treat acute malnutrition have recommended the use of WFH z-scores instead of percentage of the
median (see section 1.3 the identification of acute malnutrition for more detail).
If programmes are using a ‘two-stage’ screening and admission process, i.e. screening conducted in the
community using MUAC and subsequent admission to the programme using only WFH criteria, then it is
likely that the programme will suffer from negative feedback in the community due to the number of
‘rejected referrals’. WFH and MUAC are two different indicators, which identify two different populations;
while there is some overlap of cases that will be identified as MAM using both indicators, inevitably some
cases of MAM identified through MUAC will not subsequently be admitted to the programme on the WFH
criteria. Problems arise when caregivers have attended the site with the expectation that they will receive
food for their child (the referral slip is often viewed as a ‘promise’ of food). If their child is then not
admitted to the programme, meaning they go away empty handed, caregivers often will not return to the
site, even if their child’s condition deteriorates. Furthermore, they might discourage family, friends and
neighbours from attending the programme following referral.
2.3.2.5.1 MAM children 6-59 months
MUAC is an internationally accepted independent criterion for admission for children 6-59 months of age,
although exact age may be difficult to obtain. Where this is so, the caregiver should be asked to estimate
the age of the child (or use the family health card, where available). The mother is likely to be able to recall
the time of birth of a young child and it is essential to obtain this information. 24 Local events calendars can
help this process. Children should not only be selected on the basis of height as a proxy for age, as in
24 A guide for selective feeding programmes, UNHCR/WFP. Geneva, May 2009.
18
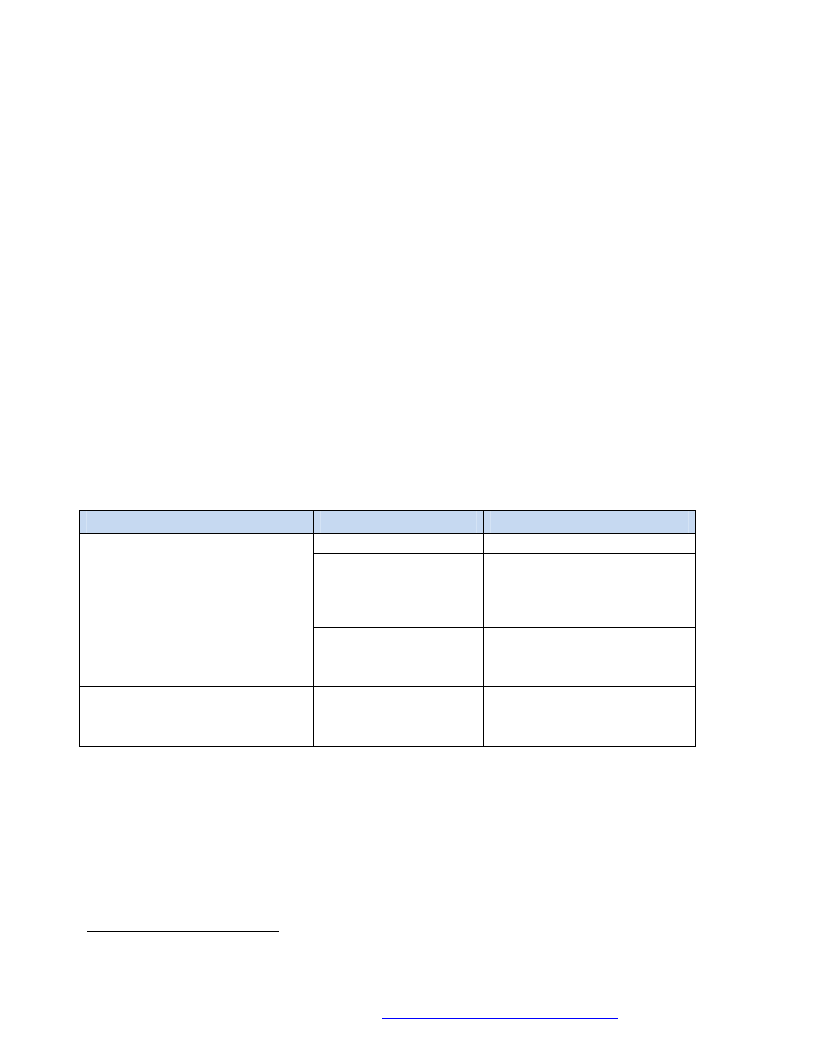

populations with high stunting rates (such as Ethiopia), there will be many children older than 6 months but
shorter than 65 cm. Such children would therefore be excluded from the programme if a proxy height was
used.
Infants under-6 months must never be included in the TSFP, but referred to the nearest TFU for treatment
when identified as malnourished [see section 4.1 for the Management of Acute Malnutrition in Infants
(MAMI)].
2.3.2.5.2 MAM Pregnant and Lactating Women (PLW)
During pregnancy and lactation, women’s nutritional needs are greatly increased, largely due to the
demands for net tissue deposit or milk formation. According to the recommendations from 2003, pregnant
women with a normal weight before pregnancy require an additional 285 kcal/day and lactating women
require an additional 500 kcal/day. 25 Both pregnant and lactating women also have increased needs for
micronutrients. Iron, folate, vitamin A and iodine are especially important for the health of women and
their infants.26
In Ethiopia, the current MUAC cut-off for classification of MAM in pregnant women in their third trimester
of pregnancy and lactating women with an infant < 6 months, is recommended to be < 23.0 cm
Table 2: Summary of Admission Criteria for TSFP
Target group
Indicator
Oedema
Children:
6-59 months
Women:
Pregnant (3rd trimester)
Lactating (infant < 6 months)
Anthropometric
Measurements
Follow-up of SAM
patients
Anthropometric
Measurement
Criteria
None
MUAC: ≥11.0 cm to < 12.0 cm
AND/OR
Weight-for-height (WFH) z-
score: < -2 to ≥ -3
Discharged cured from OTP
(automatic admission TSFP for
2 months to prevent relapse)
MUAC: < 23.0 cm
25 Well-nourished women with adequate gestational weight gain should increase their food intake by 505 kcal/day for the first 6
months of lactation, while undernourished women and those with insufficient gestational weight gain should add to their personal
energy demands 675 kcal/day during the first semester of lactation. Energy requirements for milk production in the second 6 months
are dependent on rates of milk production, which are highly variable among women and populations. Food and Nutrition Needs in
Emergencies. UNHCR/UNICEF/WFP/WHO. Geneva, 2003. http://www.unhcr.org/publ/PUBL/45fa745b2.pdf
26 A guide for selective feeding programmes, UNHCR/WFP. Geneva, May 2009.
19
2.3.2.5.3 MAM in other vulnerable groups (admission and discharge criteria)
Table 3: Recommendations for admission and discharge criteria for other vulnerable groups
suffering from MAM
(Source – adapted from the HTP MODULE 12: Management of MAM, technical notes, version 2: 2011 and
the Ethiopia HIV and Nutrition guideline, revised 2011)
Vulnerable
group
Infants < 6
months
Children 5 to
<10 years
Admission
Discharge
WFH z-score ≤ -2. Infants with MAM should immediately be referred to in-patient care
where appropriate support for breastfeeding can be given, where possible.
MUAC ≥ 13 to < 14 cm
MUAC ≥ 14.0 cm for two
consecutive distributions
Adolescents
with MAM
Weight-for-height (WFH) z-score: < -2 to ≥ -3.
MUAC for age >10 to ≤ 15 years old; ≥ 16 to < 18
cm
WFH ≥ -2 z-score for two
consecutive distributions
MUAC ≥ 18.0 cm for two
consecutive distributions
Adults with
HIV/AIDS
and/or TB and
MAM
Body Mass Index (BMI)27 –for-age, with results
presented based on
Weight-for-height (WFH) z-score: < -2 to ≥ -3
according to the WHO growth Reference for
children and adolescents (see annex 12)
MUAC ≥ 18.0 to < 23.0 cm
For non-pregnant or lactating
BMI < 18.5
OR
For PLW with HIV/AIDS and/or TB
MUAC ≥ 18.0 to < 23.0 cm
WFH ≥ -2 z-score for two
consecutive distributions
MUAC ≥ 23.0 cm for two
consecutive distributions
UNHCR/WFP recommend
discharge for adults as
BMI ≥ 18.5
2.3.2.6 TSFP distribution procedures at the site for new and registered
beneficiaries
Once the decision has been made to admit a beneficiary to the TSFP, the following steps should be
completed as follows;
1. Beneficiary registration
2. Administration of routine treatment
3. Follow-up procedures for those already registered in TSFP and referrals to OTP/TFU
4. Nutritional counselling and education
5. Distribution of the supplementary food ration
6. Discharge criteria and procedures
27 Body Mass Index defined as the (weight in Kg)/(height in m)² for assessing the nutritional status of adults
20
2.3.2.6.1 Beneficiary registration
a) Provide the beneficiary or caregiver with a ration card (see annex 2)
b) Ensure that the registration book is filled in with all essential information, e.g. name, age, sex,
home address, anthropometric details on admission, etc. (see annex 4 for example of registration
book)
c) Explain the process of the TSFP to the beneficiary or caregiver, including how the programme
works, reasons for admission to the programme, the ration given and expected length of stay.
Posters at the site (in local language and/or descriptions through pictures) can help the
beneficiaries understand what to expect at the site, and what they are entitled to
2.3.2.6.2 Routine treatment
The TSFP should always provide routine medicines, such as, antihelminthics, vitamin A supplementation
and routine immunizations. The tables below (4 and 5) detail each medicine, with specifications of when to
give and the dose. Pregnant women must be referred to the nearest health facility for Ante-Natal Care
(ANC) to receive additional services, such as iron/folate supplementation and tetanus vaccination.
Table 4: Summary of routine medicines for children 6-59 months
Name of Medicine
Vitamin A28
When
On admission
Antihelminithic
Albendazole
On admission
OR
Mebendazole
Measles vaccination
On admission
On admission
Age
Dose
6 to 11 months 100,000 IU
≥ 12 months
< 12 months
12 to 23 months
≥ 24 months
< 12 months
12 to 23 months
≥ 24 months
9 months or older
200,000 IU
Do not give
200mg
400mg
Do not give
500 mg
500 mg
Prescription
Single dose on
admission
None
Single dose on
admission
None
Single dose on
admission
One dose
Table 5: Summary of routine medicines for pregnant and lactating women
Name of Product When
Albendazole or
Mebendazole
Vitamin A
Third trimester
Within first 6
weeks after
delivery
Physiological
Status
Pregnancy
Post-partum
Dose
Albendazole 400mg OR
Mebendazole 500 mg
200,000 IU
Prescription
Single dose
Single dose
on admission
2.3.2.6.3 Follow up procedures for those already registered in TSFP
The beneficiary’s progress should be monitored at every visit; assess for oedema, weight and MUAC every 2
weeks and height every month (where a height board is available). Record the measurements in the
register and, importantly, analyse whether there has been any improvement or deterioration. If any
28 Do not give vitamin A supplement (VAS) if child has received within the last one month. It is vital to check with local health
officials whether there have been any VAS campaigns in the area during the previous month.
21

deterioration is noted, alert the TSF supervisor and refer to the nearest health facility for further follow up.
Each beneficiary should receive nutrition counselling and education sessions (including the importance of
using milk-based products for children < 2 years) prior to receipt of the next ration.
During each follow up at the TSFP site, the following actions are encouraged:
• If the child is gaining weight, congratulate the caregiver and explain that the child is improving
• If the child has lost weight since the last visit, or has not gained weight in 3 consecutive
distributions, conduct a thorough medical examination to ensure there are no concurrent medical
problems. Explain the situation to the caregiver with a reminder of the importance of not sharing
the food rations; reinforce nutritious food preparation with the caregiver
• If the child or PLW fails to reach the target weight within four months, or loses weight on 3
consecutive distributions, refer him/her to the outpatient department for a medical check-up (see
section 2.3.2.9.2 for discharge criteria)
2.3.2.6.4 Transfer to OTP or inpatient unit (TFU or SC)
Even while registered in the TSFP, MAM children can be at risk of becoming severely malnourished if they
suffer from an episode of illness or other problem. Their health and growth must be monitored at each SFP
visit to ensure that they are improving as expected and also to identify those whose condition has
deteriorated.
Children should be referred to the nearest OTP for further assessment if any of the following occurs (see
annex 13 for example of referral form):
Bilateral pitting oedema develops
MUAC drops below 11.0 cm
WFH z-score decreases to less than -3
Development of any medical complications
The health worker at the OTP can then determine if the child should be admitted to OTP or referred to the
nearest TFU (using the triage diagram outlined in figure 3, page 16).
2.3.2.7 Nutrition counselling and education
A vital part of MAM programming; for further information refer to chapter 4.
2.3.2.8 Supplementary food ration
2.3.2.8.1 Provision of the dry ration
The regular distribution of fortified blended food (FBF) or other nutritional rehabilitation products (e.g.
RUF) to assist in home treatment is given. FBF is a pre-mixed, fortified food which contains the necessary
nutrients to treat MAM. It is strongly advised to provide dry rations to beneficiaries rather than implement
‘wet feeding’ programmes for the following reasons:
Advantages of the dry ration
• Less risk of cross-infection as large numbers of malnourished and sick children do not have to sit in
close proximity while feeding
22

• Fewer resources and organisation than wet feeding; staff time taken to establish and implement
the programme. Programmes can therefore be established in a more timely fashion
• Less opportunity costs for caregivers who only have to attend once every two weeks, which
generally leads to better coverage of the population and a lower default rate
• Encourages the responsibility for rehabilitation of malnourished individuals within the family
• Improved access which is more appropriate for widely dispersed populations (as in much of
Ethiopia), many of whom would have to travel long distances to attend daily
Quantity and quality of the ration
The dry ration supplement should consist of approximately 1124 kcal per day.
This can be achieved by the provision of 6.25 kg FBF and 1 litre of oil29 per beneficiary/per month.
The food provided should have the following characteristics using NutVal 2006 version:
37.4 % of the energy as protein
45.5 % of the energy as fat
An adequate nutrient content (concentration) for all the essential micronutrients according to
Recommended Dietary Allowances (RDAs)
The shelf-life of the supplementary food should be known; the product adequately labelled and must be
free from infestation and spoilage. Supplementary food must be correctly stored (see section 2.2.3 for
more detail).
2.3.2.8.2 Premixing the ration
When oil and sugar are given alongside the FBF, it is essential to mix it into the FBF before distribution. This
is to ensure that the oil and sugar are not used for the family cooking or sold, as they can otherwise be
viewed as valuable cash opportunities for the caregivers. If rations are premixed at the distribution site, the
beneficiaries will be more likely to reap the full benefit of the ration, resulting in TSFPs being more able to
reach the objectives of successful treatment of MAM in the community.
However, premix must be used within a 2 week period before any rancidity develops; if the distributions
are being conducted less frequently e.g. monthly, then FBF and oil should not be premixed at the site.
2.3.2.8.3 Cooking demonstrations
Fortified Blended Food (FBF) can be ‘spoiled’ if it the porridge is cooked either for too little, or too much
time. The ideal cooking time to maximise the nutrients available in FBF is 10 minutes. In order that the
beneficiaries well understand how best to cook the ration, cooking demonstrations conducted on-site can
be very helpful. If at all possible, caregivers should be asked to assist with the cooking, as the learning will
likely be more effective if they are included in the practical aspects of cooking. It is also important to
indicate how much and how often the porridge should be given to the children. The correct measurements
for cooking either thick or thin porridge are included as annex 14.
Sometimes beneficiaries prefer to cook bread with the flour. This should be strongly discouraged, as bread
more often tends to be shared around the family, meaning the malnourished individual will not be
receiving the correct amount of calories/nutrients for recovery.
29 One litre of oil weighs 0.9 kg
23
Where possible and resources allow, demonstrations should also be conducted to show how to prepare
nutrient-rich meals which are appropriate for infants and young children using locally available foods. This
can help to reinforce the nutrition and health education messaging on how to prevent healthy children
deteriorating into sick children.
2.3.2.8.4 Newer products for the treatment of MAM
A host of new products are now available for the treatment of MAM. However, as yet no conclusive
evidence is available to identify which product is superior to the others in any given situation. A decision
tree has been developed to assist with the selection of nutritional products for particular MAM
interventions and is included as annex 15.
It is however important to note that no definitive evidence is yet available for which of these products
might be most appropriate and in which context. Organisations need to weigh up the advantages and
disadvantages of each product (including cost of treatment) before deciding what is best to use. Any
products used in Ethiopia must be registered and approved for use by the Food, Medicine and Health Care
Administration and Control Authority (FMHACA). It is also vital that agencies discuss and secure agreement
with local, regional and federal MoH staff, prior to implementing programmes using any of these ‘new’
products. It is also very important that organisations ensure they have sufficient stocks of the product for
the entire programme. Beneficiaries might become confused and/or discouraged if they are receiving
different products at different times.
2.3.2.9 Discharge criteria
2.3.2.9.1 Discharge recovered cured
There is currently no internationally recognised consensus on the discharge criteria for TSFP using the
recommended admission criterion, MUAC.30 It is therefore recommended that a target weight gain of 13%
increase in weight from admission weight is used for MUAC admissions (see annex 16 for 13% target weight
gain table and annex 17 for discussion of the 13% target weight gain criterion). For admissions on WFH z-
scores, discharge is recommended as ≥ -2 scores for two consecutive distributions. Table 6 below
elaborates the discharge criteria for recovery of children 6-59 months and PLW suffering from MAM:
Table 6: Criteria for MAM beneficiaries, discharge ‘recovered/cured’
Admission criteria:
Children with MUAC ≥11.0 to < 12.0 cm
Children with WFH < -2 to ≥-3 z-score without
complications
Pregnant and lactating women with a MUAC
< 23.0 cm
Corresponding discharge criteria:
Reach the target weight gain of 13% from admission
weight AND
MUAC ≥ 12.0 cm for two consecutive distributions
≥ -2 z-score for a period of two consecutive
distributions
MUAC > 23.0 cm for two consecutive distributions
30 The EOS programme does not need to use a discharge criteria; as the screening is done every 6 months (child health days screen
every 3 months), the child has a MUAC < 12.0 cm so is admitted/remains in the programme, or the MUAC is ≥ 12.0 cm and is not
registered for the next distribution.
24

The discharge criteria must match the admission criteria. For example, children admitted on WFH z-scores
should be discharged using WFH Z-score ≥ -2 for 2 consecutive distributions.
If a child was admitted based on MUAC, they should be discharged based on a target weight gain of 13%
AND MUAC ≥ 12.0 cm for 2 consecutive distributions. If the child reaches 13% target weight gain, but the
MUAC measurement remains less than 12.0 cm, the child should continue attending TSFP distributions until
the MUAC reaches ≥ 12.0 cm.
2.3.2.9.2 Discharges from TSFP other than recovered cured - children 6-59 months
Programme discharges in categories other than those who ‘recover’ are described below:
• Died: Child died after admission to the programme (this should be confirmed by a home visit or by
information provided by neighbours/relatives)
• Defaulter: Child is absent from the programme for three consecutive distributions
• Transfer: Either the child’s condition deteriorated requiring transfer to the TFP (OTP or TFU) or the
family moved and the child was transferred to another SFP site (transfers are not included in
calculations of programme performance). Numbers of transfers to in-patient care should be closely
monitored, as high numbers could indicate a worsening food security situation in the area
• Non-response (failure to respond to treatment): Where a child fails to reach the discharge criteria
over a period of four months, they should be discharged as a non-responder. Investigations must
be conducted prior to discharge, as outlined below
Criteria for investigating failure to respond to treatment:
1. No weight gain after 6 weeks in the programme
2. Weight loss during 4 consecutive weeks in the programme
3. Weight loss exceeding 5% of body weight at any time
4. Failure to reach discharge criteria after 4 months in the programme
Possible reasons for failure to respond:
1. Problems with the application of the protocol
2. An underlying physical condition/illness, such as HIV/AIDS, TB
3. Nutritional deficiencies that are not being corrected by the diet supplied in the TSFP
4. Home/social circumstances of the individual
5. Excessive sharing of the ration
6. Other causes
Steps to take for failure to respond to treatment:
Step 1: Review the patient’s register card and confirm that the protocol for TSFP has been adhered to
correctly (ensure that the details on the child’s card are correct)
Step 2: Conduct a full medical examination and nutrition assessment. If the patient presents with any signs
of medical complications or nutrition deficiencies, refer immediately to the nearest health facility or TFU
for further investigation and/or treatment
25

Step 3: Request a home visit by community mobilisers to assess the home/social situation of the child.
Assess whether the caregiver is preparing the porridge correctly, whether it is acceptable/tolerated by the
child and whether the supplementary food is being given exclusively to the child or excessive sharing is
occurring (see annex 18 for home visit form)
2.3.2.9.3 Discharges from TSFP other than recovered cured - PLW
Programme discharges in categories other than those who ‘recover’ are described below:
• Died: PLW died after admission to the programme (this should be confirmed by a home visit or by
information provided by neighbours/relatives)
• Defaulter: PLW is absent from the programme for three consecutive distributions
• Transfer: If the family has moved and the PLW was transferred to another SFP site (transfers are
not included in calculations of programme performance)
• Other discharges/non-response
o For pregnant women - child is born. The woman should be encouraged to return to the TSFP
once the confinement period is over (usually 40 days), to check whether she is still MAM and
is entitled to receive TSF rations
o For lactating women - Infant reaches 6 months of age. Infant’s anthropometric status should
then be checked, if the infant is MAM, it should be admitted to the TSFP
2.3.2.10 When to close the emergency TSFP
Repeat anthropometric nutrition surveys should be conducted to inform programme effectiveness and
assess whether the programme should continue or phase-out. Refer to the Ethiopia ENI, 2011 for more
details.
26

Chapter 3. Monitoring, reporting and coverage
3.1 Monitoring
It is important to know whether the intervention is making progress towards its objectives. Monitoring
helps implementers to understand what is working well and what is sub-optimal, and where gaps may be.
If management and information systems are simple the burden on programme staff will be produced, but
sufficient and useful information to ensure programme effectiveness can be provided. Robust and regular
monitoring information can also facilitate programme managers in decision making and whether any
adjustments are required.
For effective TSF programming three kinds of monitoring are required: 31
a) individual beneficiaries
Four tools are available:
i) Individual ration/record cards
ii) Registration books
iii) Referral slips
iv) Records of home visit/post distribution monitoring forms
Beneficiaries are anthropometrically monitored at each visit with details recorded in the registration book
and on their ration cards. Numbering systems should be developed to enable tracking of individual
beneficiaries, especially for those transferring between SFP and OTP.
Home visits using post-distribution monitoring questionnaires (see annex 19) should be conducted when
indicated and wherever possible.
b) Programme performance and effectiveness
Several tools are available for use:
Monthly reports with data on admissions and discharges (statistical data) are compiled for TSFP.
See below, reporting.
Supervision checklists and/or reports - supportive supervision of TSFP sites should be conducted
regularly by programme managers and federal/regional MoH counterparts (see annex 7). Joint
supervision between partners is more likely to result in successful outcomes
Collection of additional information – readmissions, cause of death, reasons for default and non-
recovery. Collected by community outreach workers, mobilisers or other programme staff
Mapping – simple mapping can also be done. This will help identify where most of the admissions
are coming from and can help determine if more sites should be opened. This can also help
programme implementers better understand possible issues in the programme such as high default
or low coverage
Focus group discussions (FGD) with community members - discussions with affected communities
by the MoH and programme staff can also provide useful insights into programme perceptions, and
identify any barriers to uptake. FGDs are useful tools to initiate and direct discussion around how
programmes can improve the delivery of services (see annex 20).
Coverage monitoring surveys (see below)
31 Following the individual beneficiary is only possible in TSFPs, not BSFPs.
27

c) Commodity distribution monitoring and reporting
Stock reports are required to provide a breakdown of stock movement and to facilitate uninterrupted
supplies (see annex 9). It is recommended that programmes keep a buffer stock of supplies and pre-
position food during expected rainy seasons when transport of commodities are likely to become more
challenging. The provision of clear instructions regarding minimum re-order levels of commodities can
assist with ensuring an uninterrupted supply chain.
3.2 Reporting
3.2.1 Completing the monthly report
• Programme data can be compiled at each distribution site (usually 2-weekly) on tally sheets. The
compilation sheets can be used for combining information from various sites and also for collating
2 weekly information into monthly data (see annex 5 for example of tally and compilation sheets)
• Programme data must be extrapolated according to admission group e.g. 6-59 months, PLW, other
vulnerable groups
• Data should be disaggregated by gender e.g. no of boys/girls recovered cured, died, etc.
• Programme data should then be compiled every month from the tally and compilation sheets and
collated into one monthly report per woreda (see annex 6 for example of monthly report)
• To facilitate calculations and speed up data processing, the monthly reports may be collated into a
simple excel spreadsheet or access database, to facilitate programme implementers in monitoring
progress and performance
• Reports must be filled in accurately. Cases should not be double counted. Particular attention
should be given to accurately recording returning defaulters and/or readmissions. In areas where
there is considerable movement of the population (e.g. pastoralist livelihood zones), care should be
given to track ‘moved’ cases, where possible
3.2.2 Using the monthly reports to determine programme performance
• Programme outcomes (numbers of beneficiaries who have recovered, died, defaulted and non-
recovered) can be compared to international minimum standards in order to provide information
on how well the programme is performing. Outcomes can be illustrated in graph form
• Following analysis at facility level with health staff, the reports should be passed to the woreda
health information system and then to zonal, regional and federal level
28
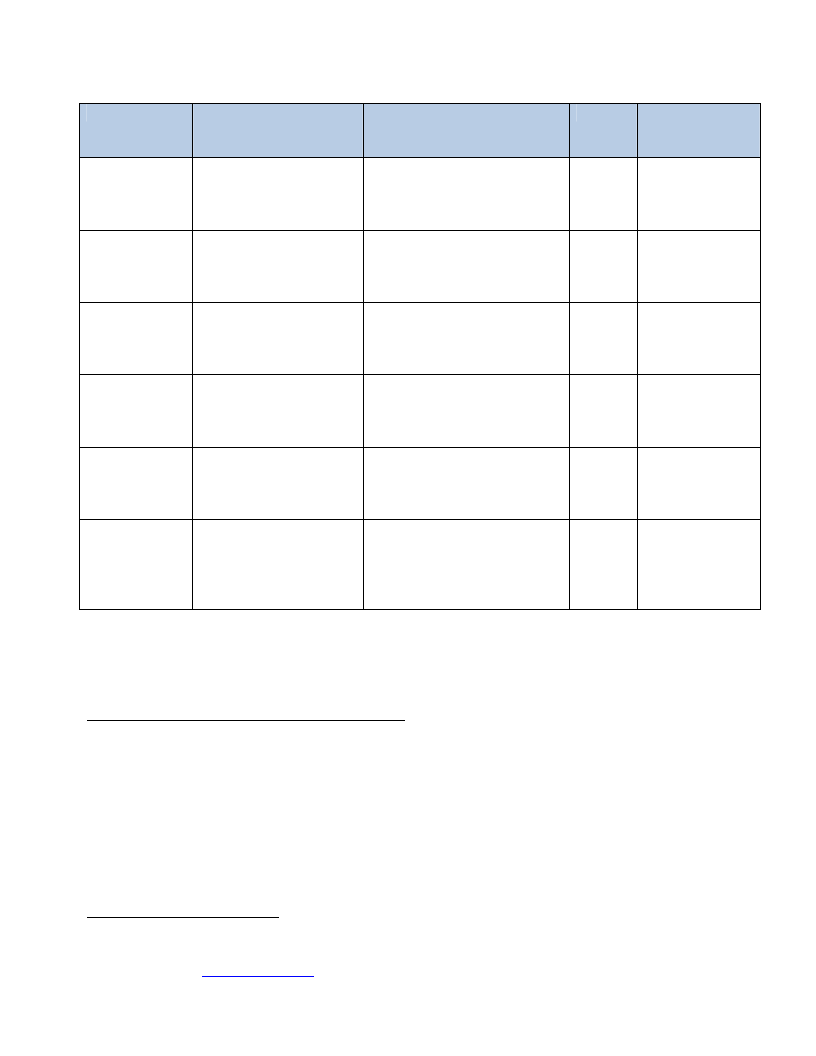
Table 7: Calculation of indicators for the monthly report (example given is for Under-5 children)
Indicator32
Recovery rate
Death rate
Default rate
Non-responder
rate
Mean length of
stay (see annex
6 for how to
calculate)
Average weight
gain (see annex
6 for how to
calculate)
Description
Proportion of U5
discharges due to
recovery
Proportion of U5
discharges due to death
Proportion of U5
discharges due to default
Proportion of U5
discharges due to non-
response
Average length of stay for
recovered children
Average number of grams
that 6-59 m recovered
children gained per kg per
day since admission to
TSFP
Formula
No. 6-59 m recovered/total no.
of 6-59 m discharges
(recovered, died, default and
non-response) X 100
No. 6-59 m died/total no. of 6-
59 m discharges (recovered,
died, default and non-response)
X 100
No. 6-59 m defaulted/total no.
of 6-59 m discharges
(recovered, died, default and
non-response) X 100
No. 6-59 m non-response/total
no. of 6-59 m discharges
(recovered, died, default and
non-response) X 100
Sum no. of weeks admissions of
recovered children 6-59 m/No.
6-59 m discharges due to
recovery
Sum [(weight on discharge (g) –
weight on admission
(g))/(weight on admission (kg))
X duration of treatment (days)]
Unit
%
%
%
%
weeks
g/kg/day
Sphere
recommendation
for TSFP33
>75%
<3%
<15%
No
recommendation
Depends on
country context
Depends on
country context
3.3 Coverage
Estimating coverage of selective feeding programmes
Coverage is an extremely valuable indicator to monitor the quality and impact of selective feeding
programmes.34 Assessments of programme coverage are vital, as while the TSFP services might be in place,
it does not necessarily follow that the population are fully utilising these services. It is important to
measure and quantify levels of service uptake by the target population, to understand the reasons why
some areas may have high uptake and others low, as lessons can be learned from both scenarios.
Previous methods to assess coverage were based on two stage cluster sampling methodology using
population proportional sampling (PPS) which were only able to produce fairly unreliable estimates of
coverage.
32 Transfers in/out of the programme are not included in the calculation of programme performance
33 The Sphere Project. Humanitarian Charter and Minimum Standards in Disaster Response. Geneva. 2011 Edition. Sphere Project.
Hobbs Publishing, UK. www.sphereproject.org
34 Coverage refers to the degree of exclusion error- i.e. the omission of eligible children (e.g. with WFH <-2 to ≥-3 z-score and/or
MUAC ≥11.0 and < 12.0 cm) into the programme. ‘Acceptable’ standard for coverage refers to the Sphere Project Guidelines (2011)
recommending >50% coverage as acceptable for selective feeding programmes in rural communities, >70% in urban populations and
>90% in a camp situation.
29

Methods of measuring coverage:
1. Centric Systematic Area Sampling (CSAS)
In 2003, a new methodology for the measurement of coverage was developed that has been widely
used in Ethiopia; the Centric Systematic Area Sampling (CSAS) survey.35 These surveys are based on
small eligible populations assuming simple random samples. CSAS is based on spatial geographic
sampling, using many clusters randomly selected from quadrats allocated to a map of the study area.
Survey teams are assigned to use active case finding techniques to identify all cases in the sampled
community and calculate the number of cases that are currently enrolled in the programme. CSAS
surveys provide two estimates of coverage; period and point, described below in Figure 5:
Figure 5: Formulas for calculating period and point coverage
Formula 1: Period coverage
Children enrolled in the programme, malnourished or not malnourished
Children enrolled in the programme, malnourished or not malnourished + children
malnourished but not enrolled
X 100
Formula 2: Point coverage
Malnourished children admitted in the programme
Total malnourished children
X 100
Period coverage estimates show the proportion of respondents in the programme, whilst point
coverage gives the ratio of cases in the programme as compared to the total number of cases
identified by the assessment.
Period coverage is designed to take into account the number of children treated by the programme
over its recent duration, including those who are no longer cases, i.e. children from 6-59 months who
were admitted as MAM cases but are currently recovering and no longer MAM on the day of the
assessment. Period coverage can therefore provide a good reflection of programme performance over
recent months.
Point coverage shows the ratio of MAM cases in the programme compared to the total number of
MAM cases identified by the assessment. Point coverage does not include children registered in the
programme who are partially recovered and no longer MAM (e.g. MUAC ≥ 12.0 cm on the day of
assessment). Point coverage estimates, with the stricter definitions, provide a reflection of
programme performance ‘right now’.
Estimates of period coverage will therefore always be higher than point coverage. While both are
useful measures, period coverage estimates are more commonly quoted, as they can provide a
broader picture of programme coverage, especially over its recent duration.
In addition to the quantitative information presented above, CSAS will also enable a wealth of
qualitative information to be collected to better understand the barriers to service uptake, or
35 New Method for Estimating Programme Coverage. Mark Myatt presentation at an interagency workshop on Community-based
Approaches to Managing Severe Malnutrition. Dublin 8-10th October 2003. http://fex.ennonline.net/21/coverage.aspx
30

misperceptions of the various selective feeding programmes that may co-exist in a community for
example. This information, if acted on, can help programme implementers to strengthen programme
performance and impact. It is therefore strongly recommended that agencies implementing selective
feeding programmes conduct a coverage survey using CSAS (or other methodology as it becomes
available) in order to effectively monitor their programmes. Annex 21 provides a simple picture guide
for conducting CSAS surveys.
At present, the current CSAS methodology is suitable only for measuring small intervention areas (i.e.
individual woredas); however new methodology for assessing wider area coverage surveys [Simple
Spatial Survey Method, (S3M)] is under development, with a plan to pilot it in Ethiopia during 2011.
2. Semi Quantitative Evaluation and Assessment of Coverage (SQUEAC)
The use of standardised and validated tools such as Semi-Quantitative Evaluation of Access and
Coverage (SQUEAC) surveys is encouraged, where resources are available. SQUEAC surveys also report
point and period coverage. These surveys are particularly useful for exploring the causes of high and
low coverage that are identified. SQUEAC surveys are usually used for measuring coverage of SAM
programmes, although it would be possible to adapt them for assessment of MAM coverage.36
3. Simple Spatial Survey Method (S3M)
The Simple Spatial Survey Method (S3M)37 is currently under development and will be piloted during
2011 in partnership with EHNRI. It has the potential to offer a platform that can accept a wide range of
indicators, is most appropriate for large area-based sampling, and produces great efficiency over
previous area-based methods (a 5-fold increase in precision over CSAS).
The potential application of this method in conducting surveys for major national level nutrition
interventions should be explored.
36 A system for providing support with coverage related queries is currently under development. It will likely be hosted on the en-net
discussion forum at http://www.en-net.org.uk/
37 To date, there is no published literature available for S3M
31

Chapter 4. Community mobilisation, nutrition counselling
and education
4.1 Community mobilisation
The term ‘community mobilisation’ refers to a range of activities designed to help implementers
understand affected communities, build a relationship with them and foster participation in the
programme.38 The high levels of MAM seen in many areas of Ethiopia ensures that it is essential that
individuals seek treatment for malnutrition as soon after onset as possible. It is also imperative that
communities understand the principles underlying malnutrition and services provided to treat it, in order to
be able to access care appropriately, obtain the maximum benefits and prevent future episodes of
malnutrition. Early and comprehensive case-finding is a key component of MAM prevention and treatment,
through a well-informed and responsive community.
A strong community volunteer network can have a considerable impact on MAM programming by
supporting and sustaining services and feeding into longer-term strategies, such as those outlined under
the National Nutrition Programme (NNP). The Health Service Extension Programme, a community based
health care delivery system that provides essential health interventions at village/kebele and household
level is the ideal vehicle for effective mobilisation; its health extension workers (HEWs) providing the bridge
between health services and the community in the facilitation of case finding, follow up and sustaining
community-based programmes to prevent and treat malnutrition.
Due to the wide variety of individuals and organisations that undertake nutrition and/or health mobilisation
activities in Ethiopia, the general term ‘community mobiliser’ is used throughout this document. Mobilisers
may be the HEWs, Community Health Volunteers, members of the Health Development Army, other
members of the community, etc.
4.1.1 Objectives of community mobilisation
The purpose of community mobilisation is to:
• Promote understanding of available services and the target groups
• Increase programme coverage
• Conduct active case finding and make appropriate referrals
• Follow-up absentees and defaulters and understand the reasons for it so that programme
implementers can address them
• Increase understanding of any barriers to access (why people might not be accessing services)
• Link prevention and treatment services at community level wherever possible, in order to address
the underlying causes of malnutrition
38 Community-Based Therapeutic Care (CTC); A Field Manual. Valid International. First Edition, 2006.
32

4.1.2 Information required prior to programming
It is important for programme implementers to gain a good understanding of community structures and
perceptions, through engaging in dialogue with key community members to determine the following
information:
• What the problems with malnutrition in the area are, what the local terms for malnutrition are, the
perceived causes and common solutions
• What the formal (e.g. village meetings) and informal (e.g. discussions at water points) channels of
communication are in the area, especially to identify those that are known to be most effective for
disseminating information
• The local schedules of events that the programme can work with and around, for example, market
days
• Local attitudes and beliefs towards health and health seeking behaviours
• Any existing interventions in the area that the programme can link with, including health, nutrition,
agriculture, water, etc. It is useful to determine interventions that already use community
volunteers to prevent duplication. Standardisation of any messages to be given to community
members is also vital, to minimise possible confusion
4.1.3 Who should be involved in community mobilisation
Community screening and mobilisation is an ongoing process and is best conducted by a range of key
figures, both to help in gaining the population’s acceptance and trust and also for communicating and
disseminating messages. In discussion with the HEWs, potentially important individuals might include;
social or political leaders (traditional and modern), religious leaders (priests, imams), traditional health
practitioners (healers, birth attendants), teachers and elders. Members of key community organisations can
also be a useful resource, for example, women’s associations, funeral associations (idirs), youth
associations, etc. Once programmes have been operational for a while, caregivers of children who have
already recovered from an episode of malnutrition can act as powerful motivators to encourage other
caregivers to seek treatment for their child (sometimes referred to as ‘positive deviants’).
4.1.4 Supplies and training
Mobilisers will need the following supplies (where resources allow) to conduct screening and follow-up
activities
• MUAC tapes
• Referral slips (see annex 3)
• Home visit forms (see annex 18)
• Post distribution monitoring forms (see annex 19)
Community mobilisers should be trained to identify, refer and follow-up malnourished individuals. Training
is usually conducted during one or two days, depending on available time, resources and levels of
understanding. Refresher training sessions should also be regularly conducted, especially if there is high
turnover of mobilisers. Training sessions should include:
33

• Programme aims, objectives and the target population
• Basic information on the causes, identification and treatment of malnutrition
• Practical sessions in identification of oedema (for referral to SAM treatment programmes) and
wasting, using the MUAC tape
• Case finding and referral
• Follow-up and home visits
• Health and nutrition education topics based on the Essential Nutrition Action (ENA) framework
• Appropriate counselling techniques
Regular meetings can also help to identify and discuss any challenges that mobilisers might be facing, and
to devise appropriate solutions.
4.1.5 Case finding and referral
In order to reach as many malnourished individuals as possible, community mobilisers must actively
identify children who require treatment. Screening can be conducted via a number of opportunities,
including:
• House to house visits
• At health facilities, community and outreach programmes (e.g. EPI, CHDs)
• At community or religious meetings, health campaigns (e.g. polio eradication campaigns) or other
opportunities
• At growth monitoring sessions (e.g. during the CBN programme), general food distributions, PSNP
gatherings, etc.
Individuals are identified with MAM in the community through the use of MUAC tapes (see section
2.3.2.5.3 for MUAC cut offs for vulnerable groups) and should be referred to the nearest distribution site
for treatment. Individuals identified as suffering from SAM [presence of bilateral pitting oedema or (for
children 6-59 months) MUAC < 11.0 cm] should be immediately referred to the nearest health facility
offering TFP services.
If programmes are using a ‘two stage’ screening and admission process, i.e. screening in the community
using MUAC and admission using WFH, as outlined in section 2.3.2.5; mobilisers should be aware that there
might be some negative feedback in the community from those they have referred, but who were
subsequently not admitted at the site.
4.1.6 Follow-up and home visits
Community mobilisers have an important role in the tracing of beneficiaries who have been absent or have
defaulted from the programme; identifying the cause of absence or default and encouraging them to
return, where possible. Individuals who are failing to gain sufficient weight also require home visits, to
establish and correct the causes of static or loss of weight.
34

4.2 Nutrition counselling and education
During emergency situations it is vitally important that IYCF practices are strengthened, wherever possible.
International guiding principles on IYCF in Emergencies is included as annex 22.
Ideal opportunities exist when addressing MAM (either during routine activities or emergency situations),
to provide nutrition and health education to beneficiaries and the wider community; at screening sites,
during home visits and SFP sites. While it must be noted that messages given at sites in ‘campaign style’ are
much less likely to be effective than those given on a one-to-one basis, education sessions given at the SFP
sites can be reinforced later by home visits or through other sessions given by HEWs or other key
community members. Community mobilisers should be encouraged to pass key health and nutrition
messages each time they come into contact with community members.
It is vitally important to ensure that any health or nutrition education
information sessions are given in the local language that the
community can understand. If the health and or distribution staff do
not speak the local language, then a person must be trained who can
speak the language in nutrition education techniques. Where this is
not possible, a translator can be used.
Simple and contextually specific flip charts written in the local
language can also help to relay important information
Areas to be addressed during nutrition education and behavioural change sessions should place particular
emphasis on the promotion of breastfeeding, discouragement of early weaning, improved feeding practices
and other measures to prevent malnutrition. The key to effective education messaging is to keep the
messages simple. In this way, caregivers and the wider community can easily understand and absorb the
most important information. The Essential Nutrition Action (ENA) framework provides an excellent base to
model education sessions on. The ENA list of seven nutrition actions is based on a lifecycle approach, as
follows:39
1. Promotion of optimal nutrition for women
2. Promotion of adequate intake of iron and folic acid and prevention and control of anaemia for
women and children
3. Promotion of adequate intake of iodine by all members of the household
4. Promotion of optimal breastfeeding during the first six months
5. Promotion of optimal complementary feeding starting at six months with continued breastfeeding
to 2 years of age and beyond
6. Promotion of optimal nutritional care of sick and severely malnourished children
7. Prevention of vitamin A deficiency in women and children
The ENA booklet that nutrition messages must be modelled on has been translated into Amharic, Tigrinya
and Oromifya and widely disseminated within the MoH system. It should therefore be available in most
health facilities. ENA information has also been included in many other materials developed by the MoH,
for example, information for the CBN programme, the Integrated Refresher Training (IRT) package, etc.
39 Guyon, AB and Quinn, VJ. Booklet on Key Essential Nutrition Actions Messages. Core Group, Washington, D.C., January 2011
35
The web link for full ENA information is:
http://www.coregroup.org/storage/Nutrition/ENA/Booklet_of_Key_ENA_Messages_complete_for_web.pdf
Nutrition surveys can provide information regarding what topics might be the most urgent to address (e.g.
low rates of breastfeeding or sub-optimal complementary feeding practices). However, four key messages
should always be provided at the TSF site or during home visits:
1. Handwashing with soap (or ash if soap is unavailable) before eating and after defecation
2. Exclusive breastfeeding (for the first 6 months)
3. Timely introduction and use of appropriate complementary foods using locally available foods
4. Continued feeding during illness
4.2.1 Promotion of good hygiene at health facilities and distribution
sites
The linkages between malnutrition and unsafe water sources/poor hygiene practices are by now extremely
well understood. It is difficult for distribution staff and/or health workers to demonstrate good hygiene and
sanitation practices (e.g. hand washing techniques) if there is an inadequate water supply at the site or
health facility. Where the health facilities lack appropriate water supply, short term measures need to be
implemented; for example sufficient jerry cans of water and supplies of soap need to be brought to the site
to provide a practical illustration for the caregivers the importance about of hand washing prior to food
preparation. It can often be useful to provide enhanced training to at least one of the distribution staff in
hygiene practices, so they can share this knowledge with other members of the team and provide on-site
training in the case of high staff turnover.
UNICEF standards generally suggest that between 3 - 7 hand-washing stations are required per health post,
with one allocated for drinking and the rest for hand washing. If health posts lack sufficient hand washing
stations, they should immediately inform UNICEF via the Zonal and Regional MoH authorities, as it may well
be possible to supply more hand-washing stations to make up the shortfall.
36

Chapter 5. Management of acute malnutrition in infants
under-6 months (MAMI), maternal health, urban and
pastoralist issues
5.1 Management of acute malnutrition in infants < 6 months
(MAMI)
Treatment for acute malnutrition in infants has been largely neglected during emergency programming and
measurement of their nutritional status is almost never included in nutrition surveys or rapid assessments.
Focus is placed instead on children 6-59 months and malnourished pregnant and lactating women, with the
burden of malnutrition in infants remaining largely hidden.
During 2009, the Management of Acute Malnutrition in Infants (MAMI) project40 undertook an important
retrospective meta-review. The review utilised data from DHS national datasets of 21 nutritionally
vulnerable countries, drawn from the 2008 Lancet ‘Maternal and Child Undernutrition’ series of countries
(those that account for >90% of global malnutrition). Current national and international guidelines for
treatment of acute malnutrition were also assessed from 37 different countries.41
The aim of the MAMI Project was to investigate the management of acutely malnourished infants under six
months of age (infants <6m) in emergency programmes, in order to improve practice by contributing to
evidence-based, best practice and development of guidelines. Main findings are summarised below in box
2.
40 Kerac, M. et al, 2009. Prevalence of wasting among under 6-month-old infants in developing countries and implications of new
case definitions using WHO growth standards: a secondary data analysis. Summarised in a Technical Review; Field Exchange, No
39, pg 19. 2010.
41 The MAMI Project was a collaborative effort between ENN, University College London Centre for International Health and
Development (CIHD) London, and Action Contre la Faim, funded by the UNICEF-led IASC Nutrition Cluster.
37

Box 2: Technical review of the Management of Acute Malnutrition in Infants (MAMI) Project: Current
evidence, policies, practices & programme outcomes
MAMI - A retrospective review of the current field management of moderately and severely
malnourished infants under six months of age
What was already known on this topic:
• Infants aged under 6 months are often excluded from nutrition surveys and marginalised in
malnutrition treatment programmes
• In May 2009, a joint statement from WHO and UNICEF recommended a transition to WHO
growth standards to identify wasting but only reviewed the implications for children aged
from 6 - 59 months
What this study added:
• In developing countries, large numbers of infants under 6 months are wasted; it was
estimated that 0.8 million are severely wasted worldwide and 2.2 million moderately
wasted (diagnosed using NCHS growth references)
• Using WHO standards to diagnose wasting results in a large prevalence increase: an extra 3
million infants under 6 months severely wasted and an extra 2.5 million moderately wasted
worldwide
Principal findings: The data suggested that large numbers of infants under 6 months in developing
countries are wasted. Prevalence is greatest when using WHO growth standards to define cases;
severe infant wasting prevalence is 3.5 times greater than when using NCHS references. By
comparison, severe child wasting is 1.7 times greater using WHO standards. Moderate wasting of
infants under 6-months is 1.4 times greater, whereas moderate child wasting decreases.
Conclusions: Whether defined by NCHS references or WHO standards, wasting among infants
under-6 months is prevalent in many of the developing countries examined in this study. Use of
WHO standards to define wasting results in a greater disease burden, particularly for severe
wasting. Policy makers, programme managers and clinicians in child health and nutrition
programmes should consider resource and risk/benefit implications of changing case definitions.
5.1.1 Implications for Ethiopia from the MAMI project findings
Results from the MAMI project suggest that there may be a considerable (and currently undetected) case-
load of acutely malnourished infants in Ethiopia, and the move to the WHO GS will ensure that this case-
load more than doubles. Most selective feeding interventions implemented to date in Ethiopia have not
focussed on this group, more often targeting lactating women who are themselves MAM (according to
MUAC), but not those infants of women who have difficulty breast-feeding, or those infants who have
started a period of acute malnutrition; which not only raises the immediate risk of mortality, but is also
likely to rapidly lead to growth faltering.
It is important for programmes to identify this highly vulnerable group and refer for appropriate counselling
and treatment, in order to have additional impact on the infant mortality rate in Ethiopia. The vicious cycle
of infection and undernutrition is especially powerful for infants; a sick baby can rapidly deteriorate into a
malnourished baby, with a greatly increased chance of death.
38

The role of the Community Based Nutrition (CBN) programme42 is to capture and help prevent growth
faltering, but as height is not taken, infants starting an acute period of malnutrition could be missed.
Additionally, it is often preferred to keep sick infants within the house, so their presence at CBN gatherings
might not be guaranteed and the CBN programme is currently operational only in the most food insecure
woredas of Ethiopia.
5.1.2 Identification and response
It can be difficult to measure acute malnutrition in infants under-6 months of age, with no internationally
agreed MUAC cut-off to identify malnutrition in this age group. MAM in infants can only therefore be
identified through the use of WHO GS, using z-scores. In terms of accuracy, where staff have not had
sufficient training in anthropometric measurements and because the legs of infants may not straighten as
well as older children, it can be difficult to measure length; small errors might considerably alter the WFH z-
scores of the infant. 43
The HEWs and community health workers are therefore the essential community tool for identifying this
(currently hidden) case-load; through identifying and encouraging the caregivers to urgently attend the
health post for nutritional screening and counselling:
Women who are experiencing difficulty breast-feeding
Those infants where there are no opportunities for breast-feeding (e.g. mother has died and no
‘wet nurse’ available)
Infants having acute periods of infectious disease such as, diarrhoea respiratory infections, malaria,
etc.
Interventions need to be carefully planned in advance. Wherever possible, awareness and expertise in
infant feeding and the provision of breast-feeding support is essential. Where there is limited capacity
amongst the health workers in maternal and infant nutritional requirements (including breastfeeding
assessment, management and support), training sessions should urgently be facilitated by suitably qualified
personnel. The current Sphere recommendations (2011) for the malnutrition treatment programmes do
not provide specific indicators regarding infants under 6 months; however in recognition of the importance
of implementing these ‘life-saving IYCF interventions’ during emergency and non-emergency situations,
two new standards have been introduced.44
IYCF standard 1: Policy guidance and coordination
Safe and appropriate infant and young child feeding for the
population is protected through implementation of key policy
guidance and strong coordination.
IYCF standard 2: Basic and skilled support
Mothers and caregivers of infants and young children have
access to timely and appropriate feeding support that minimises
risks and optimises nutrition, health and survival outcomes.
42 The CBN is currently operational in more than 200 woredas and provides preventative nutritional support including growth
monitoring and promotion (GMP) for children under-2, followed by community conversations with women and other key village
members.
43 En-net discussion: http://fex.ennonline.net/36/prevalence.aspx. - date accessed - June 2011.
44 The Sphere Project. Humanitarian Charter and Minimum Standards in Disaster Response. Geneva, 2011 Edition. Sphere Project.
Hobbs Publishing, UK. www.sphereproject.org
39

Sphere also recommended that breast-feeding mothers of infants with acute malnutrition should be
admitted to MAM treatment programmes, regardless of their nutritional status.
Appropriate responses for interventions that identify and target women and malnourished infants
emphasise intensively supporting or re-establishing appropriate and successful breast-feeding, wherever
possible. Where breast-feeding is not possible, support for artificial feeding should be given. MAM
programme implementers must recognise that that this process will take considerable time on the part of
the health/community worker, and also require sufficient expertise. Enough time must be provided for
training and supervision at community level, where most of the counselling needs to take place.
Infants with MAM should receive similar support as those with SAM, including extensive support for
mothers with breastfeeding and optimal health and hygiene behaviours. Detailed information regarding
these practices is provided in the National Protocol for the Management of SAM (FMoH 2007), including
supplementary suckling techniques, so is not repeated here.
For full information regarding guidance for IYCF programming, refer to the Ethiopian F-MoH National
Strategy for IYCF (April 2004).
Further information can also be sourced from the ‘Infant feeding in Emergencies (IFE) module 2, follow this
link:
http://www.who.int/nutrition/publications/emergencies/ife_module2/en/index.html
For operational guidance on IFE, follow this link:
www.ennonline.net/ife
Part 4 of the IYCF module in the HTP, lists key resources and sources for IYCF in emergency situations,
follow this link:
http://www.unscn.org/en/gnc_htp/howto-htp.php#howtousehtp
5.2 Maternal nutrition health
Maternal undernutrition rates in Ethiopia are also amongst the highest in the world, with one in three
suffering from undernutrition. Maternal mortality rates are particularly high. It is well known by now
amongst the international community that much of the stunting that occurs in children is predetermined at
birth; low birth weight (LBW) infants, defined as those that weigh < 2.5 kg at birth. They are described in
terms of being ‘undernourished’ because they were deprived of essential energy and nutrients before they
were born. While in developed countries, Intra Uterine Growth Retardation (IUGR) may be more associated
with risk factors such as maternal smoking, in less developed countries, it is maternal undernutrition that
most often leads to the birth of small infants; undernourished infants are then at risk for a host of potential
illnesses, many of which may be fatal.
Any newborn infant is highly vulnerable; for the LBW infant, this vulnerability is magnified. Healthy, well-
nourished women do not generally give birth to LBW infants. It is evident therefore that poor foetal
growth results from undernutrition in women. Maternal macro- and micronutrient deficiencies can be
particularly damaging to the functioning both to her child’s present, and future, cognitive, developmental
and immune systems.45
45 Black, R., Allen, L. H., Bhutta, Z. A., Caulfield, L. E., De Onis, M., Ezzati, M., Mathers, C., and Rivera, J. For the Maternal and
Child Undernutrition Study Group. Maternal and child undernutrition: global and regional exposures and health consequences. The
Lancet. Published online Jan 17 2008.
40

SFPs do target undernourished PLW and must continue to do so. But a stronger focus is also needed to
develop understanding through enhanced education of the importance of the woman consuming (at least
most of) the ration allocated for her.
Recommendations for strengthening maternal nutrition health programming include:
Linkages with CBN, PSNP and other major bilateral projects need to be urgently strengthened. The
catchment population of these programmes is likely to not only include beneficiaries who are
pregnant and/or breast-feeding women, but also their husbands (who are often in charge of
household expenditure), leaders and other community members. Strengthened linkages with these
programmes therefore present an unique opportunity to reach wider and more diverse audiences
than SFP alone
Even if the women are not currently undernourished, encouragement for ‘healthy pregnancies’ can
be provided. Ante-Natal Care (ANC) is a vital part of ensuring healthy foetal growth, which results in
stronger infants better able to withstand the rigors of being born into poor households with limited
dietary diversity, education, resources and optimal WASH practices
Deeper analysis of the prevailing gender issues in Ethiopia is suggested, as enduring gender
inequalities are likely to be one of the major underlying causes of undernutrition across the country
5.3 Urban and pastoralist issues
5.3.1 Urban issues
Ethiopia’s population is undergoing steadily increasing urbanisation.46 Nutrition services in most large cities
and towns are poorly developed at present, see box 3 below:
Box 3: Urban issues
(Source – Harmonised Training Package. Module 12: Management of MAM, technical notes, version 2:
2011)
There are several issues related to addressing MAM in urban contexts. The scale of the problem of
malnutrition in urban contexts is largely hidden, given that very few anthropometric surveys have
been undertaken in this context in Ethiopia. Disparities in economic status between groups can also
be obscured through anthropometric surveys with only a single estimate of GAM for the population,
while sampling to obtain estimates of GAM for separate groups can be resource intensive. Population
density, issues of overcrowding and disease transmission, along with higher HIV and TB levels, poor
sanitation and limited capacity for household level agricultural production exacerbate the underlying
causes of malnutrition. For example, food access is often more of an issue than food availability. A
more appropriate response to MAM in this instance could be cash or voucher transfers rather than
traditional blanket or targeted SFPs.1 In cities where household registration is required, this and other
socio-cultural issues of urban living can be important. Security issues are also often different in urban
settings than in rural or camp settings.
These issues underline how anthropometric survey results need to be complemented by other
available information during the assessment and design phase of programmes to address MAM.
Given increasing urbanisation globally, further clarity on best practice for addressing MAM in urban
populations is needed.
46 Ethiopian DHS, 2005. Central Statistics Agency
41

5.3.2 Pastoralist issues
A number of issues are relevant when identifying and treating MAM in pastoralist populations, briefly
described below:
• The mobile nature of the population; static distribution sites are not usually sufficient for mobile
populations. Organisations/agencies will be likely to have more effective programmes if mobile
distribution sites are organised, according to where the population is likely to be heading. As much
information as possible should be sourced from local officials and community leaders, both prior to
setting up a new programme and on an ongoing basis, as situations may change according to
rainfall patterns or available pasture
• Pastoralist populations often face considerable difficulties with water supply, which should be
taken into consideration during the planning phase of the programme. Water trucking might be an
appropriate adjunct to a MAM treatment programme. Distribution teams must ensure that they
bring enough water to the sites (in jerry cans or other suitable containers) to ensure that
beneficiaries and staff are sufficiently hydrated
• Milk is an integral part of the pastoralist diet, providing a vital contribution to the improvement of
dietary quality for women and young children. During times of drought, milk access is considerably
reduced due to the weak state and/or death of their livestock.47 To improve the nutritional status
of these vulnerable groups and where resources allow, treatment programmes should strive to
include some form of milk or milk protein in the ration; for example through the mixing of milk
powder into the dry ration, or using one of the lipid based products that contains milk protein
• Questions have been raised about suitable indicators and criteria for evaluating levels of wasting
that constitute an ‘emergency’ in pastoralist livelihood zones.48 Differences in growth or body
shape may have the effect of overestimating the prevalence of wasting measured by WFH in
pastoralist children aged 2 years and above, in both emergency and non-emergency situations.
While investigations into the most suitable indicators and criteria for pastoralist populations are
still in the early stages and WFH remains an indicator recommended by WHO, the use of MUAC to
define wasting in these populations will be particularly useful to contribute to both the national
and international national learning agenda
47 Sadler, K. Kerven, C. Calo, M. Manske, M. and Catley, A. (2009). Milk Matters: A literature review of pastoralist nutrition and
programming responses. Feinstein International Centre, Tufts University and Save the Children, Addis Ababa.
48 Chotard, S. Mason, J.B. Oliphant, N.P. Mebrahtu, S. and Hailey, P. Fluctuations in wasting in vulnerable child populations in the
Greater Horn of Africa. Child nutrition in vulnerable populations in Eastern and Southern Africa, 2000–2006. Food and Nutrition
Bulletin. Volume 31, Number 3, September 2010
42

References
Black, R., Allen, L. H., Bhutta, Z. A., Caulfield, L. E., De Onis, M., Ezzati, M., Mathers, C., and Rivera, J. For the Maternal
and Child Undernutrition Study Group. Maternal and child undernutrition: global and regional exposures and health
consequences. The Lancet. Published online Jan 17 2008. DOI:10.1016/S0140-6736(07)61690-0
Chotard, S. Mason, J.B. Oliphant, N.P. Mebrahtu, S. and Hailey, P. Fluctuations in wasting in vulnerable child
populations in the Greater Horn of Africa. Child nutrition in vulnerable populations in Eastern and Southern Africa,
2000–2006. Food and Nutrition Bulletin. Volume 31, Number 3, September 2010CSA. Ethiopia Census 2007. Central
Statistics Agency.
CSA. Ethiopia Demographic and Health Survey, 2005. Central Statistics Agency.
DRMFSS (MOARD). National Guidelines on Targeting Relief Food Assistance. Ministry of Agriculture (Disaster Risk
Management and Food Security Sector), Addis Ababa, Ethiopia.2011
EHNRI. The National Nutrition Survey, 2010. Ethiopian Health and Nutrition Research Institute.
ENN. Harmonised Training Package (HTP) Module 12: Management of MAM, technical notes, version 2: 2011.
http://www.ennonline.net/pool/files/ife/management-of-moderate-acute-malnutrition-technical-notes.pdf
FMoH. Concept note for the Management of MAM. Ethiopian Federal Ministry of Health, 2010.
FMoH. Protocol for the Management of Severe Acute Malnutrition, Ethiopia, Federal Ministry of Health (FMoH),
March 2007.
Guyon, AB and Quinn, VJ. Booklet on Key Essential Nutrition Actions Messages. Core Group, Washington, D.C., January
2011
Heikens, G. T., Amadi, B. C., Manary, M., Tollins, N., and Tomkins, A. Nutrition interventions need improved
operational capacity. The Lancet. Published online Jan 17 2008. DOI:10.1016/S0140-6736(07)61690-0
IASC Nutrition Cluster and Nutrition Working Group of the Somalia Support Secretariat. Moderate Acute Malnutrition
Guidelines, 2009
Kerac, M. et al, 2009. Prevalence of wasting among under 6-month-old infants in developing countries and
implications of new case definitions using WHO growth standards: a secondary data analysis. Summarised in a
Technical Review; Field Exchange, No 39, pg 19. 2010.
MoHS. National Protocol for CMAM, Ministry of Health and Sanitation, Sierra Leone, 2010
Myatt, M., and Duffield, A. (2007) Assessing the impact of the introduction of the World Health Organisation (WHO)
growth standards on the measured prevalence of acute malnutrition and the number of children eligible for
admission to emergency feeding programmes. Background paper
Myatt, M., Khara, T., and Collins, S. A review of methods to detect cases of severely malnourished children in the
community for admission into community-based therapeutic programmes. Food and Nutrition Bulletin. Vol 27. No 3
(Suppl). 2006:S7-23.
Myatt, M. New Method for Estimating Programme Coverage. Mark Myatt presentation at an interagency workshop on
Community-based Approaches to Managing Severe Malnutrition. Dublin 8-10th October 2003.
http://fex.ennonline.net/21/coverage.aspx
Navarro-Colorado, C., Shoham, J., Mason, F. Measuring the effectiveness of Supplementary Feeding Programmes in
Emergencies. Working Paper HPN Network Papers 63, August 2008.
43

de Onis, M., Onyango, A. W., Borghi, E., Garza, C., Yang, H. (2006) Comparison of the World Health Organisation
(WHO) child growth standards and the National Centre for Health Statistics/WHO international growth reference:
implications for child health programmes. Public Health Nutrition 9: 942-947
Sadler, K. Kerven, C. Calo, M. Manske, M. and Catley, A. (2009). Milk Matters: A literature review of pastoralist
nutrition and programming responses. Feinstein International Centre, Tufts University and Save the Children, Addis
Ababa.
Seal, A., and Kerac, M. (2007) Operational implications of using the 2006 World Health Organisation growth standards
in nutrition programmes: secondary data analysis. British Medical Journal. DOI:10.1136
Sphere Project. Humanitarian Charter and Minimum Standards in Disaster Response. Geneva. 2011 Edition. Sphere
Project. Hobbs Publishing, UK. www.sphereproject.org
UNICEF. A toolkit for addressing nutrition in emergency situations. IASC Global Nutrition Cluster, New York, NY, 2008
UNICEF and IFPRI coordinated effort, 2005. An Assessment of the causes of Malnutrition in Ethiopia: A contribution to
the formulation of a National Nutrition Strategy for Ethiopia (Background Papers)
UNHCR/UNICEF/WFP/WHO. Food and Nutrition Needs in Emergencies. Geneva, 2003.
http://www.unhcr.org/publ/PUBL/45fa745b2.pdf
UNHCR/WFP. A guide for selective feeding programmes, Geneva, May 2009.
Valid International. Community-Based Therapeutic Care (CTC); A Field Manual. Valid International. First Edition, 2006.
44
Annex 1: Weight-for -height reference tables, girls and boys, World Health Organisation
Growth Standards (WHO-GS), 2006
-4SD
1,7
1,8
1,8
1,9
2,0
2,0
2,1
2,1
2,2
2,3
2,4
2,4
2,5
2,6
2,7
2,8
2,9
3,0
3,1
3,2
3,3
3,4
3,5
3,6
3,7
3,8
3,9
4,0
4,1
4,2
4,3
4,4
4,5
4,6
4,7
4,8
4,9
5,0
5,1
5,2
5,3
5,4
5,5
5,5
5,6
5,7
5,8
5,9
6,0
6,0
6,1
6,2
6,3
6,4
6,4
6,5
6,6
6,7
6,7
6,8
6,9
7,0
7,0
7,1
7,2
7,2
7,3
7,4
7,4
7,5
7,6
7,6
7,7
7,8
7,9
7,9
8,0
8,1
8,2
8,3
Boys weight (kg)
-3SD
1,9
1,9
2,0
2,1
2,1
2,2
2,3
2,3
2,4
2,5
2,6
2,7
2,7
2,8
2,9
3,0
3,1
3,2
3,3
3,4
3,6
3,7
3,8
3,9
4,0
4,1
4,3
4,4
4,5
4,6
4,7
4,8
4,9
5,0
5,1
5,2
5,3
5,4
5,5
5,6
5,7
5,8
5,9
6,0
6,1
6,2
6,3
6,4
6,5
6,6
6,6
6,7
6,8
6,9
7,0
7,1
7,2
7,2
7,3
7,4
7,5
7,6
7,6
7,7
7,8
7,9
7,9
8,0
8,1
8,2
8,2
8,3
8,4
8,5
8,5
8,6
8,7
8,8
8,9
9,0
-2SD
2,0
2,1
2,2
2,3
2,3
2,4
2,5
2,6
2,6
2,7
2,8
2,9
3,0
3,1
3,2
3,3
3,4
3,5
3,6
3,7
3,8
4,0
4,1
4,2
4,3
4,5
4,6
4,7
4,8
5,0
5,1
5,2
5,3
5,4
5,6
5,7
5,8
5,9
6,0
6,1
6,2
6,3
6,4
6,5
6,6
6,7
6,8
6,9
7,0
7,1
7,2
7,3
7,4
7,5
7,6
7,6
7,7
7,8
7,9
8,0
8,1
8,2
8,3
8,3
8,4
8,5
8,6
8,7
8,7
8,8
8,9
9,0
9,1
9,1
9,2
9,3
9,4
9,5
9,6
9,7
-1SD
2,2
2,3
2,4
2,5
2,5
2,6
2,7
2,8
2,9
3,0
3,0
3,1
3,2
3,3
3,5
3,6
3,7
3,8
3,9
4,0
4,2
4,3
4,4
4,6
4,7
4,9
5,0
5,1
5,3
5,4
5,5
5,6
5,8
5,9
6,0
6,1
6,2
6,4
6,5
6,6
6,7
6,8
6,9
7,0
7,1
7,2
7,3
7,5
7,6
7,7
7,8
7,9
8,0
8,1
8,2
8,3
8,4
8,5
8,6
8,7
8,8
8,9
8,9
9,0
9,1
9,2
9,3
9,4
9,5
9,5
9,6
9,7
9,8
9,9
10,0
10,1
10,2
10,3
10,4
10,5
Median
2,4
2,5
2,6
2,7
2,8
2,9
2,9
3,0
3,1
3,2
3,3
3,4
3,5
3,6
3,8
3,9
4,0
4,1
4,3
4,4
4,5
4,7
4,8
5,0
5,1
5,3
5,4
5,6
5,7
5,9
6,0
6,1
6,3
6,4
6,5
6,7
6,8
6,9
7,0
7,1
7,3
7,4
7,5
7,6
7,7
7,9
8,0
8,1
8,2
8,3
8,4
8,5
8,6
8,8
8,9
9,0
9,1
9,2
9,3
9,4
9,5
9,6
9,7
9,8
9,9
10,0
10,1
10,2
10,3
10,4
10,4
10,5
10,6
10,7
10,8
10,9
11,0
11,2
11,3
11,4
Length (cm)a
45,0
45,5
46,0
46,5
47,0
47,5
48,0
48,5
49,0
49,5
50,0
50,5
51,0
51,5
52,0
52,5
53,0
53,5
54,0
54,5
55,0
55,5
56,0
56,5
57,0
57,5
58,0
58,5
59,0
59,5
60,0
60,5
61,0
61,5
62,0
62,5
63,0
63,5
64,0
64,5
65,0
65,5
66,0
66,5
67,0
67,5
68,0
68,5
69,0
69,5
70,0
70,5
71,0
71,5
72,0
72,5
73,0
73,5
74,0
74,5
75,0
75,5
76,0
76,5
77,0
77,5
78,0
78,5
79,0
79,5
80,0
80,5
81,0
81,5
82,0
82,5
83,0
83,5
84,0
84,5
Median
2,5
2,5
2,6
2,7
2,8
2,9
3,0
3,1
3,2
3,3
3,4
3,5
3,6
3,7
3,8
3,9
4,0
4,2
4,3
4,4
4,6
4,7
4,8
5,0
5,1
5,2
5,4
5,5
5,6
5,7
5,9
6,0
6,1
6,3
6,4
6,5
6,6
6,7
6,9
7,0
7,1
7,2
7,3
7,4
7,5
7,6
7,7
7,9
8,0
8,1
8,2
8,3
8,4
8,5
8,6
8,7
8,8
8,9
9,0
9,1
9,1
9,2
9,3
9,4
9,5
9,6
9,7
9,8
9,9
10,0
10,1
10,2
10,3
10,4
10,5
10,6
10,7
10,9
11,0
11,1
Girls weight (kg)
-1SD
2,3
2,3
2,4
2,5
2,6
2,6
2,7
2,8
2,9
3,0
3,1
3,2
3,3
3,4
3,5
3,6
3,7
3,8
3,9
4,0
4,2
4,3
4,4
4,5
4,6
4,8
4,9
5,0
5,1
5,3
5,4
5,5
5,6
5,7
5,8
5,9
6,0
6,2
6,3
6,4
6,5
6,6
6,7
6,8
6,9
7,0
7,1
7,2
7,3
7,4
7,5
7,6
7,7
7,7
7,8
7,9
8,0
8,1
8,2
8,3
8,4
8,5
8,5
8,6
8,7
8,8
8,9
9,0
9,1
9,1
9,2
9,3
9,4
9,5
9,6
9,7
9,8
9,9
10,1
10,2
-2SD
2,1
2,1
2,2
2,3
2,4
2,4
2,5
2,6
2,6
2,7
2,8
2,9
3,0
3,1
3,2
3,3
3,4
3,5
3,6
3,7
3,8
3,9
4,0
4,2
4,3
4,4
4,5
4,6
4,7
4,8
4,9
5,0
5,1
5,2
5,3
5,4
5,5
5,6
5,7
5,8
5,9
6,0
6,1
6,2
6,3
6,4
6,5
6,6
6,7
6,8
6,9
6,9
7,0
7,1
7,2
7,3
7,4
7,4
7,5
7,6
7,7
7,8
7,8
7,9
8,0
8,1
8,2
8,2
8,3
8,4
8,5
8,6
8,7
8,8
8,8
8,9
9,0
9,1
9,2
9,3
-3SD
1,9
2,0
2,0
2,1
2,2
2,2
2,3
2,4
2,4
2,5
2,6
2,7
2,8
2,8
2,9
3,0
3,1
3,2
3,3
3,4
3,5
3,6
3,7
3,8
3,9
4,0
4,1
4,2
4,3
4,4
4,5
4,6
4,7
4,8
4,9
5,0
5,1
5,2
5,3
5,4
5,5
5,5
5,6
5,7
5,8
5,9
6,0
6,1
6,1
6,2
6,3
6,4
6,5
6,5
6,6
6,7
6,8
6,9
6,9
7,0
7,1
7,1
7,2
7,3
7,4
7,4
7,5
7,6
7,7
7,7
7,8
7,9
8,0
8,1
8,2
8,2
8,3
8,4
8,5
8,6
-4SD
1,7
1,8
1,9
1,9
2,0
2,0
2,1
2,2
2,2
2,3
2,4
2,4
2,5
2,6
2,7
2,8
2,8
2,9
3,0
3,1
3,2
3,3
3,4
3,5
3,6
3,7
3,8
3,9
3,9
4,0
4,1
4,2
4,3
4,4
4,5
4,6
4,7
4,7
4,8
4,9
5,0
5,1
5,1
5,2
5,3
5,4
5,5
5,5
5,6
5,7
5,8
5,8
5,9
6,0
6,0
6,1
6,2
6,3
6,3
6,4
6,5
6,5
6,6
6,7
6,7
6,8
6,9
6,9
7,0
7,1
7,1
7,2
7,3
7,4
7,5
7,5
7,6
7,7
7,8
7,9
Boys weight (kg)
Girls weight (kg)
-4SD
-3SD
-2SD
-1SD
Median Height (cm)a Median
-1SD
8,4
9,1
9,8
10,6
11,5
85,0
11,2
10,3
8,5
9,2
9,9
10,7
11,6
85,5
11,3
10,4
8,6
9,3
10,0
10,8
11,7
86,0
11,5
10,5
8,7
9,4
10,1
11,0
11,9
86,5
11,6
10,6
8,9
9,6
10,4
11,2
12,2
87,0
11,9
10,9
9,0
9,7
10,5
11,3
12,3
87,5
12,0
11,0
9,1
9,8
10,6
11,5
12,4
88,0
12,1
11,1
9,2
9,9
10,7
11,6
12,5
88,5
12,3
11,2
9,3
10,0
10,8
11,7
12,7
89,0
12,4
11,4
9,3
10,1
10,9
11,8
12,8
89,5
12,5
11,5
9,4
10,2
11,0
11,9
12,9
90,0
12,6
11,6
9,5
10,3
11,1
12,0
13,0
90,5
12,8
11,7
9,6
10,4
11,2
12,1
13,1
91,0
12,9
11,8
9,7
10,5
11,3
12,2
13,2
91,5
13,0
11,9
9,8
10,6
11,4
12,3
13,4
92,0
13,1
12,0
9,9
10,7
11,5
12,4
13,5
92,5
13,3
12,1
9,9
10,8
11,6
12,6
13,6
93,0
13,4
12,3
10,0
10,9
11,7
12,7
13,7
93,5
13,5
12,4
10,1
11,0
11,8
12,8
13,8
94,0
13,6
12,5
10,2
11,1
11,9
12,9
13,9
94,5
13,8
12,6
10,3
11,1
12,0
13,0
14,1
95,0
13,9
12,7
10,4
11,2
12,1
13,1
14,2
95,5
14,0
12,8
10,4
11,3
12,2
13,2
14,3
96,0
14,1
12,9
10,5
11,4
12,3
13,3
14,4
96,5
14,3
13,1
10,6
11,5
12,4
13,4
14,6
97,0
14,4
13,2
10,7
11,6
12,5
13,6
14,7
97,5
14,5
13,3
10,8
11,7
12,6
13,7
14,8
98,0
14,7
13,4
10,9
11,8
12,8
13,8
14,9
98,5
14,8
13,5
11,0
11,9
12,9
13,9
15,1
99,0
14,9
13,7
11,1
12,0
13,0
14,0
15,2
99,5
15,1
13,8
11,2
12,1
13,1
14,2
15,4
100,0
15,2
13,9
11,2
12,2
13,2
14,3
15,5
100,5
15,4
14,1
11,3
12,3
13,3
14,4
15,6
101,0
15,5
14,2
11,4
12,4
13,4
14,5
15,8
101,5
15,7
14,3
11,5
12,5
13,6
14,7
15,9
102,0
15,8
14,5
11,6
12,6
13,7
14,8
16,1
102,5
16,0
14,6
11,7
12,8
13,8
14,9
16,2
103,0
16,1
14,7
11,8
12,9
13,9
15,1
16,4
103,5
16,3
14,9
11,9
13,0
14,0
15,2
16,5
104,0
16,4
15,0
12,0
13,1
14,2
15,4
16,7
104,5
16,6
15,2
12,1
13,2
14,3
15,5
16,8
105,0
16,8
15,3
12,2
13,3
14,4
15,6
17,0
105,5
17,0
15,5
12,3
13,4
14,5
15,8
17,2
106,0
17,1
15,6
12,4
13,5
14,7
15,9
17,3
106,5
17,3
15,8
12,5
13,7
14,8
16,1
17,5
107,0
17,5
15,9
12,6
13,8
14,9
16,2
17,7
107,5
17,7
16,1
12,7
13,9
15,1
16,4
17,8
108,0
17,8
16,3
12,8
14,0
15,2
16,5
18,0
108,5
18,0
16,4
12,9
14,1
15,3
16,7
18,2
109,0
18,2
16,6
13,1
14,3
15,5
16,8
18,3
109,5
18,4
16,8
13,2
14,4
15,6
17,0
18,5
110,0
18,6
17,0
13,3
14,5
15,8
17,1
18,7
110,5
18,8
17,1
13,4
14,6
15,9
17,3
18,9
111,0
19,0
17,3
13,5
14,8
16,0
17,5
19,1
111,5
19,2
17,5
13,6
14,9
16,2
17,6
19,2
112,0
19,4
17,7
13,7
15,0
16,3
17,8
19,4
112,5
19,6
17,9
13,8
15,2
16,5
18,0
19,6
113,0
19,8
18,0
14,0
15,3
16,6
18,1
19,8
113,5
20,0
18,2
14,1
15,4
16,8
18,3
20,0
114,0
20,2
18,4
14,2
15,6
16,9
18,5
20,2
114,5
20,5
18,6
14,3
15,7
17,1
18,6
20,4
115,0
20,7
18,8
14,4
15,8
17,2
18,8
20,6
115,5
20,9
19,0
14,6
16,0
17,4
19,0
20,8
116,0
21,1
19,2
14,7
16,1
17,5
19,2
21,0
116,5
21,3
19,4
14,8
16,2
17,7
19,3
21,2
117,0
21,5
19,6
14,9
16,4
17,9
19,5
21,4
117,5
21,7
19,8
15,0
16,5
18,0
19,7
21,6
118,0
22,0
20,0
15,2
16,7
18,2
19,9
21,8
118,5
22,2
20,1
15,3
16,8
18,3
20,0
22,0
119,0
22,4
20,3
15,4
16,9
18,5
20,2
22,2
119,5
22,6
20,5
15,5
17,1
18,6
20,4
22,4
120,0
22,8
20,7
a Using this table, length should be measured from 45 to 86,9 cm and height should be measured from 87 to 120 cm.
-2SD
9,4
9,6
9,7
9,8
10,0
10,1
10,2
10,3
10,4
10,5
10,6
10,7
10,9
11,0
11,1
11,2
11,3
11,4
11,5
11,6
11,7
11,8
11,9
12,0
12,1
12,2
12,3
12,4
12,5
12,7
12,8
12,9
13,0
13,1
13,3
13,4
13,5
13,6
13,8
13,9
14,0
14,2
14,3
14,5
14,6
14,7
14,9
15,0
15,2
15,4
15,5
15,7
15,8
16,0
16,2
16,3
16,5
16,7
16,8
17,0
17,2
17,3
17,5
17,7
17,8
18,0
18,2
18,4
18,5
18,7
18,9
-3SD
8,7
8,8
8,9
9,0
9,2
9,3
9,4
9,5
9,6
9,7
9,8
9,9
10,0
10,1
10,2
10,3
10,4
10,5
10,6
10,7
10,8
10,8
10,9
11,0
11,1
11,2
11,3
11,4
11,5
11,6
11,7
11,9
12,0
12,1
12,2
12,3
12,4
12,5
12,7
12,8
12,9
13,0
13,1
13,3
13,4
13,5
13,7
13,8
13,9
14,1
14,2
14,4
14,5
14,7
14,8
15,0
15,1
15,3
15,4
15,6
15,7
15,9
16,0
16,2
16,3
16,5
16,6
16,8
16,9
17,1
17,3
-4SD
8,0
8,0
8,1
8,2
8,4
8,5
8,6
8,7
8,8
8,9
9,0
9,1
9,1
9,2
9,3
9,4
9,5
9,6
9,7
9,7
9,8
9,9
10,0
10,1
10,2
10,3
10,4
10,4
10,5
10,6
10,7
10,8
10,9
11,0
11,1
11,2
11,3
11,4
11,5
11,6
11,8
11,9
12,0
12,1
12,2
12,3
12,4
12,6
12,7
12,8
12,9
13,1
13,2
13,3
13,5
13,6
13,7
13,9
14,0
14,1
14,3
14,4
14,5
14,7
14,8
15,0
15,1
15,2
15,4
15,5
15,6
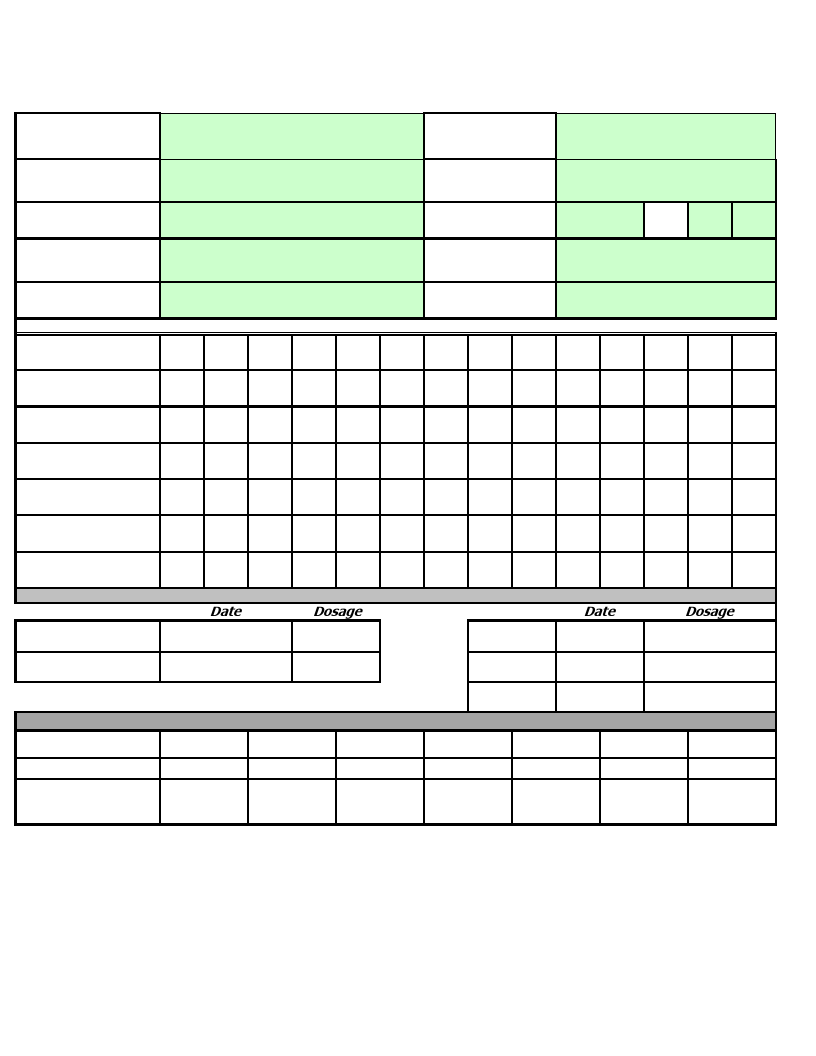

Annex 2 - Ration card; Children 6-59 months, PLW
Source: Adapted from Community-based Therapeutic Care (CTC): A field Manual. VALID International. First Edition, 2006
Childs Name
(include Grandfather's
name)
Gott/Kebele
TSFP RATION CARD; CHILDREN 6-59 MONTHS
Registration Number
Facility/ Distribution
Site
Admission date
W/H z-score
Age (months)
MUAC (cm)
sex M
F
Admission weight
TARGET WEIGHT
Distribution/Week
Date
Weight (kg)
Height (cm)
W/H z-score
MUAC (cm)
Type and amount of food
(kg)
Medication
Vitamin A (IU)
De-worming (mg)
Date
Visit date
Visit signature
Comment
Routine Admission Medication
Dosage
Medication
Measles
Anti malarial
Other
Additional Information
Date
Dosage
.

TSFP RATION CARD; PREGNANT or LACTATING WOMEN
Mother's Name
Admission MUAC (cm)
Admission Date
Preg expected delivery
date
Gott
Baby reach 6
month date
Registration Number
Kebele
Facility/
Distribution
Site
Distribution/Week
Date
MUAC (cm)
Type and amount of food
(Kg)
Medication
Vitamin A (IU)
Date
Dosage
Notes:
Medication
De-worming
Date
Dosage
.

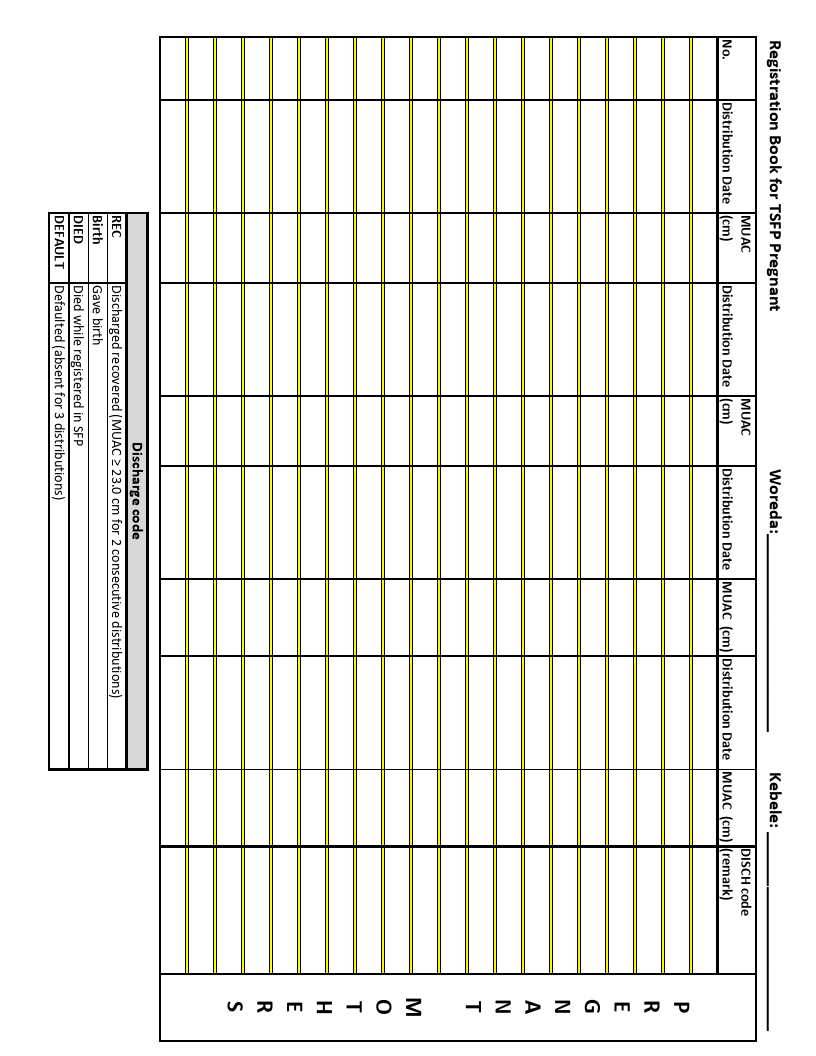
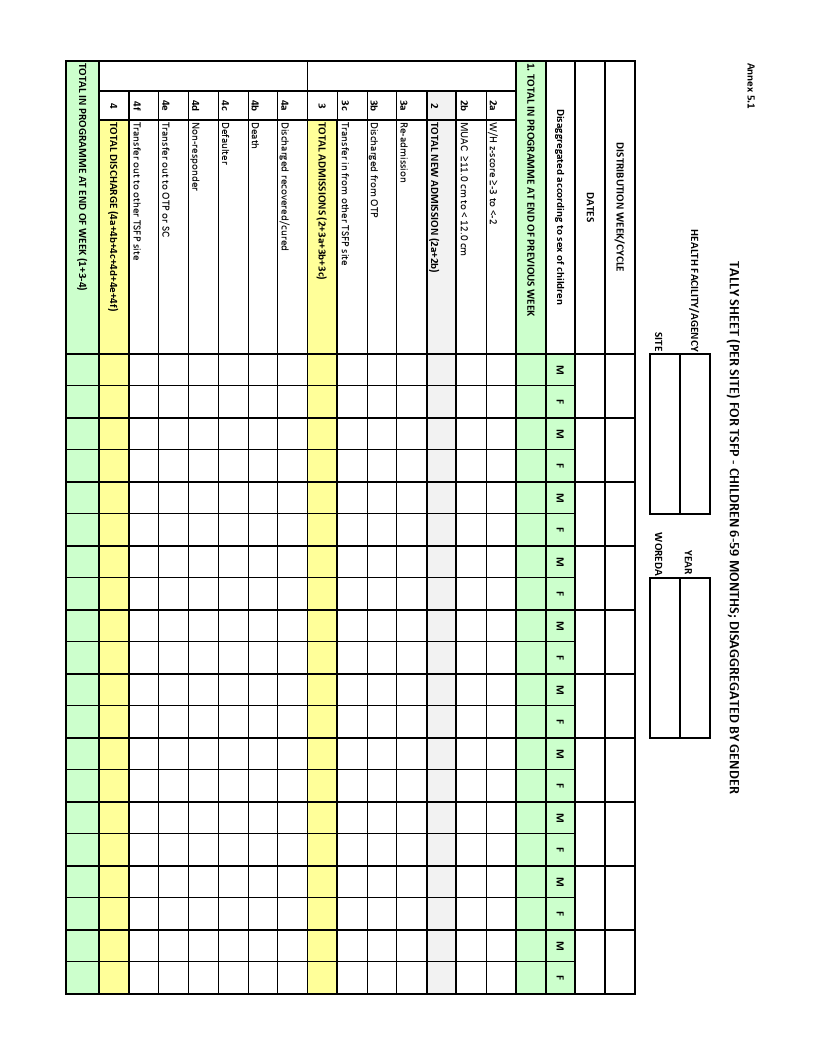
ADMISSION
EXIT
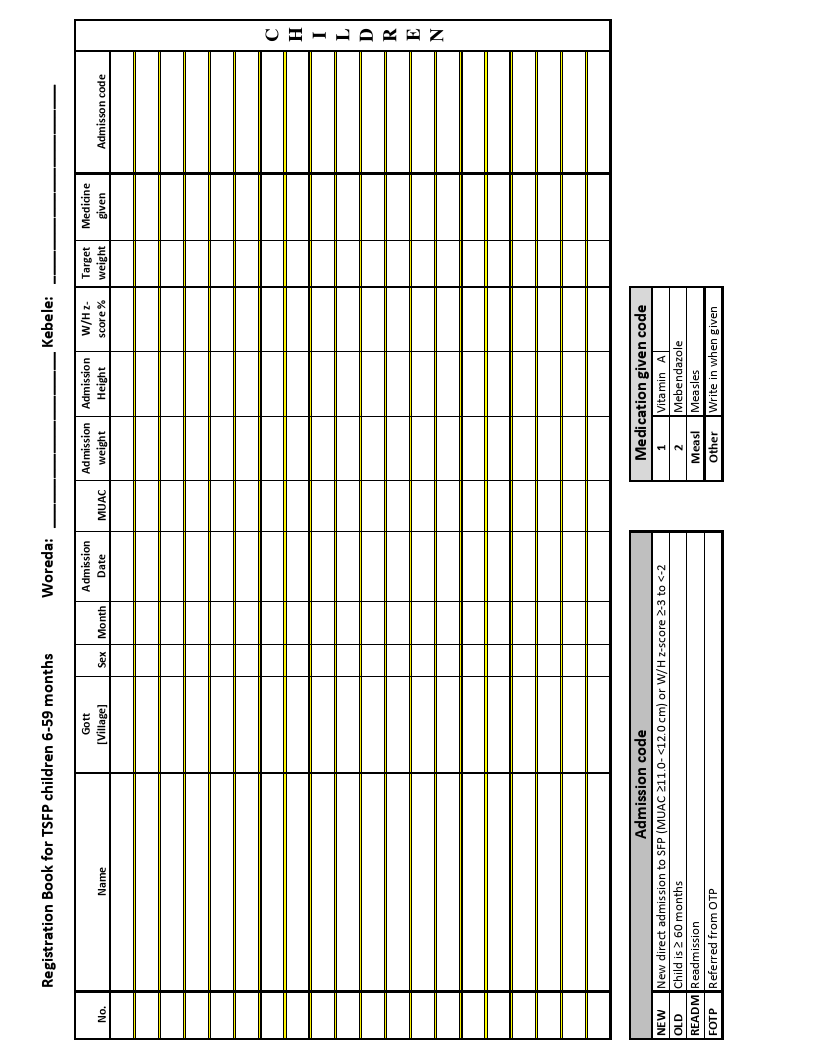
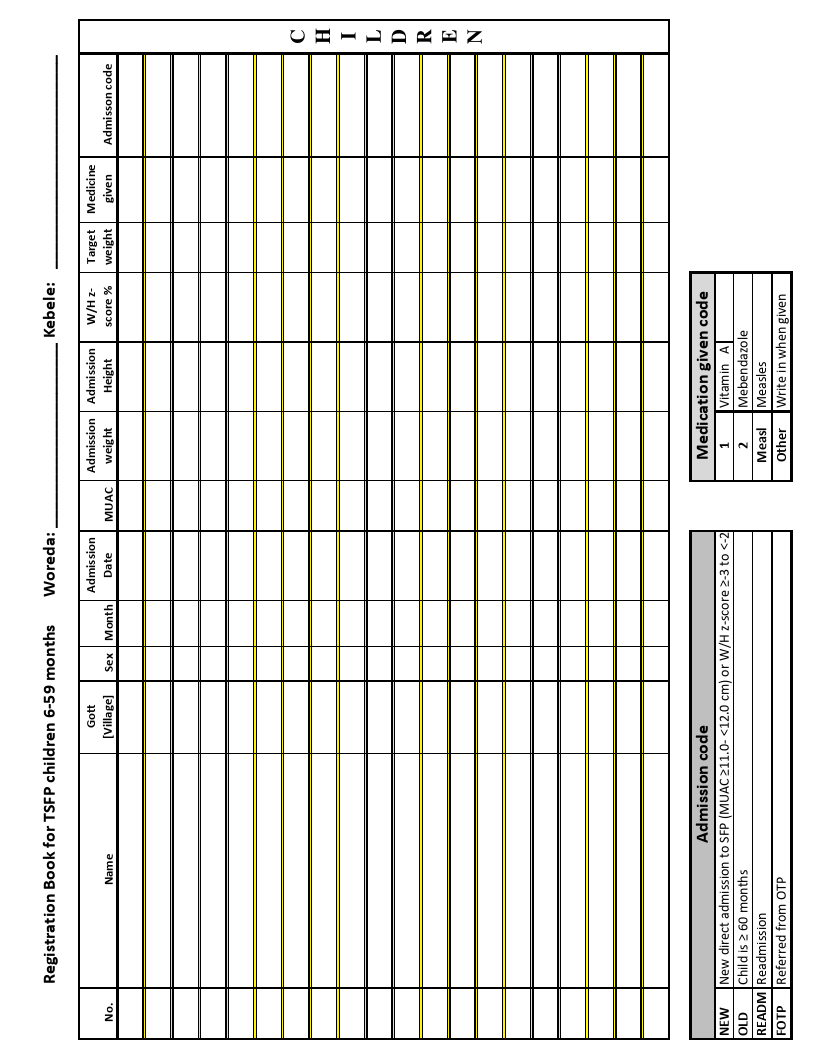




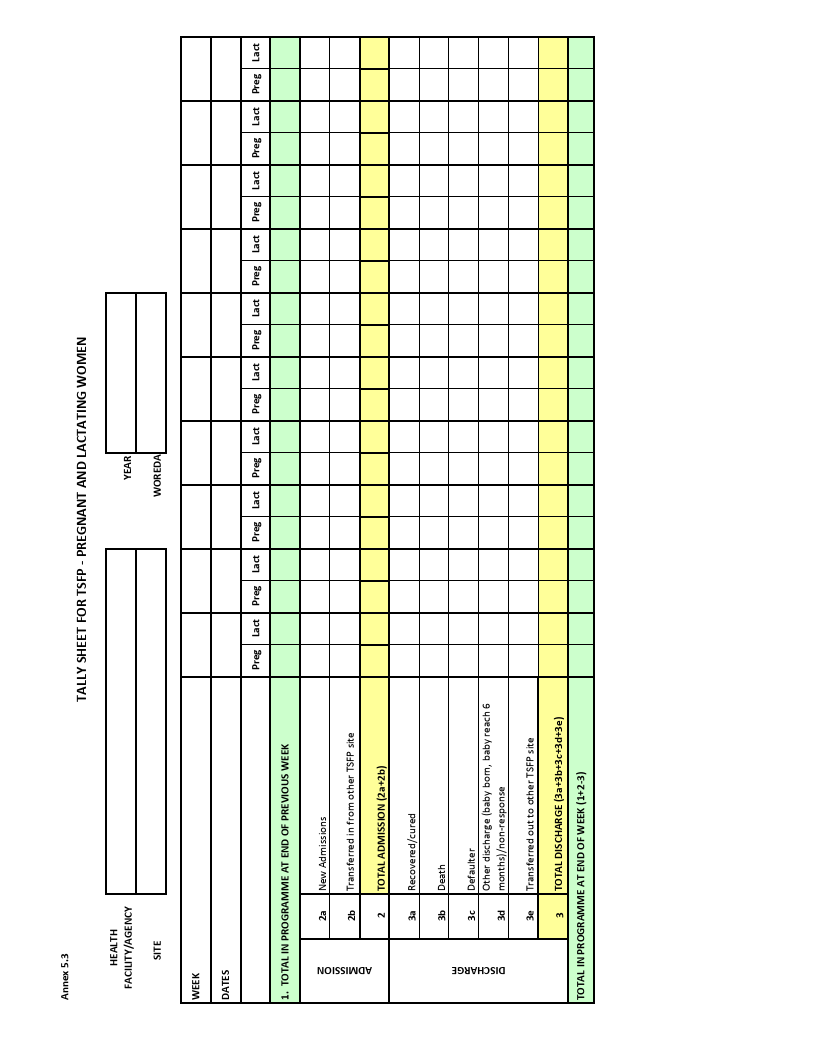
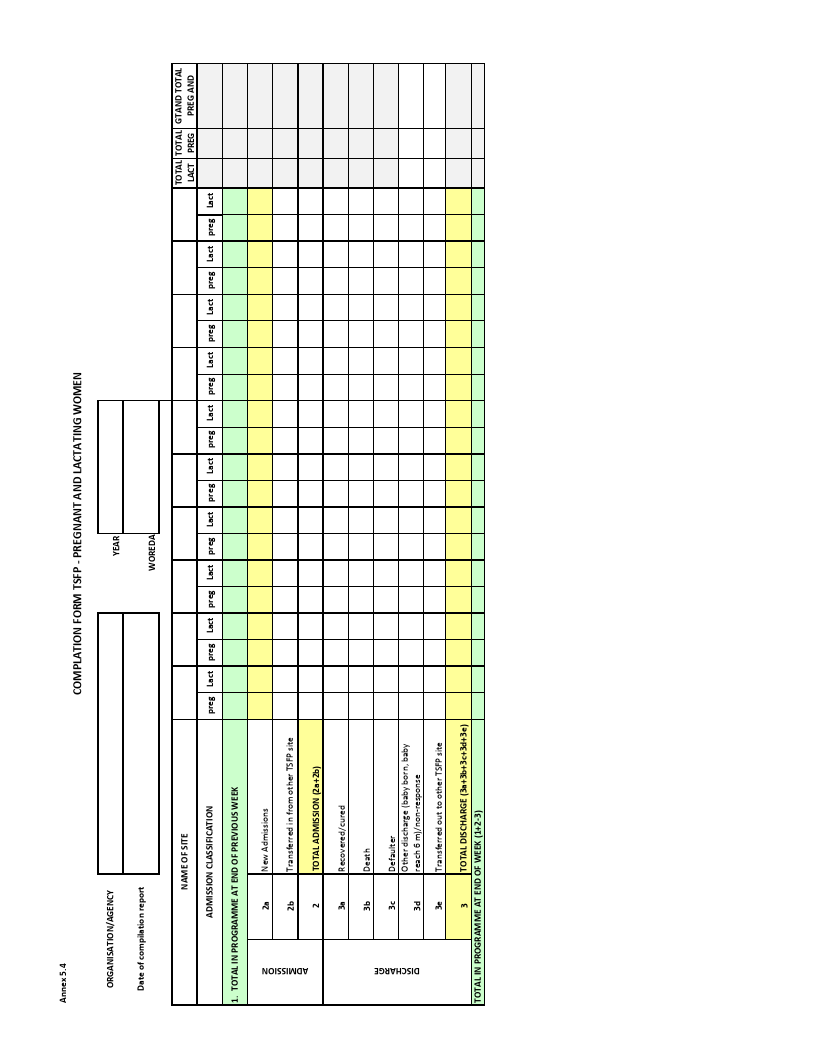
Annex 7: Supervision checklist TSFP
TSFP Facility/Distribution Site:
Kebele:
_____________
Woreda:
Date:
Zone:
Region:
Activity
Quality
(Poor, Average,
Good)
Discussed with
supervisor
(Y/N)
Registration numbers allocated
correctly
Weight measured accurately
Height measured accurately
Weight-for-Height calculated correctly
MUAC measured accurately
Oedema measured accurately
Information recorded on card and in
registration book
Beneficiary correctly referred to either
TSFP, OTP, TFU, hospital or home
Admission medication given according
to protocol and recorded
Children with no measles vaccination
referred to nearest health facility
Correct amount of food distributed
Follow up weight, MUAC and height
recorded correctly
Appropriate education given to
caretakers and TSFP beneficiaries
Cooking demonstrations conducted
Beneficiaries discharged according to
protocol.
Absentee and defaulter beneficiaries
being followed up in the community
Home visit and post-distribution
monitoring being conducted by
community workers
TSFP tally and compilation sheets
correctly completed (spot check with
cards)
TSFP monthly reports accurately
completed
Sufficient stocks of supplementary
food and other supplies available to
implement the programme
Food commodities and other stock
stored correctly
Comment
Annex 8: Suggested equipment and supplies required for TSFP
(per Health Facility/distribution site)
Item
1 TSFP file for admission cards
2 Pens
3 Calculator
4 Water jug (with lid)
5 Plastic cups
6 Teaspoons or medicine cups
7 Thermometer
8
Salter scale (25kg) and pants; ‘Mother and Child’
Weighing scale
9 Height board
10 MUAC tapes
National Protocol for the management of MAM;
11 admission and discharge criteria, Weight for Height z-
score reference tables
Scale/balance to measure food ration or
12 calibrated container that holds known weight
of food ration
Minimum stock to keep topped up
1 TSFP ration cards for new admissions
2 ID bracelets (optional)
3 Clear plastic envelopes for filing cards (optional)
4 Drinking water
5 Food: e.g. FBF
6 Routine medicines - Vitamin A and de-worming
Amount per Health Facility/ distribution site
1
3
1
2
20
6
2
1-2 depending on caseload at each site
1-2 depending on caseload at each site
4
1
1
Amount per Health facility/distribution site
100
100
100
1-4 jerry cans or at hand-washing station
Depends on expected case-load
Depends on expected case-load
Annex 8: Suggested equipment and supplies required for TSFP
(per Health Facility/distribution site)
Item
1 TSFP file for admission cards
2 Pens
3 Calculator
4 Water jug (with lid)
5 Plastic cups
6 Teaspoons or medicine cups
7 Thermometer
8
Salter scale (25kg) and pants; ‘Mother and Child’
Weighing scale
9 Height board
10 MUAC tapes
National Protocol for the management of MAM;
11 admission and discharge criteria, Weight for Height z-
score reference tables
Scale/balance to measure food ration or
12 calibrated container that holds known weight
of food ration
Minimum stock to keep topped up
1 TSFP ration cards for new admissions
2 ID bracelets (optional)
3 Clear plastic envelopes for filing cards (optional)
4 Drinking water
5 Food: e.g. FBF
6 Routine medicines - Vitamin A and de-worming
Amount per Health Facility/ distribution site
1
3
1
2
20
6
2
1-2 depending on caseload at each site
1-2 depending on caseload at each site
4
1
1
Amount per Health facility/distribution site
100
100
100
1-4 jerry cans or at hand-washing station
Depends on expected case-load
Depends on expected case-load
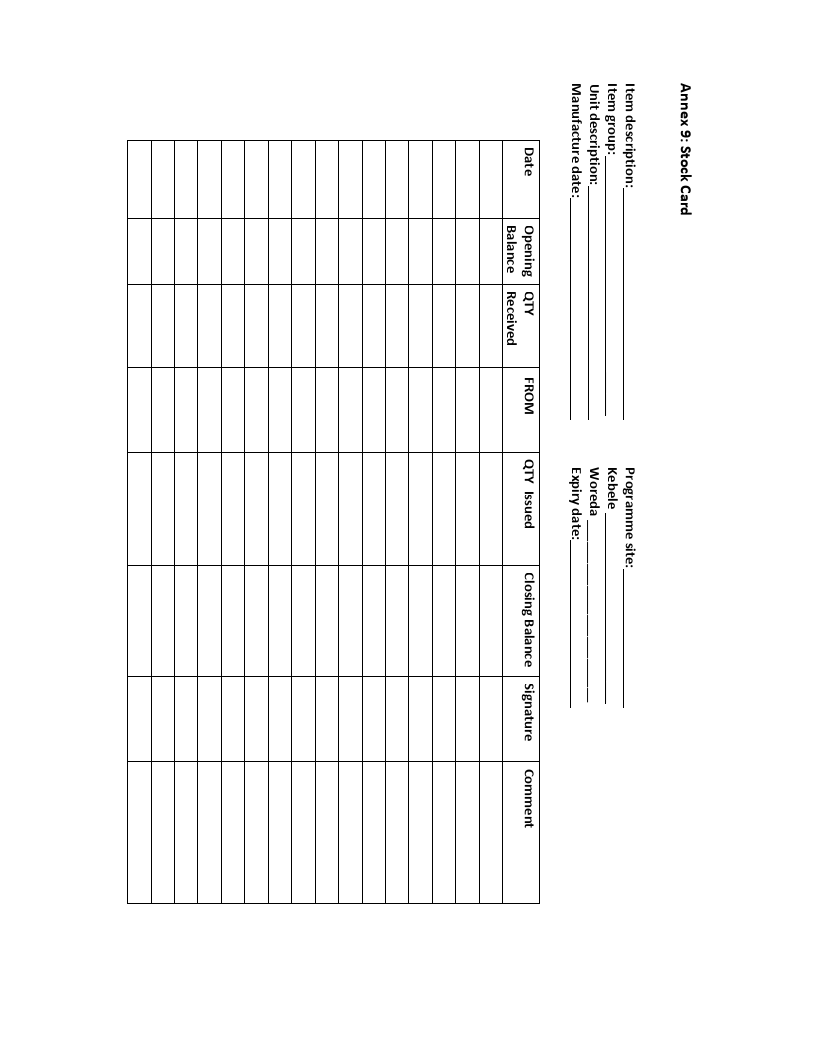


Annex 10: Anthropometric measurement techniques:
10.1 Checking for bilateral pitting oedema
10.2 Measuring the MUAC
10.3 Taking the height/length
10.4 Weighing using a standing scale
10.5 Weighing using Salter scales
10.1 Checking for bilateral oedema
Bilateral oedema is the sign of Kwashiorkor. Kwashiorkor is always a severe form of malnutrition.
Children with bilateral oedema are directly identified to be acutely malnourished. These children are
at high risk of mortality and need to be treated in a therapeutic feeding programme urgently.
In order to determine the presence of oedema, normal thumb pressure is applied to both feet for three
seconds. If a shallow print persists on both feet, then the child presents with oedema. Only children with
bilateral oedema are recorded as having nutritional oedema.
You must formally test for oedema with finger pressure
you cannot tell by just looking
Mild oedema: usually confined to feet or pre-tibial area
+
Moderate oedema on feet and legs: Intermediate between mild and severe
++
Severe oedema generalised over the whole body: deep lasting pit formed
+++
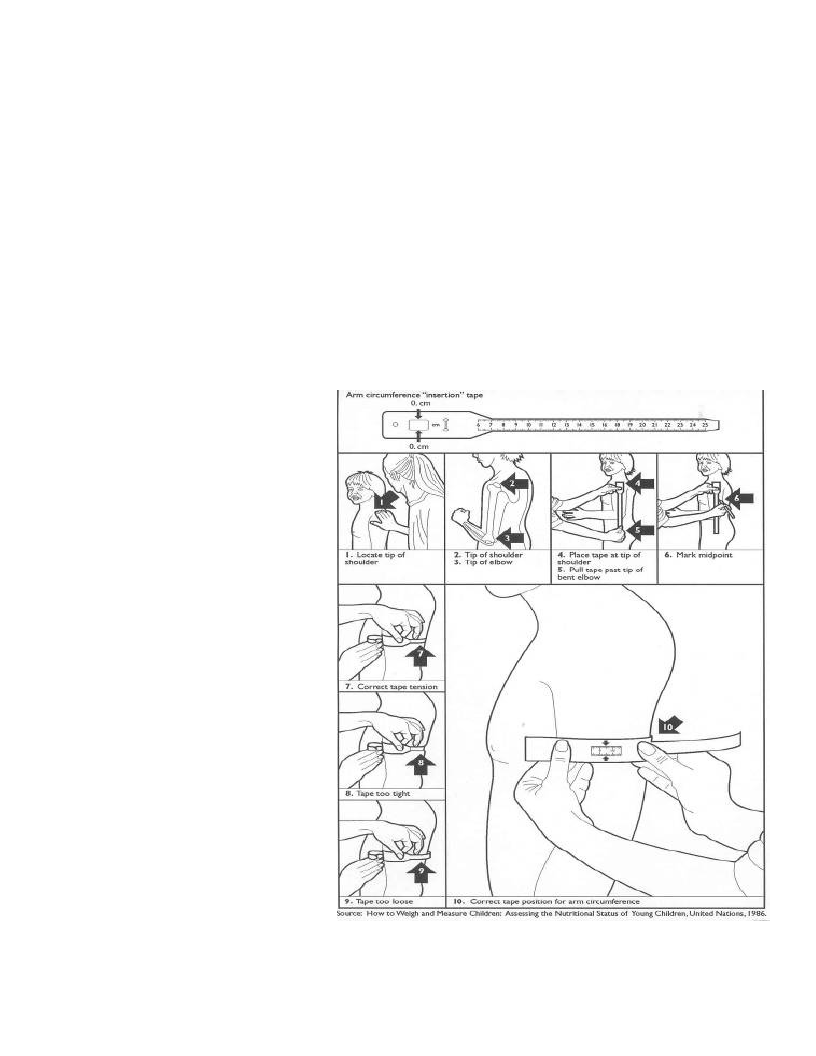
10.2 Taking the Mid-upper Arm Circumference (MUAC) measurement
MUAC is used in children from 6-59 months. It is also used for adolescents, adults and pregnant and
lactating women.
For MUAC measurement in children, follow the steps below and the corresponding picture:
1. Ask the mother to remove clothing that may cover the child’s left arm.
2. Calculate the midpoint of the child’s left upper arm by first locating the tip of the child’s
shoulder (arrows 1 and 2) with your finger tips. Bend the child’s elbow to make a right angle
(arrow 3). Place the tape at zero, which is indicated by two arrows, on the tip of the shoulder
(arrow 4) and pull the tape straight down past the tip of the elbow (arrow 5). Read the number
at the tip of the elbow to the nearest centimetre. Divide this number by two to estimate the
midpoint. As an alternative, bend the tape up to the middle length to estimate the midpoint. A
piece of string can also be used for this purpose; it is more convenient and avoids damage to the
tape. Mark the midpoint with a pen on the arm (arrow 6).
3. Straighten the child’s arm and
wrap the tape around the
arm at the midpoint. Make
sure the numbers are right
side up. Make sure the tape is
flat around the skin (arrow 7).
4. Inspect the tension of the
tape on the child’s arm.
Make sure the tape has the
proper tension (arrow 7) and
is not too tight or too loose
(arrows 8 and 9). Repeat any
step as necessary.
5. When the tape is in the
correct position on the arm
with correct tension, read out
the measurement to the
nearest 0.1cm (arrow 10).
6. Immediately record the
measurement.
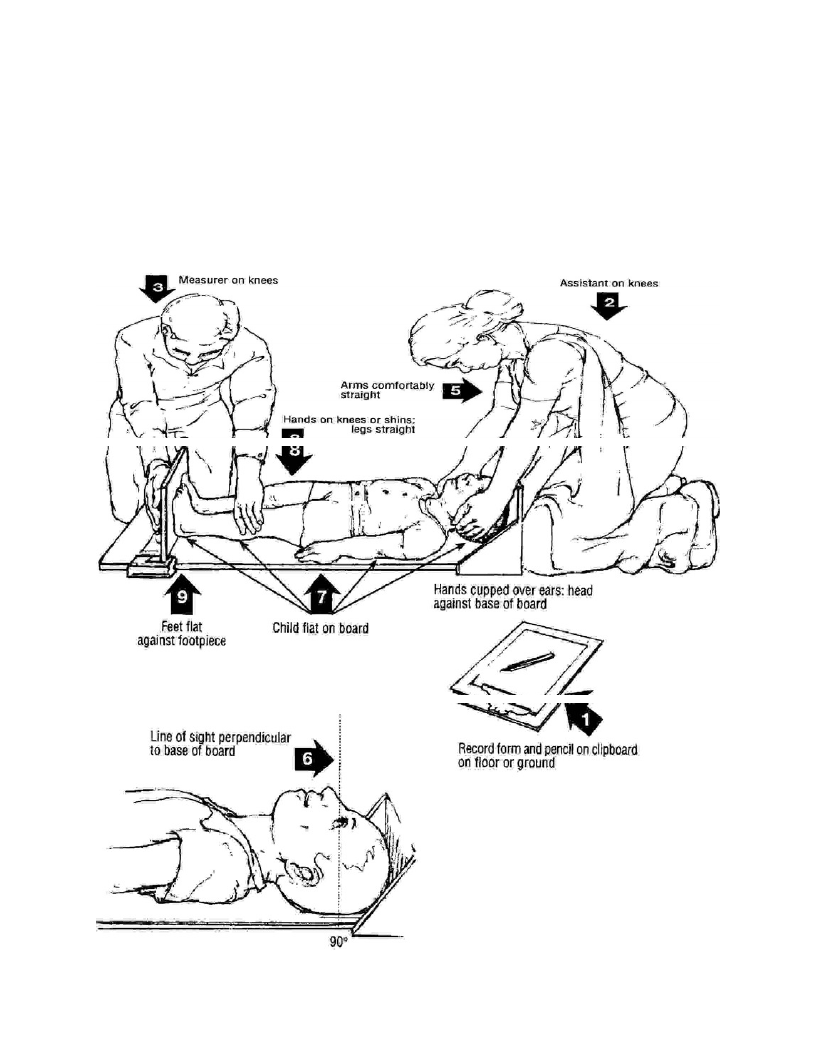
10.3 Measuring the length/height
For children less than 87 cm, the measuring board is placed on the ground. The child is placed, lying
along the middle of the board. The assistant holds the sides of the child’s head and positions the head
until it firmly touches the fixed headboard with the hair compressed. The measurer places her hands on
the child’s legs, gently stretches the child and then keeps one hand on the thighs to prevent flexion.
While positioning the child’s legs, the sliding foot-plate is pushed firmly against the bottom of the child’s
feet. To read the measure, the foot-plate must be perpendicular to the axis of the board and vertical.
The height is read to the nearest 0.1 centimetre.
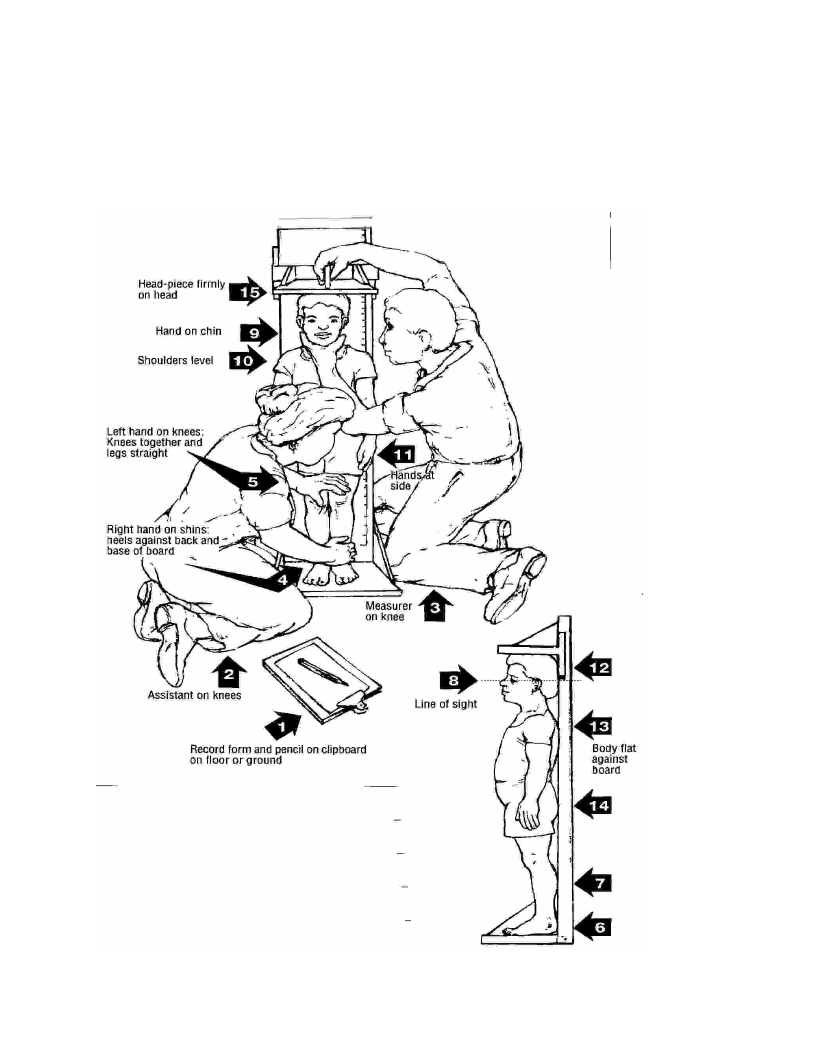
For children more than 87 cm, the measuring board is fixed upright where the ground is level. The child
stands, upright in the middle, against the measuring board. The child’s head, shoulders, buttocks,
knees, heels are held against the board by the assistant, while the measurer positions the head and the
cursor. The height is read to the nearest 0.1 centimetre.
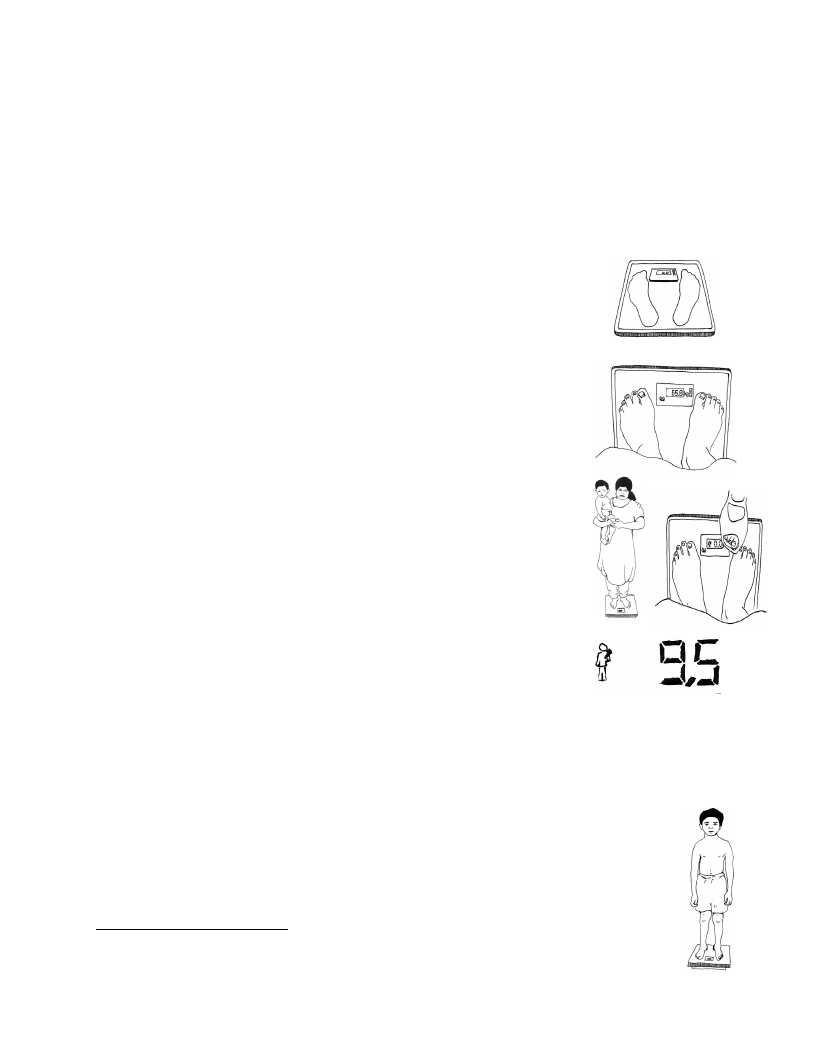
10.4 Weighing a child using a standing scale (or adult scale)1
Where this scale is available, it can be used to accurately measure the child’s weight. Be sure that the
scale is placed on a flat, hard, even surface. There must be enough light to operate the solar-powered
scale.
Explain all procedures to the mother and enlist her help. Babies should be weighed naked; wrap them in
a blanket or other covering until weighing. Older children should be weighed with minimal clothing.
If the child is less than 2 years old, do “mother and child” weighing.
1. To turn on the scale, cover the solar panel for a second. When the number
0.0 appears, the scale is ready.
2. The mother will remove her shoes and step on the scale to be weighed first
alone.
3. Have someone else hold the undressed baby wrapped in a blanket.
4. Ask the mother to stand in the middle of the scale, feet slightly apart (on
the footprints, if marked), and to remain still. The mother’s clothing
must not cover the display or the solar panel. Remind her to stay on the
scale even after her weight appears, until the baby has been weighed in
her arms.
5. With the mother still on the scale and her weight displayed, reboot the
scale by covering the solar panel for a second. The scale is ready when it
displays a figure of a mother and baby, with the number “0.0”.
6. Hand the undressed baby to the mother and ask her to remain still.
7. The baby’s weight will appear on the display (shown to the nearest 0.1
kg). Record this weight.
Note: If a mother is very heavy (e.g. more than 100 kg) and the baby’s weight is
relatively low (e.g. less than 2.5 kg), the baby’s weight may not register on the
scale. In such cases, have a lighter person hold the baby on the scale.
If the child is 2 years or older and will stand still, weigh the child alone. If the child jumps on the scale or
will not stand still, use the “mother and child” weighing procedure instead.
1. Ask the mother to help the child remove shoes and outer clothing. Talk with the child about the
need to stand still.
2. To turn on the scale, cover the solar panel for a second. When the number “0.0” appears, the
scale is ready.
3. Ask the child to stand in the middle of the scale, feet slightly apart (on the footprints, if
marked), and to remain still until the weight appears on the display.
4. Record the child’s weight to the nearest 0.1 kg
1 World Health Organisation - Training Course on Child Growth Assessment.WHO Child Growth Standards.

10.5 Weighing a child using a 25kg Salter Scale
Children are weighed by using a 25 kg hanging sprint scale graduated to 0.100 kg. Do not forget to re-
adjust the scale to zero before each weighing
A plastic washing-basin should be attached by 4 ropes that go underneath the basin. The basin needs to
be close to the ground in case the child falls out, and to make the child feel secure during weighing. If
the basin is dirtied then it should be cleaned with disinfectant. This is much more comfortable and
familiar for the child, can be used for ill children and is easily cleaned. Weighing pants that are used
during surveys should not be used; they are uncomfortable, difficult to use, inappropriate for sick
children and quickly get soiled to pass an infection to the next patient.
When the child is steady, record the measurement to the nearest 100 grams, the frame of the scale
being at eye level. Each day, the scales must be checked by using a known weight.
Annex 11:
Table of Weight-for-height Index, percentage of the median; National Centre for
Health Statistics (NCHS) 1977
Malnutrition
Moderate Severe
Height 100% 85% 80% 75% 70% 60%
in cm in kg in kg in kg in kg in kg in kg
49,0 3,2 2,7 2,6 2,4 2,2 1,9
49,5 3,3 2,8 2,6 2,5 2,3 2,0
50,0 3,4 2,9 2,7 2,6 2,4 2,0
50,5 3,4 2,9 2,7 2,6 2,4 2,0
51,0 3,5 3,0 2,8 2,6 2,5 2,1
51,5 3,6 3,1 2,9 2,7 2,5 2,2
52,0 3,7 3,1 3,0 2,8 2,6 2,2
52,5 3,8 3,2 3,0 2,9 2,7 2,3
53,0 3,9 3,3 3,1 2,9 2,7 2,3
53,5 4,0 3,4 3,2 3,0 2,8 2,4
54,0 4,1 3,5 3,3 3,1 2,9 2,5
54,5 4,2 3,6 3,4 3,2 2,9 2,5
55,0 4,3 3,7 3,5 3,2 3,0 2,6
55,5 4,4 3,8 3,5 3,3 3,1 2,6
56,0 4,6 3,9 3,6 3,5 3,2 2,8
56,5 4,7 4,0 3,7 3,5 3,3 2,8
57,0 4,8 4,1 3,8 3,6 3,4 2,9
57,5 4,9 4,2 3,9 3,7 3,4 2,9
58,0 5,1 4,3 4,0 3,8 3,6 3,1
58,5 5,2 4,4 4,2 3,9 3,6 3,1
59,0 5,3 4,5 4,3 4,0 3,7 3,2
59,5 5,5 4,6 4,4 4,1 3,9 3,3
60,0 5,6 4,8 4,5 4,2 3,9 3,4
60,5 5,7 4,9 4,6 4,3 4,0 3,4
61,0 5,9 5,0 4,7 4,4 4,1 3,5
61,5 6,0 5,1 4,8 4,5 4,2 3,6
62,0 6,2 5,2 4,9 4,7 4,3 3,7
62,5 6,3 5,4 5,0 4,7 4,4 3,8
63,0 6,5 5,5 5,2 4,9 4,6 3,9
63,5 6,6 5,6 5,3 5,0 4,6 4,0
64,0 6,7 5,7 5,4 5,0 4,7 4,0
64,5 6,9 5,9 5,5 5,2 4,8 4,1
65,0 7,0 6,0 5,6 5,3 4,9 4,2
65,5 7,2 6,1 5,7 5,4 5,0 4,3
66,0 7,3 6,2 5,9 5,5 5,1 4,4
66,5 7,5 6,4 6,0 5,6 5,3 4,5
Malnutrition
Moderate Severe
Height 100% 85% 80% 75% 70% 60%
in cm in kg in kg in kg in kg in kg in kg
67,0 7,6 6,5 6,1 5,7 5,3 4,6
67,5 7,8 6,6 6,2 5,9 5,5 4,7
68,0 7,9 6,7 6,3 5,9 5,5 4,7
68,5 8,0 6,8 6,4 6,0 5,6 4,8
69,0 8,2 7,0 6,6 6,2 5,7 4,9
69,5 8,3 7,1 6,6 6,2 5,8 5,0
70,0 8,5 7,2 6,8 6,4 6,0 5,1
70,5 8,6 7,3 6,9 6,5 6,0 5,2
71,0 8,7 7,4 7,0 6,5 6,1 5,2
71,5 8,9 7,6 7,1 6,7 6,2 5,3
72,0 9,0 7,7 7,2 6,8 6,3 5,4
72,5 9,1 7,7 7,3 6,8 6,4 5,5
73,0 9,2 7,8 7,4 6,9 6,4 5,5
73,5 9,4 8,0 7,5 7,1 6,6 5,6
74,0 9,5 8,1 7,6 7,1 6,7 5,7
74,5 9,6 8,2 7,7 7,2 6,7 5,8
75,0 9,7 8,2 7,8 7,3 6,8 5,8
75,5 9,8 8,3 7,8 7,4 6,9 5,9
76,0 9,9 8,4 7,9 7,4 6,9 5,9
76,5 10,0 8,5 8,0 7,5 7,0 6,0
77,0 10,1 8,6 8,1 7,6 7,1 6,1
77,5 10,2 8,7 8,2 7,7 7,1 6,1
78,0 10,4 8,8 8,3 7,8 7,3 6,2
78,5 10,5 8,9 8,4 7,9 7,4 6,3
79,0 10,6 9,0 8,5 8,0 7,4 6,4
79,5 10,7 9,1 8,6 8,0 7,5 6,4
80,0 10,8 9,2 8,6 8,1 7,6 6,5
80,5 10,9 9,3 8,7 8,2 7,6 6,5
81,0 11,0 9,4 8,8 8,3 7,7 6,6
81,5 11,1 9,4 8,9 8,3 7,8 6,7
82,0 11,2 9,5 9,0 8,4 7,8 6,7
82,5 11,3 9,6 9,0 8,5 7,9 6,8
83,0 11,4 9,7 9,1 8,6 8,0 6,8
83,5 11,5 9,8 9,2 8,6 8,1 6,9
84,0 11,5 9,8 9,2 8,6 8,1 6,9
84,5 11,6 9,9 9,3 8,7 8,1 7,0
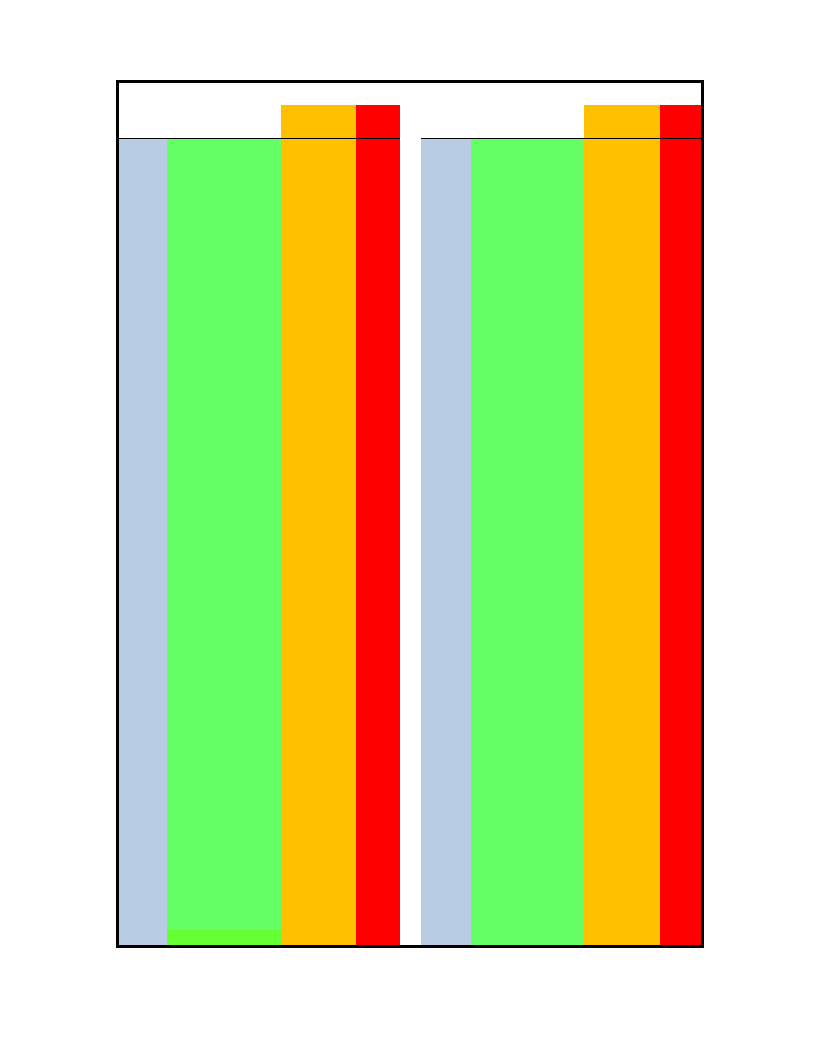
Malnutrition
Moderate Severe
Malnutrition
Moderate Severe
Height 100% 85% 80% 75% 70% 60%
in cm in kg in kg in kg in kg in kg in kg
Height 100% 85% 80% 75% 70% 60%
in cm in kg in kg in kg in kg in kg in kg
85,0 12,0 10,2 9,6 9,0 8,4 7,2
85,5 12,1 10,3 9,7 9,1 8,5 7,3
86,0 12,2 10,4 9,8 9,2 8,5 7,3
86,5 12,3 10,5 9,8 9,2 8,6 7,4
87,0 12,4 10,5 9,9 9,3 8,7 7,4
87,5 12,5 10,6 10,0 9,4 8,8 7,5
88,0 12,6 10,7 10,1 9,5 8,8 7,6
88,5 12,8 10,9 10,2 9,6 9,0 7,7
89,0 12,9 11,0 10,3 9,7 9,0 7,7
89,5 13,0 11,1 10,4 9,8 9,1 7,8
107,5 17,7 15,0 14,2 13,3 12,4 10,6
108,0 17,8 15,1 14,2 13,4 12,5 10,7
108,5 18,0 15,3 14,4 13,5 12,6 10,8
109,0 18,1 15,4 14,5 13,6 12,7 10,9
109,5 18,3 15,6 14,6 13,7 12,8 11,0
110,0 18,4 15,6 14,7 13,8 12,9 11,0
110,5 18,6 15,8 14,9 14,0 13,0 11,2
111,0 18,8 16,0 15,0 14,1 13,2 11,3
111,5 18,9 16,1 15,1 14,2 13,2 11,3
112,0 19,1 16,2 15,3 14,3 13,4 11,5
90,0 13,1 11,1 10,5 9,8 9,2 7,9
90,5 13,2 11,2 10,6 9,9 9,2 7,9
91,0 13,3 11,3 10,6 10,0 9,3 8,0
91,5 13,4 11,4 10,7 10,1 9,4 8,0
92,0 13,6 11,6 10,9 10,2 9,5 8,2
92,5 13,7 11,6 11,0 10,3 9,6 8,2
93,0 13,8 11,7 11,0 10,4 9,7 8,3
93,5 13,9 11,8 11,1 10,4 9,7 8,3
94,0 14,0 11,9 11,2 10,5 9,8 8,4
94,5 14,2 12,1 11,4 10,7 9,9 8,5
95,0 14,3 12,2 11,4 10,7 10,0 8,6
95,5 14,4 12,2 11,5 10,8 10,1 8,6
96,0 14,5 12,3 11,6 10,9 10,2 8,7
96,5 14,7 12,5 11,8 11,0 10,3 8,8
97,0 14,8 12,6 11,8 11,1 10,4 8,9
97,5 14,9 12,7 11,9 11,2 10,4 8,9
98,0 15,0 12,8 12,0 11,3 10,5 9,0
98,5 15,2 12,9 12,2 11,4 10,6 9,1
99,0 15,3 13,0 12,2 11,5 10,7 9,2
99,5 15,4 13,1 12,3 11,6 10,8 9,2
112,5 19,3 16,4 15,4 14,5 13,5 11,6
113,0 19,4 16,5 15,5 14,6 13,6 11,6
113,5 19,6 16,7 15,7 14,7 13,7 11,8
114,0 19,8 16,8 15,8 14,9 13,9 11,9
114,5 19,9 16,9 15,9 14,9 13,9 11,9
115,0 20,1 17,1 16,1 15,1 14,1 12,1
115,5 20,3 17,3 16,2 15,2 14,2 12,2
116,0 20,5 17,4 16,4 15,4 14,4 12,3
116,5 20,7 17,6 16,6 15,5 14,5 12,4
117,0 20,8 17,7 16,6 15,6 14,6 12,5
117,5 21,0 17,9 16,8 15,8 14,7 12,6
118,0 21,2 18,0 17,0 15,9 14,8 12,7
118,5 21,4 18,2 17,1 16,1 15,0 12,8
119,0 21,6 18,4 17,3 16,2 15,1 13,0
119,5 21,8 18,5 17,4 16,4 15,3 13,1
120,0 22,0 18,7 17,6 16,5 15,4 13,2
120,5 22,2 18,9 17,8 16,7 15,5 13,3
121,0 22,4 19,0 17,9 16,8 15,7 13,4
121,5 22,6 19,2 18,1 17,0 15,8 13,6
122,0 22,8 19,4 18,2 17,1 16,0 13,7
100,0 15,6 13,3 12,5 11,7 10,9 9,4
100,5 15,7 13,3 12,6 11,8 11,0 9,4
101,0 15,8 13,4 12,6 11,9 11,1 9,5
101,5 16,0 13,6 12,8 12,0 11,2 9,6
102,0 16,1 13,7 12,9 12,1 11,3 9,7
102,5 16,2 13,8 13,0 12,2 11,3 9,7
103,0 16,4 13,9 13,1 12,3 11,5 9,8
103,5 16,5 14,0 13,2 12,4 11,6 9,9
104,0 16,7 14,2 13,4 12,5 11,7 10,0
104,5 16,8 14,3 13,4 12,6 11,8 10,1
122,5 23,1 19,6 18,5 17,3 16,2 13,9
123,0 23,3 19,8 18,6 17,5 16,3 14,0
123,5 23,5 20,0 18,8 17,6 16,5 14,1
124,0 23,7 20,1 19,0 17,8 16,6 14,2
124,5 24,0 20,4 19,2 18,0 16,8 14,4
125,0 24,2 20,6 19,4 18,2 16,9 14,5
125,5 24,4 20,7 19,5 18,3 17,1 14,6
126,0 24,7 21,0 19,8 18,5 17,3 14,8
126,5 24,9 21,2 19,9 18,7 17,4 14,9
127,0 25,2 21,4 20,2 18,9 17,6 15,1
105,0 16,9 14,4 13,5 12,7 11,8 10,1
105,5 17,1 14,5 13,7 12,8 12,0 10,3
106,0 17,2 14,6 13,8 12,9 12,0 10,3
106,5 17,4 14,8 13,9 13,1 12,2 10,4
107,0 17,5 14,9 14,0 13,1 12,3 10,5
127,5 25,4 21,6 20,3 19,1 17,8 15,2
128,0 25,7 21,8 20,6 19,3 18,0 15,4
128,5 26,0 22,1 20,8 19,5 18,2 15,6
129,0 26,2 22,3 21,0 19,7 18,3 15,7
129,5 26,5 22,5 21,2 19,9 18,6 15,9
130,0 26,8 22,8 21,4 20,1 18,8 16,1
Index weight for height, for children <85cm, length should be measured lying down, , children > 85 cm should be
measured standing up according to the reference data

Admission and discharge criteria for children 6-59 months to TSFP using NCHS (1977)
reference values
TSFP admission criteria
Children 6-59 months
MUAC ≥ 11.0 cm to < 12.0 cm
TSFP discharge criteria
Children 6-59 months
Target weight gain of 13% from admission
weight AND
MUAC ≥ 12.0 for 2 consecutive distributions
Or
WFH ≥ 70% and < 80% of reference median
WFH ≥ 85% of median for two consecutive
distributions
Other discharges (default, died, non-
responder)
The same criteria as for admissions using WHO
Growth Standards (2006) – see page 26 in main
document.

Annex 12: WFH charts for adolescents and adults
Weight-for-height charts for adolescents and adults
Height 100% <-1 SD <-2SD <-3SD
(cm) Median (target) mod Severe
sex
120.5
22.1
18.8
17.7
15.5
mf
121
22.3
19
17.8
15.6
mf
121.5
22.5
19.1
18
15.8
mf
122
22.7
19.3
18.2
15.9
mf
122.5
23
19.5
18.4
16.1
mf
123
23.2
19.7
18.6
16.2
mf
123.5
23.5
19.9
18.8
16.4
mf
124
23.7
20.1
19
16.6
mf
124.5
24
20.4
19.2
16.8
mf
125
24.2
20.6
19.4
16.9
mf
125.5
24.5
20.8
19.6
17.1
mf
126
24.7
21
19.8
17.3
mf
126.5
25
21.2
20
17.5
mf
127
25.3
21.5
20.2
17.7
mf
127.5
25.5
21.7
20.4
17.9
mf
128
25.8
21.9
20.7
18.1
mf
128.5
26.1
22.2
20.9
18.3
mf
129
26.4
22.4
21.1
18.5
mf
129.5
26.7
22.7
21.3
18.7
mf
130
27
22.9
21.6
18.9
mf
130.5
27.3
23.2
21.8
19.1
mf
131
27.6
23.4
22.1
19.3
mf
131.5
27.9
23.7
22.3
19.5
mf
132
28.2
24
22.5
19.7
mf
132.5
28.5
24.2
22.8
19.9
mf
133
28.8
24.5
23
20.2
mf
133.5
29.1
24.7
23.3
20.4
mf
134
29.4
25
23.5
20.6
mf
134.5
29.7
25.3
23.8
20.8
mf
135
30.1
25.6
24.1
21.1
mf
135.5
30.4
25.8
24.3
21.3
mf
136
30.7
26.1
24.6
21.5
mf
136.5
31
26.4
24.8
21.7
mf
137
31.4
26.7
25.1
22
mf
137.5
31.7
27
25.4
22.2
mf
138
32.1
27.2
25.6
22.4
mf
138.5
32.4
27.5
25.9
22.7
mf
139
32.7
27.8
26.2
22.9
mf
139.5
33.1
28.1
26.4
23.1
mf
140
33.4
28.4
26.7
23.4
mf
140.5
33.7
28.7
27
23.6
mf
Height 100% < -1SD <-2SD <-3SD
(cm) Median (target) mod Severe
sex
151.5
41.3
35.1
33.1
28.9
mf
152
41.7
35.4
33.4
29.2
mf
152.5
42.1
35.8
33.7
29.4
mf
153
42.4
36.1
34
29.7
mf
153.5
42.8
36.4
34.3
30
mf
154
43.2
36.7
34.6
30.2
mf
154.5
43.6
37.1
34.9
30.5
mf
155
44
37.4
35.2
30.8
mf
155.5
44.2
37.6
35.4
30.9
mf
156
44.6
37.9
35.7
31.2
mf
156.5
45
38.2
36
31.5
mf
157
45.4
38.6
36.3
31.8
mf
157.5
45.8
38.9
36.7
32.1
mf
158
46.2
39.3
37
32.4
mf
158.5
46.6
39.6
37.3
32.7
mf
159
47.1
40
37.7
33
mf
159.5
47.5
40.4
38
33.3
mf
160
48
40.8
38.4
33.6
mf
160.5
48.4
41.1
38.7
33.9
mf
161
48.8
41.5
39.1
34.2
mf
161.5
49.3
41.9
39.4
34.5
mf
162
49.8
42.3
39.8
34.8
mf
162.5
50.2
42.7
40.2
35.1
mf
163
50.7
43.1
40.5
35.5
mf
163.5
51.1
43.5
40.9
35.8
mf
164
51.6
43.9
41.3
36.1
mf
164.5
52.1
44.3
41.7
36.5
mf
165
52.6
44.7
42.1
36.8
mf
165.5
53.1
45.1
42.5
37.2
mf
166
53.6
45.6
42.9
37.5
mf
166.5
54.1
46
43.3
37.9
mf
167
54.6
46.4
43.7
38.2
mf
167.5
55.1
46.9
44.1
38.6
mf
168
55.6
47.3
44.5
38.9
mf
168.5
56.2
47.7
44.9
39.3
mf
169
56.7
48.2
45.4
39.7
mf
169.5
57.3
48.7
45.8
40.1
mf
170
57.8
49.2
46.3
40.5
mf
170.5
58.4
49.6
46.7
40.9
mf
171
59
50.1
47.2
41.3
mf
171.5
59.6
50.6
47.6
41.7
mf

Annex 13
Referral Form: OTP to TSFP or TSFP to OTP
Referral: Health Facility/distribution site
DATE:
CHILD'S NAME: ________________________
CARER'S NAME: ________________________
AGE (months): ________________________
KEBELE:
________________________
GOTT:
________________________
REFERRED BY: ________________________
From
MUAC
OEDEMA
WEIGHT
____________________ To__________________
__________ cm________
YES
NO
__________ kg
HEIGHT
__________ cm
W/H Z-score __________
COMMENT: _________________________________
SIGNATURE __________________________________
Referral: Health Facility/distribution site
DATE:
CHILD'S NAME: ________________________
CARER'S NAME:
AGE (months):
KEBELE:
________________________
________________________
________________________
GOTT:
________________________
REFERRED BY: ________________________
From
MUAC
OEDEMA
WEIGHT
HEIGHT
____________________ To__________________
__________ cm________
YES
NO
__________ kg
__________ cm
W/H Z-score __________
COMMENT: _________________________________
SIGNATURE __________________________________
Referral: Health Facility/distribution site
DATE:
CHILD'S NAME: ________________________
CARER'S NAME: ________________________
AGE (months): ________________________
KEBELE:
________________________
GOTT:
________________________
REFERRED BY: ________________________
From
MUAC
OEDEMA
WEIGHT
____________________ To__________________
__________ cm________
YES
NO
__________ kg
HEIGHT
__________ cm
W/H Z-score __________
COMMENT: _________________________________
SIGNATURE __________________________________
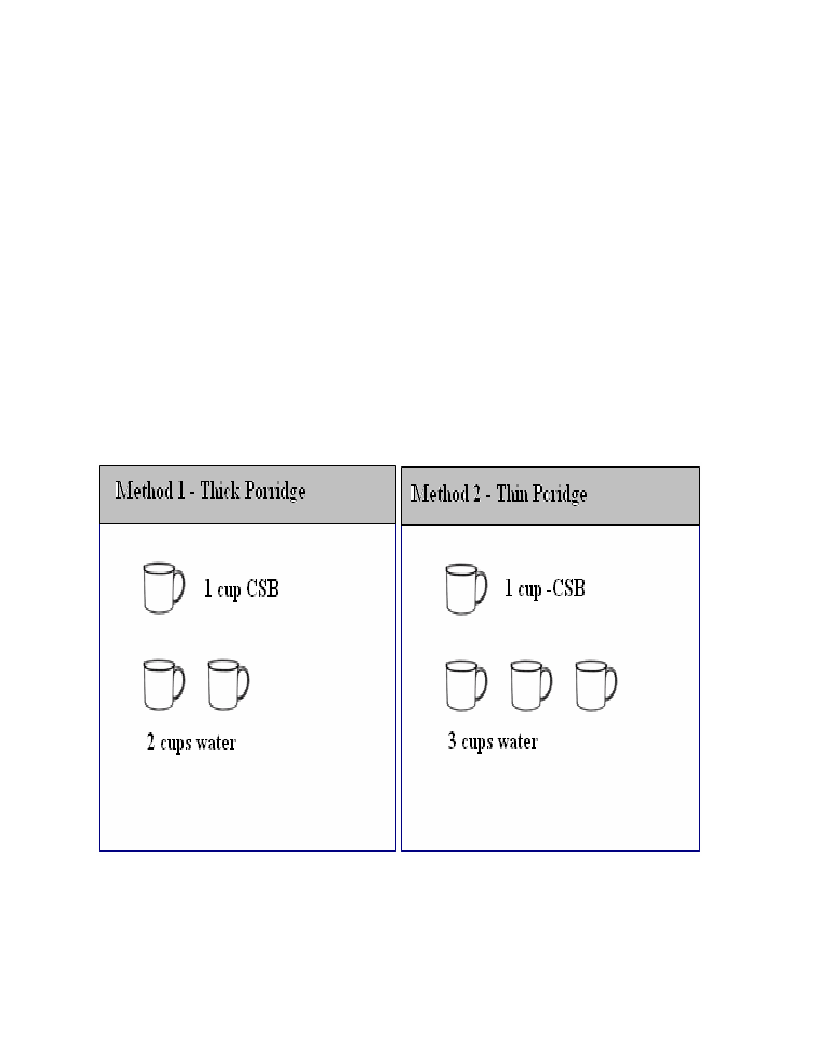
Annex 14: How to prepare premixed CSB+ or other Fortified Blended Food (FBF)
• Ensure that the water being used for cooking is safe before starting to cook
• Wash your hands with soap before you start to prepare the porridge
• Mix the premixed CSB+ (Famix, UNIMIX, Faffa) with part of the cold water to make a paste
• Add the rest of the water and bring to boil – ensure that it is not boiled for any longer than 10
minutes
• Where possible and resources allow, add additional oil, sugar, milk products, seasonal fruits
and/or local nuts to increase the energy density and improve the taste
• Serve on a clean plate or bowl
• Wash the child’s face and hands with water and soap before eating
• Use a separate plate for the child
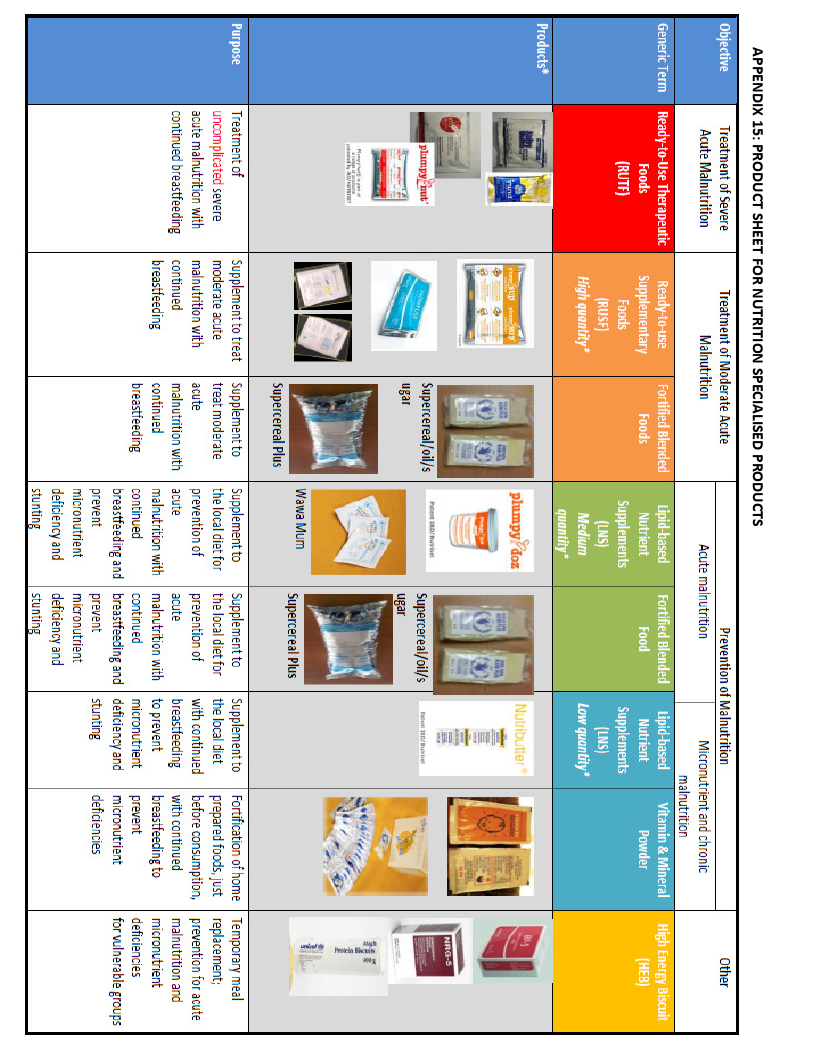
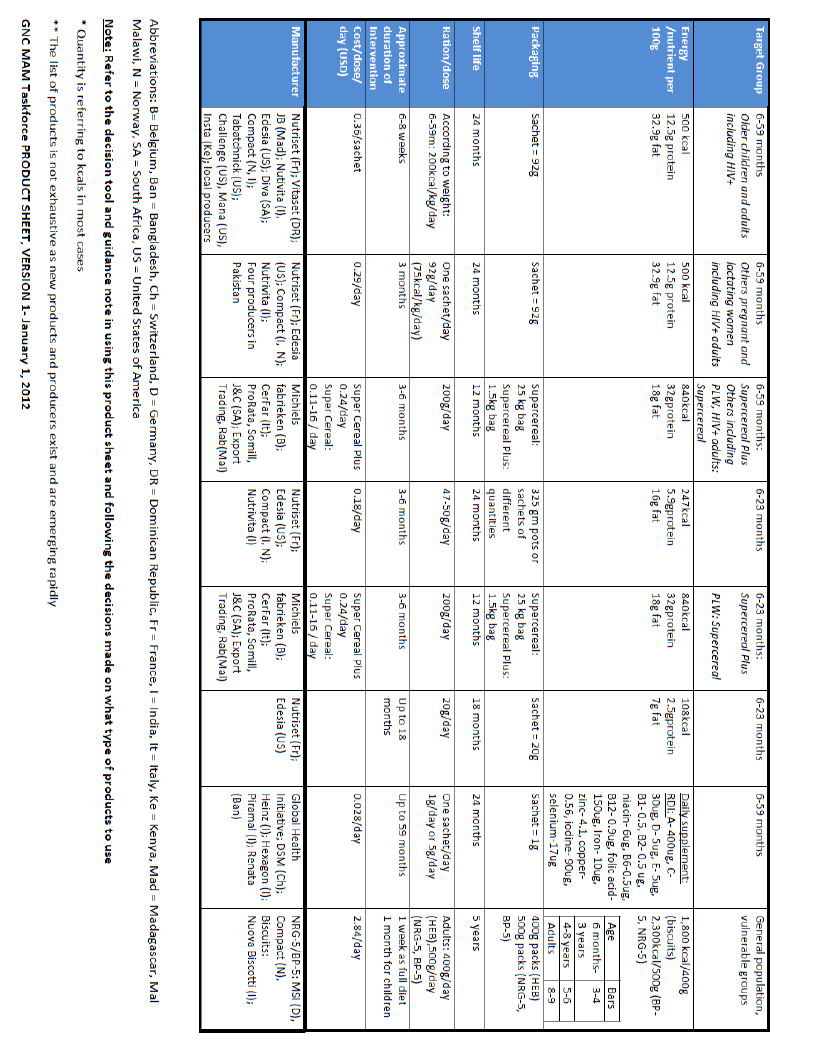
Annex 16: Target weight for
discharge
This table gives the target weight for discharge for MAM children 6-59 months admitted to TSFPs
using MUAC admission criteria (≥ 11.0 cm - < 12.0 cm)
The target weight is calculated as 13% increase in body weight from admission weight
Admission Discharge
Admission Discharge
Admission
Weight
Weight
Weight
Weight
Weight
(kgs)
(kgs)
(kgs)
(kgs)
(kgs)
Discharge
Weight
(kgs)
3
3.4
7.1
8.0
11.2
12.7
3.1
3.5
7.2
8.1
11.3
12.8
3.2
3.6
7.3
8.2
11.4
12.9
3.3
3.7
7.4
8.4
11.5
13.0
3.4
3.8
7.5
8.5
11.6
13.1
3.5
4.0
7.6
8.6
11.7
13.2
3.6
4.1
7.7
8.7
11.8
13.3
3.7
4.2
7.8
8.8
11.9
13.4
3.8
4.3
7.9
8.9
12
13.6
3.9
4.4
8
9.0
12.1
13.7
4
4.5
8.1
9.2
12.2
13.8
4.1
4.6
8.2
9.3
12.3
13.9
4.2
4.7
8.3
9.4
12.4
14.0
4.3
4.9
8.4
9.5
12.5
14.1
4.4
5.0
8.5
9.6
12.6
14.2
4.5
5.1
8.6
9.7
12.7
14.4
4.6
5.2
8.7
9.8
12.8
14.5
4.7
5.3
8.8
9.9
12.9
14.6
4.8
5.4
8.9
10.1
13
14.7
4.9
5.5
9
10.2
13.1
14.8
5
5.7
9.1
10.3
13.2
14.9
5.1
5.8
9.2
10.4
13.3
15.0
5.2
5.9
9.3
10.5
13.4
15.1
5.3
6.0
9.4
10.6
13.5
15.3
5.4
6.1
9.5
10.7
13.6
15.4
5.5
6.2
9.6
10.8
13.7
15.5
5.6
6.3
9.7
11.0
13.8
15.6
5.7
6.4
9.8
11.1
13.9
15.7
5.8
6.6
9.9
11.2
14
15.8
5.9
6.7
10
11.3
14.1
15.9
6
6.8
10.1
11.4
14.2
16.0
6.1
6.9
10.2
11.5
14.3
16.2
6.2
7.0
10.3
11.6
14.4
16.3
6.3
7.1
10.4
11.8
14.5
16.4
6.4
7.2
10.5
11.9
14.6
16.5
6.5
7.3
10.6
12.0
14.7
16.6
6.6
7.5
10.7
12.1
14.8
16.7
6.7
7.6
10.8
12.2
14.9
16.8
6.8
7.7
10.9
12.3
15
17.0
6.9
7.8
11
12.4
15.1
17.1
7
7.9
11.1
12.5
15.2
17.2
Admission
Weight
(kgs)
15.3
15.4
15.5
15.6
15.7
15.8
15.9
16
16.1
16.2
16.3
16.4
16.5
16.6
16.7
16.8
16.9
17
17.1
17.2
17.3
17.4
17.5
17.6
17.7
17.8
17.9
18
18.1
18.2
18.3
18.4
18.5
18.6
18.7
18.8
18.9
19
19.1
19.2
19.3
Discharge
Weight
(kgs)
17.3
17.4
17.5
17.6
17.7
17.9
18.0
18.1
18.2
18.3
18.4
18.5
18.6
18.8
18.9
19.0
19.1
19.2
19.3
19.4
19.5
19.7
19.8
19.9
20.0
20.1
20.2
20.3
20.5
20.6
20.7
20.8
20.9
21.0
21.1
21.2
21.4
21.5
21.6
21.7
21.8

Annex 17
Discussion of target weight gain as the discharge criteria for MUAC admissions
When considering the ‘best’ criteria to use for the discharge of MAM children, a number of
questions usually arise. The recommendations for discharge using a target weight gain of 13% have
been based on the following reasons:
1) When admitting using MUAC it is not advisable to discharge on WFH z-scores
This is because WFH and MUAC are 2 different tools, which have the potential to identify 2 different
groups of children. While there is some overlap, MUAC preferentially selects younger children and
those who are at a higher risk of mortality. Because these tools have some, but limited correlation,
some of the children with a MUAC <12.0 cm, are likely to be ≥ -2 z-scores on admission. This could
result in a child being admitted one week, discharged the next, and so on.
2) If MUAC is good to use for admission, then it should be used for discharge also
As yet, there is insufficient evidence available that suggests MUAC responds quickly and accurately
enough to treatment. So if a child has a MUAC of e.g. 11.6 cm on admission, does reaching 12.0 cm,
12.2cm or 12.5 cm constitute recovery? How long will this take? Do children respond in a similar
enough way to define cut-offs for recovery? The current thinking (internationally) is that more
evidence is required on how MUAC responds to treatment before it can be adopted as a discharge
criterion in its own right. This is the reason why target percentage weight gain was introduced for
SAM cases identified through MUAC. It is a logical process therefore, to apply similar reasoning to
the recovery of MAM cases.
3) Is 13% weight gain a reasonable target weight gain to define ‘recovery’ for MAM children
The target weight gain for recovery of SAM children in OTP was classified as 15% through
international recommendations from WHO and UNICEF during 2008. It is logical therefore to
recommend that MAM children should have a lower target weight gain, as the children were less
malnourished to begin with. It is therefore recommended that 13% target weight gain should be
used as the discharge criteria for all MUAC admissionsto TSFP for children 6-59 months. As this
discharge criterion has not yet been thoroughly tested in Ethiopia, it is also recommended that
research is conducted to assess whether target weight gain is appropriate, and whether 13% is the
ideal weight gain to define recovery of MAMthat was identified by MUAC.

Annex 18: Home Visit Form
Volunteer / Community Worker’s Name: ________________
Date of Visit: ______________
Beneficiary name:_______________Kebele:__________________Gott:____________________
Feeding Practices
Is the supplementary food ration present in the home
If not, where is the ration?
Is the available ration enough to last until the next SFP
distribution?
Is the food ration being shared or eaten only by the beneficiary?
Yes
Yes
Shared
No
No
Beneficiary only
Is the child/beneficiary given other foods in addition to the ration? Yes
No
If yes, what type of food?
How many times per day is the child given food to eat?
Does someone help/encourage the child to eat?
Yes
No
What does the caregiver do if the child does not want to eat?
Is the child currently breastfeeding? (for children < 2yrs)
Yes
No
Is clean water available?
Yes
No
Caring Practices
Are both parents alive and healthy?
Who cares for the child during the day?
Is the child clean?
Yes
No
Health
What is the household’s main source of water?
Is there soap for washing in the house?
Yes
No
Does the caregiver wash the child’s hands and face before
feeding?
Yes
No
Is food covered and protected from flies?
Yes
No
What action does the caregiver take when the child has diarrhoea?
Food Security
Does the household currently have food available?
Yes
No
What is the most important source of income for the household?
Is the household registered for PSNP?
Does the household receive any other form of external support?

Annex 19: Post Distribution Monitoring (PDM) questionnaire for TSFP beneficiaries.
Kebele: ________________ Gott: ___________________
Date: ______________
PSNP: yes:
no:
1. What do you understand as the reason for receiving your/your child’s supplementary food?
2. What are the advantages of receiving this supplementary food?
3. How was the supplementary food that you received last distribution used?
Use proportional piling techniques to assess
Use of food
Eaten within
household
Shared outside Sold
household
%
Other
(explain)
4. If any supplementary food was sold or exchanged what was bought/received in return?
5. How was the supplementary food that you received last distribution prepared?
Porridge
(thick)
Gruel
(thin)
Bread
Other: _____________
6. Who consumed the supplementary food you received last distribution?
Only the beneficiary registered in the SFP
The beneficiary registered in the SFP and other children in the family
The beneficiary registered in the SFP and other adults in the family
All the children and the adults in the family
Other: _________________________________
7. For how long does the supplementary food ration last? _______________________________
8. Do you have any comments on the quality of the supplementary food?___________________

Annex 20: Planning and Analysing Focus Group Discussions
Source: Community-based Therapeutic Care (CTC): A field Manual. VALID International. First Edition,
2006
Focus group discussions (FGDs) are a valuable tool for assessing community perceptions and different
aspects of the TSFP. There is a growing body of data and publications on how to conduct FGDs. Some of
the key issues are covered below:
Planning a Focus Group Discussion (FGD)
The effectiveness of FGDs, as well as the quality of their results, depends partly on the preparation
beforehand.
Prepare a script:
Have a mix of general and specific questions. Make sure that each question has a number of ‘probe’
questions to follow up with, as they may help clarify responses. Consider asking participants for
definitions (e.g. what is malnutrition?), impressions (e.g. are the children in the programme improving?)
and their idea of other people’s perceptions (e.g. what does the rest of the community think about the
TSFP?). Ask a broad range of questions so that related issues can be explored if they arise.
Develop a ‘questioning route’:
When drafting a questioning route, consider the type of information you want, and who can provide the
information.
Know your setting:
Who are the participants? How will you recruit them?
What questions will you ask? How will you moderate the groups and collect the data?
Conducting a FGD
Keep in mind how the findings will be used:
Avoid asking questions that you will not be able to act on or incorporate into your report. Similarly, be
cautious of raising participants’ expectations with the questions e.g. (what does the community need?)
Ask questions that draw people out:
Follow up questions can be used such e.g. can you give an example? Where do you think this
impression comes from? Encourage participants to voice their opinions, while using questions to
prevent individual members from dominating the discussions (e.g. do the rest of you agree with x’s
opinion? Does anyone have a different experience or opinion?).

Put a time limit on the FGD session:
Setting a time limit helps the moderator to cover the planned topic areas. Remember that it will take
about three times longer to transcribe the session.
Notice non-verbal interactions:
Body language, reluctance or eagerness to speak, dynamics between group members and their effect on
opening or shutting down conversations.
Keep the conversation flowing:
Encourage all participants to say whatever is on their minds. If they stray off the subject for too long, or
get ahead of the issues being discussed, the moderator must re-focus the discussion.
Try to be neutral:
Some of the participants may not like the topic being discussed. They should be actively encouraged to
voice their opinions. In such instances, ask what it is that participants like and do not like about the
subject and where solutions may lie.
Analysing the Results
• Interpret how participants talk about certain issues, as well as the information they give.
• Interpret non-verbal communication and reactions as well as the verbal interaction.
• Bear in mind that information from FGDs is group information and is not necessarily the same as
information obtained in individual interviews. It reflects collective ideas shared and negotiated
by the group. Caution is needed when making general claims extrapolated from FGD data.
Annex 21: Pictorial Guide for conducting CSAS coverage surveys1
Step 1: Find a Map
The first step in the new coverage estimation method is to find a map of the program area. Try to find a
map showing the location of town and villages. A map of 1:50,000 scale is ideal.
Step 2: Draw a grid
The next step is to draw a grid over the map. The size of each square should be small enough for it to be
reasonable to assume that coverage will be similar throughout the square. A square of 10km by 10km
will probably be small enough in most circumstances.
Step 3: Select the squares to sample
Select the squares with about 50% or more of their area inside the program area.
Step 4: Select the communities to sample
Select the community closest to the centre of each square. If prevalence is low then you might need to
select more than one community from each square. Select the communities closest to the centre of
each square. Select the communities to be sampled and the order in which they should be sampled in
advance of visiting the square.
Step 5: Case-finding
When you visit a community find cases using an active case-finding method. It is usually sufficient to ask
community health workers, traditional birth attendants, traditional healers or other key informants to
take you to see "children who are sick, thin, or have swollen legs or feet" and then ask mothers of
confirmed cases to help you find more cases. You could also use door-to-door screening. It is important
that the case-finding method that you use finds all, or nearly all, cases in the sampled communities.
Each case is confirmed by applying the program's entry criteria (e.g. < 70% of the median weight-for-
height from the NCHS reference population and /or bilateral pitting oedema). When you find a
confirmed case you should then find out whether that child is in the programme. Remember to follow-
up on children reported to be in a therapeutic feeding centre or at a distribution point on the day of the
survey
Step 6: Record the data
You need only record the number of cases found and the number of those that are in the program for
each sampled square.
Step 7: Calculate coverage
Coverage is calculated as the number of cases that you found that are in the program divided by the
number of cases that you found. You should calculate this separately for each square as well as for all of
the squares together. You could use a weighted method to calculate the coverage for all of the squares
combined but this is not essential.
Step 8: Plot the data
Coverage data is plotted as a mesh map and as a histogram. The length of the
sides of the filled squares on the mesh map reflects the level of coverage found in
each square (calculated in step 7). The small open squares indicate quadrats
(squares of approximately equal area) with zero coverage. You might find it
helpful to mark the location of feeding centres, distribution points, health posts,
and roads on the map. This will help you interpret the results of the coverage
survey.
1 Myatt M, New Method for Estimating Programme Coverage, Field Exchange, Emergency Nutrition Network, 2004;21:11

Annex 22: Guiding Principles on IYCF in Emergencies
Source: A guide for Selective Feeding Programmes, UNHCR/WFP. Geneva, May, 2009.
Breastfeeding
Breastmilk
substitutes
Complementary
feeding
Caring for
caregivers
Protecting children
Malnutrition
The acute phase of
emergencies
Assessment,
intervention and
monitoring
Principle 1: Infants born into populations affected by emergencies
should normally be exclusively breastfed from birth to 6 months of age.
Principle 2: The aim should be to create and sustain an environment
that encourages frequent breastfeeding for children up to two years or
beyond.
Principle 3: The quantity, distribution and use of breastmilk substitutes
at emergency sites should be strictly controlled.
Principle 4: To sustain growth, development and health, infants from 6
months onwards and older children need hygienically prepared and
easy-to-eat, digestable foods that nutritionally complement breastmilk.
Principle 5: Caregivers need secure uninterrupted access to appropriate
ingredients with which to prepare and feed nutrient-dense foods to
older infants and young children.
Principle 6: Because the number of caregivers is often reduced during
emergencies as stress levels increase, promoting caregivers’ coping
capacity is an essential part of fostering good feeding practices for
infants and young children.
Principle 7: The health and vigour of infants and children should be
protected so they are able to suckle frequently and well and maintain
their appetite for complementary foods.
Principle 8: Nutritional status should be continually monitored to
identify malnourished children so that their condition can be assessed
and treated, and prevented from deteriorating further. The underlying
causes of malnutrition should be investigated and corrected.
Principle 9: To minimise an emergency’s negative impact on feeding
practices, interventions should begin immediately. The focus should be
on supporting caregivers and channeling scarce resources to meet the
nutritional needs of the infants and young children in their charge.
Principle 10: Promoting optimal feeding for infants and young children
in emergencies requires a flexible approach based on continual careful
monitoring.
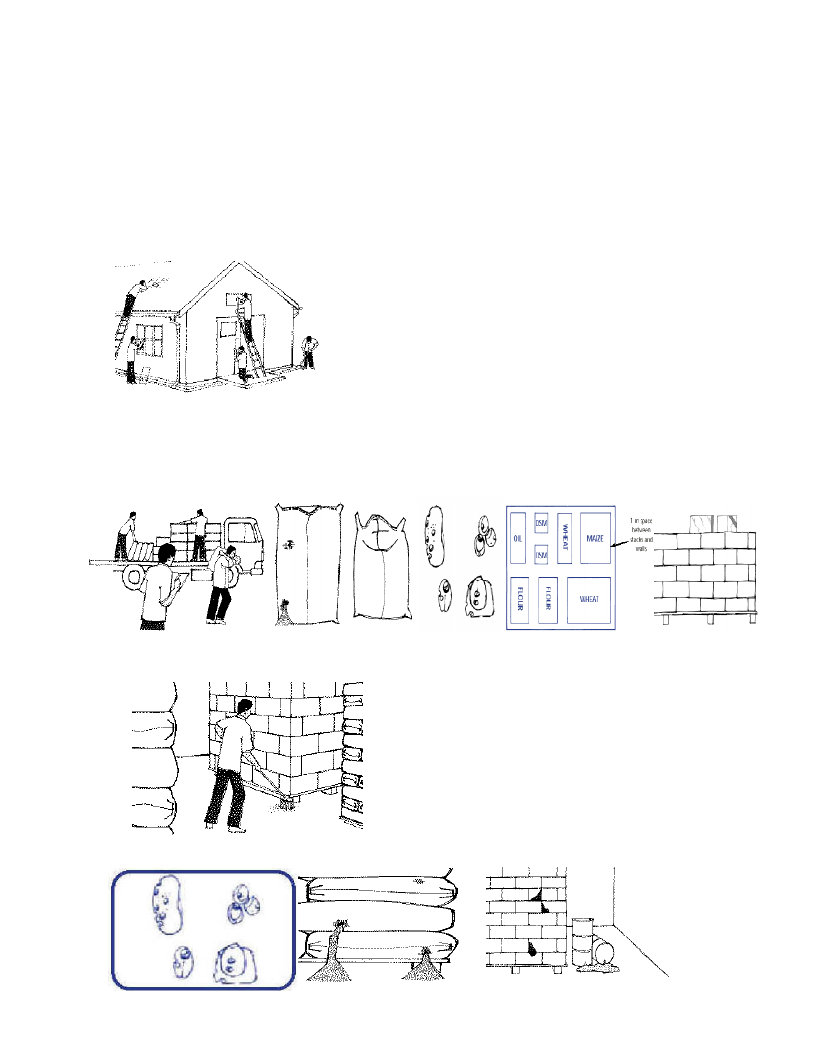
Annex 23
Warehouse Management: General Store Keeping
Objective:
• accounting of what has been received, stored and issued
• maintaining the quality of the food and minimizing looses
Standard Practices:
1. Receiving, storing and dispatching of food and Non Food Items
• Counting when receiving and issuing
• Checking, conditions of what is received, stored & issued
• Keeping records(remarks)
2. Store and store premises:Checking any damages of sections of store, repair, ensure adequate lighting, arrange security guarding,
and ensure padlocking.
3. Standard food handling and stacking(depending store size ,keep 40-100 cm space, distance from wall & in between
stacks)
• Counting
• Careful unloading
• Inspect for damages, record remarks
• Proper stacking
1. Cleaning and ventilating the store(s):cleaning and ventilating the store, daily, weekly and periodical thorough store
cleaning is mandatory
2.
3. Inspection of stocks and store: periodically make inspection, look for physical damages(insect damage), staining caused
by leakages ,water and evidence of theft and report findings,
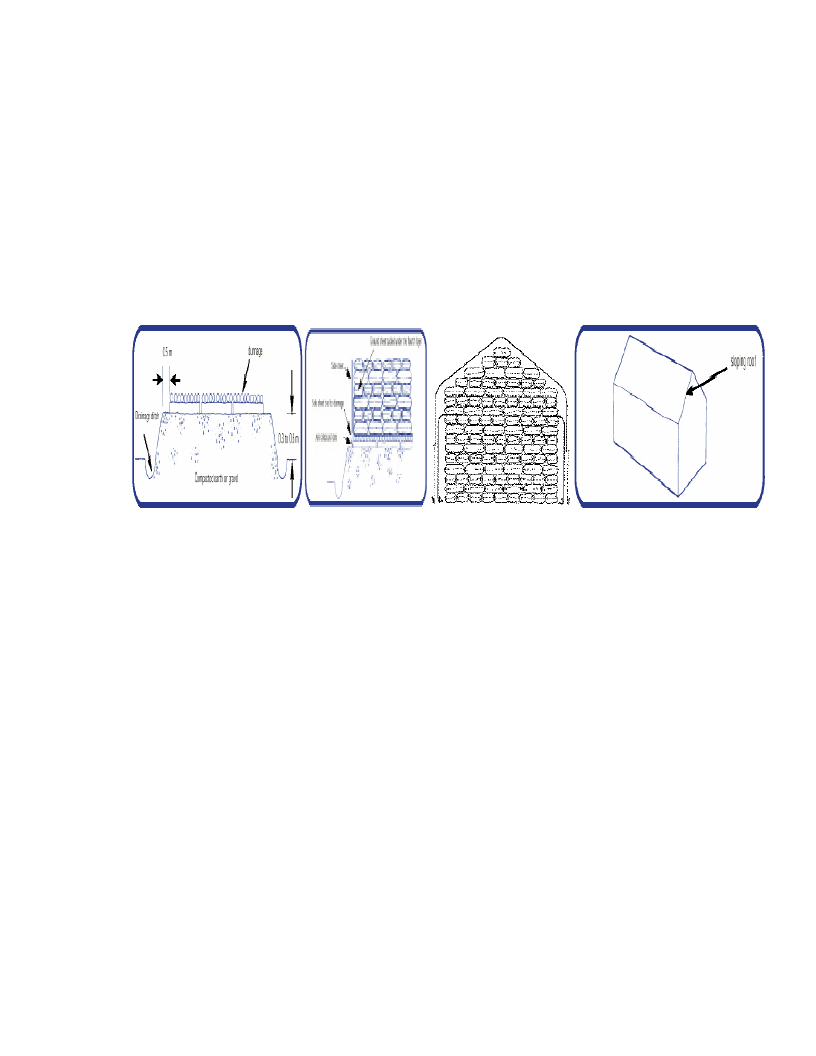
4. Stock rotations: oldest stock should be issued first - First in, first out (FIFO).
5. Waste disposal: spillage and sweeping,
• Grain and pulses spilled onto a clean floor are usually not waste – they may be re-bagged, after cleaning by
sieving if necessary - but small quantities of dirty spilt grain should be destroyed.
• Spilled flour and blended food are normally waste.
Note: that spoiled commodities are still the responsibility of the storekeeper until properly disposed of, and must be
accounted for in the records.
6. Pest Control:
• Insecticides and fumigants to control insects, and rodenticides to control rats and mice are dangerous to
human health and should only be used by trained staff.
• Regular inspections of the stock will give early warning of attack by these pests and of the need for control.
7. Temporary Outdoor Storage (outdoor stacks):Only whole-grain cereals and pulses, and for vegetable oil can be temporarily stored in
outside store,
N.B. Should never be used to store flour, blended food, milk powder or canned food.
Effective outside storage needs: a prepared stacking platform; should have dunnage and a waterproof groundsheet;_ waterproof covers
(tarpaulins);ropes for tying down tarpaulins.
8. Documentation and Record keeping: overall objectiveis to provide a commodity tracking system from
first receipt to final discharge. Main documents includes,
• Waybills, sometimes known as delivery notes: Signing a waybill is a formal acceptance of the consignment; therefore, it
is important to check that the consignment matches exactly the description on the waybill.
• Stack cards - record any movement into or out of the stack and display the current stock level,
• Warehouse ledgers (or stock cards) provide an overview of the total stock position in the warehouse.
• Stock-taking or physical audit forms record the result ofindependent physical checks on stock levels.
• Loss or damaged cargo reports - provide full details of the problem and any action taken to repackage or reconstitute.
• Inspection reports provide full details of the condition of the warehouse or the commodity.
• Certificate of destruction describes authorised action taken to destroy or dispose of unfit commodities.
• When a final distribution report is made to the donor it will be supported by copies of many of the above documents.
BASIC WAREHOUSE EQUIPMENT THAT HELPS TO KEEP IT CLEAN AND TO THE STANDARD
• Brooms
• Ladders
• Repackaging equipment e.g. sack needles and twine (orstitching machine), empty sacks, cartons, oil containers,
• adhesive tape
• Sampling spears
• Shovels
• Sieves
• Torch
• Weighing scales
N.B. Fire extinguishers and First aid box if available




